-
在我国,前列腺癌的发病率逐年上升。目前,对于前列腺癌治疗的疗效评价和肿瘤复发的早期诊断主要依靠检测前列腺特异性抗原(prostate-specific antigen,PSA)水平,且对于前列腺癌复发的患者,其肿瘤是局部复发还是已经发生远处转移,仍缺乏合适的常规影像学检查方法。18F-FDG PET-CT能同时提供肿瘤细胞的增殖代谢信息和肿瘤病灶的解剖结构信息,可一次成像探测全身转移灶。为此,本研究探讨了18F-FDG PET-CT对前列腺癌复发、转移的诊断价值。
-
2009年11月至2011年2月,临床诊断为可疑前列腺癌复发或转移、来我科行18F-FDG PET-CT的患者23例,年龄55~86岁, 平均69.2岁。治疗方法包括:前列腺根治性切除5例、经尿道前列腺电切术2例、调强适形放疗4例、内分泌治疗12例。查阅全部病历及资料进行回顾性分析,23例中,高分化腺癌3例、中分化腺癌10例、低分化腺癌10例。临床可疑复发、转移的表现:血清PSA水平升高,排尿困难及尿频、尿急等膀胱刺激症状,肉眼见血尿,骨痛等。
-
采用德国siemens公司Biography Truepoint(52环/64层)PET-CT仪。18F-FDG由江苏南京军区总医院加速器中心提供,放化纯度 > 95%。
-
患者检查前禁食6 h以上,并常规测定血糖水平,控制血糖 < 7.8 mmol/L。经肘静脉按体重注射3.70~5.55MBq/kg(0.1~0.15mCi/kg)18F-FDG,嘱患者多饮水并静脉推注速尿剂以减少膀胱的放射性,50 min时排尿后行全身PET-CT,扫描范围从颅顶至股骨上段。CT扫描参数:电压120 kV,电流80 mA,层厚5 mm。PET采集方式:三维,扫描床位数5个,1.2 min/床位。
-
用高清PET技术对PET图像进行重建,并用TrueC散射校正(高精度校正软件)对PET图像进行散射校正和衰减校正。CT图像重建采用标准重建法,重建层厚5 mm,PET重建层厚5 mm,将校正后的PET图像和CT图像进行融合,分别得到横断、矢状、冠状位CT、PET及PET-CT融合图像。延迟1h排空尿液后再次对盆腔进行扫描,获取延迟图像。
-
由2位经验丰富的核医学科医师对所有PET、CT和PET-CT融合图像进行逐帧对比分析;PET-CT采用半定量分析(SUV测定)和目测相结合的方法,根据病灶放射性浓聚程度、形态、位置、密度等综合诊断,以SUV > 2.5作为阳性判断标准。
-
应用罗氏公司e601电化学发光仪,对受检者PSA值进行电化学发光免疫分析,试剂盒为江苏南京欧诺医疗设备有限公司提供,正常参考值为0~4mg/L。
-
23例患者中,PET-CT阳性20例,其中:前列腺局部结节状放射性浓聚(SUV为2.7~10.8)5例;盆腔淋巴结转移8例;全身多发淋巴结转移1例,其中最大转移淋巴结为2.9 cm×2.8 cm,最小淋巴结短径5 mm;盆腔脓肿1例;全身骨转移5例,发现骨转移病灶27处。3例患者的PET-CT在全身未见恶性征象。小淋巴结与骨转移的明确定位均依靠PET-CT融合图像获得。血清PSA水平与PET-CT的关系见表 1。
组别 例数 血清PSA值(mg/L) < 10 10~20 20~100 > 100 PET-CT阳性 20 1 3 10 6 PET-CT阴性 3 2 1 0 0 表 1 前列腺癌患者治疗后复发、转移的PET-CT诊断与PSA水平的关系(例数)
-
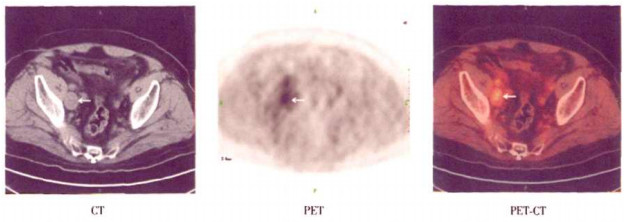
PET-CT诊断为阳性患者的20例中,12例患者经活组织或切除后病理检查,证实盆腔淋巴结转移8例,其中1例为调强适形放疗后出现小便次数增多、血尿、腰骶部疼痛,PSA为49 mg/L,PET-CT图像示右侧髂血管旁多发肿大淋巴结18F-FDG代谢增高,临近膀胱壁增厚,考虑为前列腺癌膀胱壁受侵犯及盆腔淋巴结转移(图 1);盆腔脓肿1例;前列腺癌局部复发3例,均为内分泌治疗后PSA稳定(6~100 mg/L)的患者。7例患者经临床随访证实复发、转移,均为内分泌治疗后PSA水平持续上升者,其中2例CT、B超示盆腔淋巴结肿大,5例骨扫描证实全身多发骨转移,随访结果示复发性前列腺癌治疗后未控。
图 1 前列腺癌患者,86岁,调强适形放疗后,小便次数增多、血尿、PSA水平升高。PET-CT图像示右侧髂血管旁多发肿大淋巴结18F-FDG代谢增高,临近膀胱壁增厚,考虑为前列腺癌膀胱壁受侵犯及盆腔多发淋巴结转移。
PET-CT未见恶性征象的3例患者中,1例B超提示前列腺体积增大,腺体不对称,右侧叶低回声,穿刺活检未见异常;2例前列腺癌根治术后随访1年未见异常。
-
8例PET-CT诊断为盆腔淋巴结转移者,B超、CT仅发现2例;1例PET-CT诊断全身多发淋巴结转移者,B超和腹部CT均未见异常;全身骨显像提示骨转移5例,与PET-CT结果一致,但全身骨显像发现骨转移灶仅24处。
-
前列腺癌治疗后肿瘤是否复发,主要依靠血清PSA水平的检测,目前的影像学检查如经直肠前列腺B超、骨显像、CT和MRI等检查并不能满足前列腺癌是否复发或远处转移的需要[1]。PET-CT将PET所获得的器官、组织及病变的功能分子信息与螺旋CT所获得的精确解剖结构信息融为一体,对病灶的探测、定性及定位具有重要价值,且PET-CT一次成像可进行全身检查,为前列腺癌复发、转移的诊断提供了新的监测手段[2]。
本研究显示,18F-FDG PET-CT诊断前列腺癌复发、转移的灵敏度、特异度及准确率分别为100%、75%及95%,与国外报道相似[3]。18F-FDG PET-CT可以鉴别前列腺癌是否局部复发,而且随着PSA水平的升高,其呈现为阳性图像的可能性越大。有报道提示,前列腺癌根治术后血清PSA水平将增加0.2~0.4 mg/L,而外放射治疗后其血清PSA水平会连续升高[4]。本研究使用18F-FDG PET-CT检测到2例前列腺癌患者经根治术后,因盆腔淋巴结转移而导致PSA水平升高。Chang等[3]对24例局限性前列腺癌治疗后血清PSA水平升高的患者行18F-FDG PET-CT,并与盆腔淋巴结切除术后的病理结果对比,认为18F-FDG PET-CT对治疗后PSA水平升高者盆腔淋巴结转移的诊断价值较高。本研究用18F-FDG PET-CT发现8例盆腔淋巴结转移和1例全身多发淋巴结转移患者。
与其他影像学检查比较,本研究显示,PET-CT较CT、B超可发现更多的病灶。其原因可能为:①常规CT、MRI将短径 > 10 mm视为转移淋巴结,但对肿大淋巴结不能定性,由于转移淋巴结与原发灶具有相似的代谢特点,因此用18F-FDG PET-CT既提高了对 < 10 mm转移淋巴结的检出率,也能对CT、B超发现的肿大淋巴结进行定性;②常规影像学检查无法鉴别治疗后改变与复发;③病灶可能为多部位转移,位于常规局部影像检查的扫描范围之外[5]。
Jadvar等[6]对种植了激素依赖性和激素非依赖性前列腺癌的大鼠进行超微PET研究,发现激素依赖性前列腺癌的18F-FDG浓聚程度要低于激素非依赖性前列腺癌。因此,18F-FDG PET-CT可用于评价前列腺癌去雄激素治疗的反应和早期发现转移性前列腺癌激素治疗后的复发。本研究中的12例前列腺癌患者经内分泌治疗后,3例PSA水平稳定,9例PSA水平逐渐升高,经PET-CT检查则发现异常。
18F-FDG PET-CT对骨转移者较敏感,尤其对血清PSA > 20 mg/L、并高度怀疑骨转移的患者,其前列腺癌组织学分级越高、分期越晚的病灶,18F-FDG浓聚程度越高。Nakamoto等[7]报道,对403例恶性肿瘤患者骨转移的18F-FDG PET-CT结果显示,18F-FDG PET-CT可比骨显像发现更多的病灶,而本研究显示两者相似,这可能与病例数较少有关。
综上所述,18F-FDG PET-CT有助于前列腺癌复发、转移的诊断,是一种无创性检查方法;另可评价前列腺癌经内分泌治疗后的反应和早期发现激素治疗后的复发。由于本研究的病例数有限,需扩大样本量作进一步研究。
18F-FDG PET-CT诊断前列腺癌复发与转移的价值
Value of 18F-FDG PET-CT in diagnoss of prostate cancer recurrence and metastasis
-
摘要:
目的 探讨18F-FDG PET-CT在前列腺癌复发、转移诊断中的价值。 方法 回顾性分析23例前列腺癌治疗后随访期间临床怀疑复发、转移患者的18F-FDG显像资料,同期常规显像检查结果,病理及临床随访结果。 结果 经病理及临床随访结果证实前列腺癌复发、转移者19例。PET-CT诊断为阳性者20例,其中1例盆腔脓肿、5例前列腺癌局部复发、8例盆腔淋巴结转移、1例全身多发淋巴结转移和5例骨转移;18F-FDG PET-CT诊断前列腺癌复发与转移的灵敏度为100%(19/19),特异度为75%(3/4),准确率为95%(22/23)。内分泌治疗后前列腺特异性抗原水平较稳定及逐渐升高者共12例,PET-CT均准确显示。与B超、CT、骨显像相比,PET-CT可发现更多的病灶。 结论 18F-FDG PET-CT对前列腺癌复发、转移的诊断有重要价值。 -
关键词:
- 前列腺肿瘤 /
- 正电子发射断层显像术 /
- 体层摄影术,X线计算机 /
- 氟脱氧葡萄糖F18 /
- 前列腺特异性抗原
Abstract:Objective To investigate the value of 18F-FDG PET-CT on patients with suspected prostate cancer recurrence and metastasis. Methods Retrospective analysis 23 patients with prostate cancer who were suspected to have tumor recurrence and metastasis during follow-up, underwent 18F-FDG PET-CT examination. 18F-FDG PET-CT results were compared with those of conventional images, as referred to histopathology or clinical follow-up. Results In total, 19 patients with recurrence and metastasis were confirmed by histopathology or clinical follow-up. Twenty patients were found to have positive lesion by 18F-FDG PET-CT, including the pelic abscess (1case), prostate cancer local recurrence(5cases), lymph node metastases(8cases), multiple systemic lymph node metastasis(1case)and bone metastases(5cases). The sensitivity of 18F-FDG PET-CT was 100%(19/19)in diagnosis carcinoma recurrence and metastasis, and the specificity and accuracy were 75%(3/4)and 95%(22/23). The levels of prostate specific antigen in 12 patients gradually increased after endocrine theraphy, and PET-CT could dipit this accurately. Compared with conventional images such as B mode ultrasonic, CT, bone imaging, 18F-FDG PET-CT could find more focus. Conclusion 18F-FDG PET-CT imaging is valuable in diagnosing recurrent and metastatic prostate cancer. -
表 1 前列腺癌患者治疗后复发、转移的PET-CT诊断与PSA水平的关系(例数)
组别 例数 血清PSA值(mg/L) < 10 10~20 20~100 > 100 PET-CT阳性 20 1 3 10 6 PET-CT阴性 3 2 1 0 0 -
[1] Hricak H, Schoder H, Pucar D, et al. Advances in imaging in the postoperative patient with a vising prostate-specific antigen level. Semin Oncol, 2003, 30(5): 616-634. doi: 10.1016/S0093-7754(03)00359-2 [2] Scher B, Seitz M. PET/CT imaging of recurrent prostate cancer. Eur J Nucl Med Mol Imaging, 2008, 35(1): 5-8. doi: 10.1007/s00259-007-0633-9 [3] Chang CH, Wu HC, Tsai JJ, et al. Detecting metastatic pelvic lymph nodes by 18F-2-deoxyglucose positron emission tomography in patients with prostate-specific antigen relapse after treatment for localized prostate cancer. Urol Int, 2003, 70(4): 311-315. doi: 10.1159/000070141 [4] Jorge RZ, Macarena R, Anibal RM, et al. Usefulness of PET scans in diagnosing recurrent prostate cancer. Prostate with PSA level < 5ng/ml. Actas Urol Esp, 2009, 33(8): 844-852. doi: 10.1016/S0210-4806(09)72870-0 [5] Jerusalem G, Hustinx R, Beguin Y, et al. PET scan imaging in oncology. Eur J Cancer, 2003, 39(11): 1525-1534. doi: 10.1016/S0959-8049(03)00374-5 [6] Jadvar H, Xiankui L, Shahinian A, et al. Glucose metabolism of human prostate cancer mouse xenografts. Mol Imaging, 2005, 4(2): 91-97. [7] Nakamoto Y, Osman M, Wahl RL. Prevalence and pattems of bone metastases detected with positron emission tomography using F-18 FDG. Clin Nucl Med, 2003, 28(4): 302-307. -





 下载:
下载: