-
乳腺癌是女性恶性肿瘤患者主要的死亡原因之一[1],是城市地区女性最常见的恶性肿瘤,其发病率已居女性恶性肿瘤的首位[2]。乳腺癌常出现骨转移灶,引起一系列的症状和体征(如骨痛、病理性骨折等),严重影响患者的生活质量和生存状况。99Tcm-MDP全身骨显像发现骨病灶的灵敏度较高而特异度较低;联合MRI增强检查后能明显提高骨转移灶的早期诊断及鉴别诊断准确率[3]。SPECT/CT融合显像在提供精确的解剖定位的同时,还可显示病灶的特征性影像学改变。对鉴别诊断颅骨良恶性病变有较高的灵敏度和特异度[4]。
本研究回顾性分析了我院核医学科乳腺癌患者行SPECT/CT融合显像的临床资料,探讨SPECT/CT融合显像在诊断和鉴别全身骨显像异常放射性浓聚灶性质中的临床价值。
-
收集2011年10月至2013年1月在我院经病理学确诊的乳腺癌患者25例,年龄34~81岁,平均年龄为51.3岁。所有患者99Tcm-MDP全身骨显像显示骨骼中有一个或多个异常放射性浓聚灶,即刻行SPECT/CT融合显像。在初次检查后4~8个月再次行99Tcm-MDP全身骨显像及SPECT/CT融合显像检查。所有患者均于检查前签署了知情同意书。
-
采用德国西门子公司SYMBIA T2双探头SPECT/CT仪,配低能高分辨平行孔准直器。99Tcm-MDP由广州原子高科股份有限公司提供,每支活度为555~925 MBq。
-
检查前所有患者无需特殊准备,按体重经右肘静脉注射99Tcm-MDP 555~925 MBq。嘱患者在注射显像剂后30 min至显像前,饮水1500 ml以上,并尽量排尽尿液。排尿时避免尿液污染皮肤衣物,污染患者检查前需更换干净衣物。
-
于注射99Tcm-MDP后3 h行全身骨显像,患者仰卧位平躺于检查床上,双臂自然放于身体两侧。采用低能高分辨平行孔准直器,双探头SPECT/CT前后位连续采集图像。采集条件为:能峰140 keV,窗宽20%,矩阵256×1024,连续采集模式,双探头采集,采集速度为20 cm/min。采集完成后即刻判读影像结果。
-
患者保持全身骨显像时的体位不变,以全身骨显像显示的判读为骨转移可能性较大的放射性浓聚灶为中心行99Tcm-MDP SPECT/CT融合显像。CT采集条件:电压130 kV,电流100 mA,矩阵512×512。SPECT采集条件:低能高分辨平行孔准直器,能峰140 keV,窗宽20%,矩阵128×128,身体自动轮廓跟踪,双探头同时采集32个视野,每个视野采集20 s。所有采集的图像应用德国西门子公司Syngo工作站e.soft软件处理。CT图像采用B60卷积核进行骨窗重建,层厚3 mm;SPECT图像采用有序子集最大期望值法处理及Flash-3D重建,获得冠状位、矢状位、横断位断面的影像。采用对象与目标矩阵法进行断层图像的配准与同机图像融合。
-
全身骨显像判读标准[5]:①全身骨显像出现多发、散在的异常放射性浓聚灶;②单个放射性浓聚灶经其他影像学方法初步排除良性病变者,判读为肿瘤骨转移病灶可能性大。对所有病灶都进行病理学检查不切实际,因此4~8个月后复诊时我们的判读依据:若出现临床症状加重,原病灶于SPECT/CT、CT和(或)MRI等影像学表现进展,如病灶范围扩大、出现成骨或溶骨性变化、放射性浓聚度加重或出现新病灶等而无其他原因解释者均视为肿瘤骨转移确诊。
所有影像均由两名有经验的核医学科医师进行分析,意见有分歧则共同协商,统一结论;对部分难以明确判断的CT影像咨询放射科医师的意见。
-
为评估全身骨显像与SPECT/CT的诊断效能,将所有放射性浓聚灶根据判断为恶性可能性的大小分为5级:1级为肯定为恶性病灶;2级为恶性可能性比较大;3级为不能确定良恶性质;4级为良性可能性比较大;5级为肯定为良性病灶。利用ROC进行分析。
-
采用SPSS 17.0软件进行统计学分析。配对计数资料和等级资料采用卡方检验,以P<0.05为差异有统计学意义。
-
在25例乳腺癌患者的初次全身骨显像中,发现37个放射性异常浓聚灶。患者的病灶数分别为:17例患者有1个病灶,5例患者有2个病灶,2例患者有3个病灶,仅1例患者有4个病灶。大部分患者的放射性浓聚灶均表现为单发灶。
全身骨显像不同部位的病灶数目为椎体20(54.05%)个、肋骨5(13.51%)个、骨盆4(10.81%)个、锁骨3(8.11%)个、头颅及胸骨均为2(5.41%)个、肩胛骨1(2.70%)个。显示大部分病灶分布于椎骨、肋骨及骨盆骨,以椎骨较多见。在全身骨显像中,对37个放射性异常浓聚灶判读为恶性的31个,良性的6个。在初次SPECT/CT融合显像中,初步判定骨转移灶28个,良性病灶9个。
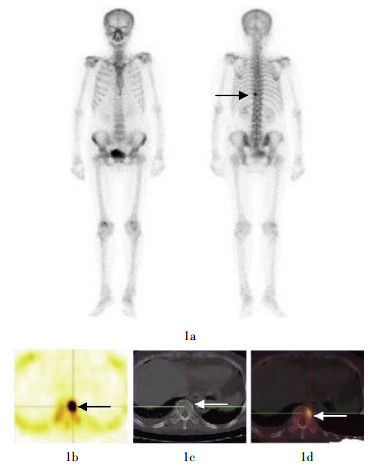
25例患者在4~8个月后接受了全身骨显像及SPECT/CT融合显像复查。重新判读初次检查发现的37个放射性异常浓聚灶中,有29个确诊为骨转移灶(图 1),其中有2个椎体病灶初次检查中判读为良性病灶;8个病灶确诊为良性,其中有1个肋骨病灶在初次检查中被判读为骨转移;比较全身骨显像与SPECT/CT融合显像结果,在检出病灶方面二者间的差异具有统计学意义(χ2=6.975,P<0.05)。良性病灶主要出现在椎体和肋骨部。

图 1 患者女性,53岁,乳腺癌。图中,1a:99Tcm-MDP全身骨显像,示T10椎体左缘单个异常放射性浓聚灶(箭头所示);1b~1d:该病灶的SPECT、CT和SPECT/CT融合显像的横断位图像,CT示T10椎体有放射性浓聚灶并且局部骨质破坏;SPECT与CT融合图像提示异常放射性浓聚灶为乳腺癌T10椎体骨转移灶。
全身骨显像和SPECT/CT融合显像的诊断灵敏度、特异度、阳性预测值、阴性预测值和准确率分别为82.76%、75.00%、92.31%、54.55%、81.08%和93.10%、87.50%、96.43%、77.78%、91.89%。
对全身骨显像及SPECT/CT显像分级结果进行ROC分析,得到全身骨显像曲线下面积为0.860±0.056,SPECT/CT显像曲线下面积为0.974±0.020。SPECT/CT曲线下面积大于全身骨显像曲线下面积,两者之间差异具有统计学意义(χ2=9.924,P<0.001)。本研究结果表明,SPECT/CT融合显像较全身骨显像具有更好的诊断效能。
-
乳腺癌发生骨转移的概率很高,是主要的死亡原因。约90%骨转移灶发生于红骨髓内,如椎体及骨盆,其次发生于肋骨、颅骨及四肢骨近端。骨转移引起的骨痛、病理性骨折、高钙血症等并发症常严重影响患者的生活质量。及早发现、及早治疗转移灶对患者的生活质量与生存状况具有重要的价值。99Tcm-MDP全身骨显像是检查肿瘤骨转移最常用的功能影像学方法,灵敏度高,可较常规X线检查方法早3~6个月发现异常病灶。当放射性浓聚灶位于结构复杂的中轴骨如头颅骨、椎体附件或骨盆骨不能判断位置或者出现局部单发病灶时,单一的全身骨显像容易引起误诊,此时应用SPECT显像能够提高病灶定位的准确率[6-7];由于核素显像是功能成像,解剖结构层次不清晰,此时联合其他检查方法如CT、MRI检查就很必要。这样可进一步提高诊断的特异性。
核素全身骨显像是利用骨骼内羟基磷灰石结晶吸附亲骨性的99Tcm-MDP而成像,只要局部骨骼的代谢活性、血流量或交感神经兴奋性发生改变时都会出现异常显像,恶性骨转移瘤、恶性及良性肿瘤、骨损伤、代谢性骨病及骨骼退行性病变等均可导致局部放射性示踪剂吸附的增加或减少,因此,全身骨显像的灵敏度高而特异度低。Sharma等[8]研究显示,乳腺癌骨转移患者行SPECT/CT显像的灵敏度、特异度及准确率分别为83%、98%和90%。本研究结果显示,单一全身骨显像时,有78.38%(29/37)的病灶可初步确定性质;在进一步行SPECT/CT显像后,灵敏度、特异度及准确率分别为93.10%、87.50%和91.89%,与Sharma等[8]的研究结果相近。本研究中,乳腺癌骨转移病灶显示椎骨及肋骨是较多出现转移灶的部位(20/37, 54.05%;4/37, 10.81%)。由于椎骨形态不规则、结构复杂、关节面多,并且许多乳腺癌患者处于绝经期或围绝经期或接受化学治疗后,椎骨及肋骨发生程度不等的退行改变,易导致骨折等发生,全身骨显像解剖结构层次不清晰,进一步增加了诊断及病灶性质判断的难度。此时,进行SPECT及CT就显得很有必要。本研究中有2个椎骨病灶在初诊时判读为良性,复查时才最终确定为恶性病灶,是由于初诊时椎骨CT扫描形态结构无异常且位于椎骨附件局部,增加了病灶性质鉴别的难度。本研究样本量较小,且大部分骨骼放射性异常浓聚灶的病理检查实际上不具有可操作性,病灶恶性性质的确诊有待更理想方法的建立,以便进一步完善本研究。本研究中,由于病例数较少,有待于进一步收集相关病例资料。
综上所述,全身骨显像的高灵敏度已被公认,而CT又能够提供细致的解剖影像,所以利用全身骨显像发现骨骼可疑病灶,对不能确定性质的病灶进行有针对性的SPECT/CT显像,能够提高诊断准确率,具有重要的临床价值,有助于指导乳腺癌患者的综合治疗。
乳腺癌患者骨病灶SPECT/CT融合显像的临床价值
The clinical value of SPECT/CT fusion imaging in the diagnosis of bone metastasis of breast cancer
-
摘要:
目的 探讨SPECT/CT融合显像诊断与鉴别乳腺癌患者全身骨显像放射性异常浓聚灶的临床价值。 方法 对25例乳腺癌患者的99Tcm-MDP全身骨显像显示的骨异常放射性浓聚灶行SPECT/CT融合显像。4~8个月后再次行全身骨显像及SPECT/CT融合显像复查。图像由两名有经验的核医学科医师独立分析, 部分CT图像由有经验的放射科医师分析指导。 结果 在25例乳腺癌患者的37个异常放射性浓聚灶中, 确定29(29/37, 78. 38%)个病灶为骨转移灶, 其中有2个椎体病灶在初次检查中判读为良性病灶; 8(8/37, 21. 62%)个病灶为良性病灶, 其中1个肋骨病灶在初次检查中判读为骨转移灶, 比较全身骨显像和SPECT/CT融合显像, 二者之间差异有统计学意义(χ2=6.975, P < 0.05)。骨转移灶主要分布于椎骨及肋骨。全身骨显像和SPECT/CT融合显像的诊断灵敏度、特异度、阳性预测值、阴性预测值和准确率分别为82.76%、75.00%、92.31%、54.55%、81.08%和93.10%、87.50%、96.43%、77.78%、91.89%。采用受试者操作特性曲线(ROC)进行分析, 结果:全身骨显像曲线下面积为0. 860±0. 056, SPECT/CT融合显像曲线下面积为0. 974±0. 020。SPECT/CT融合显像曲线下面积大于全身骨显像曲线下面积, 两者之间差异具有统计学意义(χ2=9. 924, P < 0.001)。 结论 SPECT/CT融合显像较全身骨显像能更好地鉴别出乳腺癌骨病灶的性质, 能够提高诊断准确率, 具有重要的临床价值; 必要时应在4~8个月后复查SPECT/CT。 -
关键词:
- 乳腺肿瘤 /
- 肿瘤转移 /
- 体层摄影术,发射型计算机,单光子 /
- 体层摄影术,X线计算机
Abstract:Objective To evaluate the clinical value of SPECT/CT fusion imaging in the diagnosis and differential diagnosis the characteristic of the whole body bone scan radioactive hot lesions in patients with breast cancer. Methods The abnormal radioactive hot lesions of whole body bone scan in 25 patients with breast cancer underwent SPECT/CT fusion imaging immediately. Another whole body bone scan and SPECT/CT fusion imaging were carried out 4 to 8 months later in all these patients. The whole body bone scan images, SPECT/CT images and fusion images were analyzed independently by two experienced nuclear medicine physicians and some of the equivocal CT images were analyzed by an experienced radiologist. Results Among all the 37 abnormal radioactive hot bone lesions, 29(29/37, 78. 38%) lesions were confirmed metastatic lesions, including 2 vertebral lesions classified as benign lesions on the basis of the first examinations data; and 8 lesions were benign, including a rib lesion classified as benign lesion according to the first examinations data. The difference between whole body bone scan and SPECT/CT examination was statistically significant(χ2=6. 975, P < 0. 05). The bone metastases are located mainly in spine and ribs. The sensitivity, specificity, positive and negative predictive values, and accuracy of whole-body bone scan and SPECT/CT fusion imaging were 82.76%, 75.00%, 92.31%, 54.55%, 81.08% and 93.10%, 87.50%, 96.43%, 77.78%, 91.89%, respectively. The area under the receiver operating characteristics curve was 0. 860±0. 056 for whole body bone scan and 0. 974±0. 020 for SPECT/CT. The area under the curve for SPECT/CT was significantly larger compared with the whole body bone scan(χ2=9. 924, P < 0. 001). Conclusions SPECT/CT fusion imaging is better than whole body bone scan alone to characterize the abnormal bone radioactive hot lesions and it can improve the accuracy of diagnosis. The patients should repeat the modality 4 to 8 months later if necessary. -
[1] Jemal A, Siegel R, Ward E, et al. Cancer statistics, 2007. CA Cancer J Clin, 2007, 57(1): 43-66. doi: 10.3322/canjclin.57.1.43 [2] 周涛, 陈丽芬. 30岁以下乳腺癌临床病理特征及分子生物学特点分析.国际肿瘤学杂志, 2006, 33(11): 874-877. doi: 10.3760/cma.j.issn.1673-422X.2006.11.024
[3] 汤志谋, 许海富, 李明智. SPECT核素骨显像联合MRI增强成像鉴别诊断骨转移瘤100例临床观察.实用癌症杂志, 2009, 24(5): 498-500. doi: 10.3969/j.issn.1001-5930.2009.05.019
[4] 韩鹏慧, 张书旭, 葛永兵, 等. SPECT/螺旋CT融合显像鉴别诊断颅骨良恶性病变的临床价值.中国临床医学影像杂志, 2012, 23(7): 484-487. doi: 10.3969/j.issn.1008-1062.2012.07.008
[5] 李少林, 王荣福.核医学. 7版.北京:人民卫生出版社, 2008: 153.
[6] Even-Sapir E. Imaging of malignant bone involvement by morphologic, scintigraphic and hybrid modalities. J Nucl Med, 2005, 46(8): 1356-1367. [7] Horger M, Bares R. The role of single photon emission computed tomography/computed tomography in benign and malignant bone disease. Semin Nucl Med, 2006, 36(4): 286-294. [8] Sharma P, Singh H, Kumar R, et al. Bone scintigraphy in breast cancer: added value of hybrid SPECT-CT and its impact on patient management. Nucl Med Commun, 2012, 33(2): 139-147. -





 下载:
下载: