-
分化型甲状腺癌(differentiated thyroid carcinoma,DTC)是最常见的甲状腺恶性肿瘤,其中大部分是甲状腺乳头状癌(papillary thyroid cancer,PTC),约占85%[1]。甲状腺球蛋白(thyroglobulin,Tg)水平在PTC术后131I治疗随访中有重要的价值,是判断甲状腺癌复发或转移的重要指标之一[2-3],近年来备受关注。但对Tg与PTC颈部淋巴结转移的关系却少有报道,本研究分析了45例PTC患者术后刺激状态Tg水平与颈部淋巴结转移的关系,现报道如下。
-
1998年1月至2011年10月在本院经手术和病理检查确诊为PTC的患者45例,其中,男性16例、女性29例,年龄6~70岁,所有患者均行甲状腺全切(40例)或近全切(5例),同时行颈部淋巴结清扫术。根据颈部淋巴结的转移情况将所有患者分为2组:非转移组(L0 组)[共14例(男性4例、女性10例),平均年龄(42.4±11.4)岁]和转移组(L1组)[共31例(男性12例、女性19例),平均年龄(43.9±16.3)岁]。甲状腺癌有远处转移者不纳入本研究。
-
采用瑞士Roche公司生产的Cobas e 601电化学发光免疫分析仪,在术前常规条件下检测患者血清中游离三碘甲状腺原氨酸、游离甲状腺素、促甲状腺激素(thyroid stimulating hormone,TSH)、Tg、甲状腺球蛋白抗体(thyroglobulin antibody,TgAb)水平。术后禁碘饮食,未补充甲状腺激素,3~4周后检测血清中游离三碘甲状腺原氨酸、游离甲状腺素、TSH、Tg和TgAb水平,以术后血清TSH > 30 mU/L时的Tg作为术后刺激状态Tg水平(血清Tg正常值≤84 μg/L),为避免血清中TgAb对Tg水平的影响,本研究在病例选择时剔除了TgAb阳性的患者。
-
一般资料分析采用t检验和卡方检验;数据采用均数±标准差(x±s)表示,采用SPSS 13.0统计学软件进行t检验;采用Pearson相关性分析评价术后刺激状态Tg水平与淋巴结转移数目的相关性,P < 0.05为差异有统计学意义。
-
L1组和L0组患者的年龄(t=-0.675,P > 0.05)和性别(χ2=1.20,P > 0.05)的差异无统计学意义。L1组术后刺激状态Tg水平为(380.85±337.10)μg/L,L0组术后刺激状态Tg水平为(32.04±26.85)μg/L,2组术后刺激状态Tg水平差异有统计学意义(t=4.617,P < 0.01)。
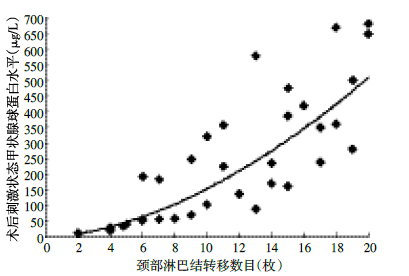
本研究45例患者中,31例(69%)伴颈部淋巴结转移,共清扫淋巴结833枚,其中经病理学检查诊断转移淋巴结350枚(42%),颈部转移淋巴结数目与术后刺激状态Tg水平呈正相关(r=0.676,P < 0.01)(图 1)。
-
Tg是一种糖蛋白,储存于甲状腺滤泡,由甲状腺滤胞细胞和分化较好的甲状腺癌细胞分泌。PTC患者的甲状腺滤泡细胞有活跃的Tg分泌[4],术前血清中Tg水平阳性率不高,不宜将术前Tg水平作为甲状腺癌的筛查指标。本研究中45例PTC患者术前仅有4例Tg水平高于正常,阳性率仅为8.9%。而术后刺激状态Tg水平比抑制状态具有更高的灵敏度和准确率,在PTC的术后随访中有重要的价值,而术后刺激状态Tg水平与131I清除残留甲状腺组织治疗后刺激状态Tg水平呈明显正相关[5],可作为判断有无甲状腺癌转移或复发的重要指标之一[2-3]。李田军等[6]报道PTC患者术后刺激状态Tg水平对预测远处转移有较高的准确率。本研究结果显示,PTC颈部淋巴结转移患者术后刺激状态Tg水平较无颈部淋巴结转移患者明显增高,提示术后刺激状态Tg水平与颈部淋巴结的转移情况均是预测PTC患者预后的重要指标。
影响PTC术后Tg水平的因素较多,如肿瘤的TNM分期(T代表原发肿瘤,N代表区域淋巴结,M代表远处转移)等,有文献报道,肿瘤大小、病灶数量、血管和周围软组织侵犯等均是影响Tg水平和患者预后的常见原因[7-8],并且颈部淋巴结的转移情况可独立影响131I清除残留甲状腺组织后刺激状态的Tg水平[9-10]。本研究中有31例(69%)患者经病理证实伴有颈部淋巴结转移,转移的淋巴结多分布在Ⅵ区(60%),且患者颈部淋巴结转移数目与术后刺激状态Tg水平呈明显正相关。因此笔者认为,甲状腺癌患者常发生颈部淋巴结转移,在行甲状腺切除的同时,应常规进行颈部淋巴结清扫(尤其是Ⅵ区),可有效降低肿瘤复发及转移,同时术后刺激状态Tg水平的变化是评价PTC术后131I治疗疗效的重要指标。
甲状腺乳头状癌术后刺激状态Tg与颈部淋巴结转移关系的研究
The correlation between the stimulated thyroglobulin level after surgery in papillary thyroid carci-noma and cervical lymph node metastasis
-
摘要:
目的 探讨甲状腺乳头状癌(PTC)患者术后刺激状态甲状腺球蛋白(Tg)与颈部淋巴结转移的关系。 方法 45例PTC患者行甲状腺全切或近全切并行颈部淋巴结清扫术,根据是否存在淋巴结转移分为L1和L0 2组,检测术后刺激状态Tg水平,采用统计学软件对数据进行t检验及相关性分析。 结果 2组患者的年龄(t=-0.675,P > 0.05)、性别(χ2=1.20,P > 0.05)差异无统计学意义,术后刺激状态Tg水平差异有统计学意义(t=4.167,P < 0.01)。L1组术后刺激状态Tg水平与颈部淋巴结转移水平呈正相关(r=0.676,P < 0.01)。 结论 PTC患者术后刺激状态Tg水平与颈部淋巴结转移关系密切,是评价PTC术后131I治疗疗效及判断预后的重要指标。 Abstract:Objective To discuss the correlation between the stimulated thyroglobulin (Tg) level after surgery in papillary thyroid carcinoma (PTC) and cervical lymph node metastasis. Methods Total thyroidectomy or subtotal thyroidectomy and radical cervical lymphadenectomy have been performed in 45 cases with PTC. All patients have been divided into two groups (L1 group and L0 group) according to whether lymph node metastasis exists. The stimulated Tg level after surgery were mesured and analyzed by t test with statistical software. Results There was no significant difference between the two groups in age (t=-0.675, P > 0.05) and gender(χ2=1.20, P > 0.05), but significant difference could be found in stimulated Tg level after surgery between the two groups(t=4.167, P < 0.01). There was positive correlation between the stimulatied Tg level after surgery and cervical lymph node metastasis in L1 group(r=0.676, P < 0.01). Conclusion The stimulated Tg level after surgery is closely correlated to cervical lymph node metastasis in patients with PTC, which can be used as an assessment of the effect of the postsurgical 131I therapy and prognosis. -
Key words:
- Thyroid neoplasms /
- Carcinoma /
- papillary /
- Thyroglobulin /
- Lymph nodes
-
[1] American Thyroid Association(ATA)Guidelines Taskfouce on Thyroid Nodules and Differentiated Thyroid Cancer, Cooper DS, Doherty GM, et al. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid, 2009, 19(11): 1167-1214. doi: 10.1089/thy.2009.0110 [2] Kim TY, Kim WB, Kim ES, et al. Serum thyroglobbulin levels at the time of 131I remnant ablation just after thyroidectomy are useful for early prediction of clinical recurrence in low-risk patients with differentiated thyroid carcinoma. J Clin Endocrinol Metab, 2005, 90(3): 1440-1445. doi: 10.1210/jc.2004-1771 [3] Heemstra KA, Liu YY, Stokkel M, et al. Serum thyroglobulin concentrations perdict disease-free remission and death in differentiated thyroid carcinoma. Clin Endocrinol(Oxf), 2007, 66(1): 58-64. [4] Suh I, Vrients MR, Guerrero MA, et al. Serum thyroglobulin is a poor diagnostic biomarker of malignancy in follicular and Hurthle-cell neoplasms of the thyroid. Am J Surg, 2010, 200(1): 41-46. doi: 10.1016/j.amjsurg.2009.08.030 [5] 高再荣, 常伟, 崔坤炜, 等.甲状腺乳头状癌术后刺激状态Tg预测131I清甲治疗后Tg水平的价值.中华核医学杂志, 2009, 29(3): 156-159. doi: 10.3760/cma.j.issn.0253-9780.2009.03.005
[6] 李田军, 林岩松, 梁军, 等. 131I治疗前刺激性Tg对乳头状甲状腺癌远处转移的预测价值.中华核医学与分子影像杂志, 2012, 32(3): 189-191. doi: 10.3760/cma.j.issn.2095-2848.2012.03.007
[7] Lundgren CI, Hall P, Dickman PW, et al. Clinically significant prognostic factors for differentiated thyoid carcinoma: a population-based, nested case-control study. Cancer, 2006, 106(3): 524-531. [8] Bilimoria KY, Bentrem DJ, Ko CY, et al. Extent of surgery affects survival for papillary thyroid cancer. Ann Surg, 2007, 246(3): 375-384. doi: 10.1097/SLA.0b013e31814697d9 [9] Sawka AM, Orlov S, Gelberg J, et al. Prognostic value of postsurgical stimulated thyroglobulin levels after initial radioactive iodine therapy in well-differentiated thyroid carcinoma. Head Neck, 2008, 30(6): 693-700. doi: 10.1002/hed.20755 [10] Low TH, Delbridge L, Sidhu S, et al. Lymph node status influences follow-up thyroglobulin levels in papillary thyroid cancer. Ann Surg Oncol, 2008, 15(10): 2827-2832. doi: 10.1245/s10434-008-0049-1 -






 下载:
下载: