-
鼻咽癌是我国常见恶性肿瘤之一, 在我国头颈部肿瘤中的发病率居首位。由于鼻咽癌特殊的生物学行为以及解剖学部位, 放射治疗是其首选并且是最主要的治疗手段。但由于个体间肿瘤敏感性的不同, 相同放疗剂量能够达到的治疗效果存在着很大的差异。目前多个研究显示, 对于根治性放疗结束后仍有肿瘤残留而采用局部加量治疗, 或局部复发后采用再次放疗治疗, 都可能产生严重的放疗后期反应, 影响患者的生活质量[1-2]。因此, 早期评估放疗疗效, 确定是否需要加量或采用更有效的治疗方式, 制定个体化的治疗方案, 对提高患者的无瘤生存率以及生活质量都有重要的影响。
在评价其他肿瘤治疗效果的研究中显示, 18FFDG PET-CT所反映的细胞代谢水平变化明显先于CT、MRI所反映的形态组织学变化。部分研究还证实, 鼻咽癌组织中细胞增殖核蛋白Ki67表达水平不但与肿瘤的淋巴结转移、远处转移以及临床分期等有联系, 还与鼻咽癌的放疗敏感性密切相关[3-4]。本研究拟通过对18F-FDG PET-CT在裸鼠鼻咽癌移植瘤放疗监测中的应用以及Ki67表达水平的检测, 探讨18F-FDG PET-CT对早期评估裸鼠鼻咽癌移植瘤放疗疗效的作用, 并分析18F-FDG PET-CT与Ki67表达之间的关系。
-
BALB/C系雄性裸小鼠15只, 鼠龄4~6周, 质量16.3~19.8 g, 由中山大学实验动物中心提供, 在无特定病原体环境下饲养。
-
人鼻咽癌低分化鳞癌细胞株CNE-2, 由中山大学实验动物中心提供。小牛血清购于杭州四季青生物公司; RPMI-1640培养液、胰蛋白酶均为美国Sigma公司产品。
-
CNE-2细胞用含有100 U/ml青霉素和链霉素及15%小牛血清的RPMI-1640培养液培养, 置于37℃、含5%CO2的培养箱中, 传代一周, 待细胞长成满瓶时, 用0.25%胰蛋白酶和0.02%乙二胺四乙酸, 按1∶1混合配成的消化液, 制成1.0×106/ml的细胞悬液, 用7号针头注入0.2 ml于裸鼠右腋皮下。待瘤体最大直径达到1.0~1.5 cm时, 将裸鼠随机分成3个组。
-
将15只裸鼠随机分成3个小组: 对照组、6 Gy放疗组、12 Gy放疗组。①对照组直接行18FFDG PET-CT; 6 Gy放疗组给予单次6 Gy放疗, 于放疗前后分别行18F-FDG PET-CT; 12 Gy放疗组给予2次6 Gy放疗, 于放疗前、第1次放疗后、第2次放疗后第2 d、第6 d分别行18F-FDG PETCT。②所有裸鼠于实验结束后处死并行病理检查。
-
采用F34-1型深部X射线治疗机(北京东方红医疗器械厂), 照射条件: 电压120 kV, 电流12 mA, 焦皮距40 cm, 滤过板0.25 mm Cu, 空气量600 cGy/次。照射时将裸鼠固定在特制的有机玻璃固定架上, 暴露肿瘤, 非照射部位用铅板遮蔽。
-
采用Philips公司GEMINI型PET-CT, CT为MX8000两排螺旋CT。18F-FDG由广州同位素中心提供。
-
显像前夜所有实验裸鼠予禁食, 可自由饮水。经尾静脉注射7.4 MBq18F-FDG后1 h显像。CT扫描参数为120 kV、120 mAs, 层厚5 mm, 螺距1.0, PET以三维采集方式采集, 3 min/床位, 采集后进行PET图像重建和图像融合处理, 用CT数据进行非均匀透射衰减校正PET重建, 采用Ramla三维重建分别获得横断面、冠状面和矢状面图像。
-
依据计算机自动生成的PET-CT融合图像, 采用感兴趣区技术测定T/NT值, 进行定量分析。
-
所有病理学标本行常规10%福尔马林固定, 石蜡包埋切片, 苏木精-伊红染色, 20倍光镜观察。免疫组织化学染色使用Envision法对切片进行Ki-67染色, 鼠抗人单克隆抗体工作液Ki-67检测试剂盒购自上海基因科技有限公司。
Ki-67以胞核呈棕黄色染色为阳性判断标准。高倍镜(×400)下选择10个有代表性的视野, 每个视野计数100个肿瘤细胞, 计算阳性细胞的百分比。
-
样本均数以x±s表示, 采用SPSS13.0统计软件进行t检验, 多组间比较采用LSD法, 同一实验组裸鼠移植瘤不同时间T/NT值两两比较采用配对t检验, 不同实验组之间Ki67表达两两比较采用独立t检验, 以P<0.05作为具有统计学差异的标准。
-
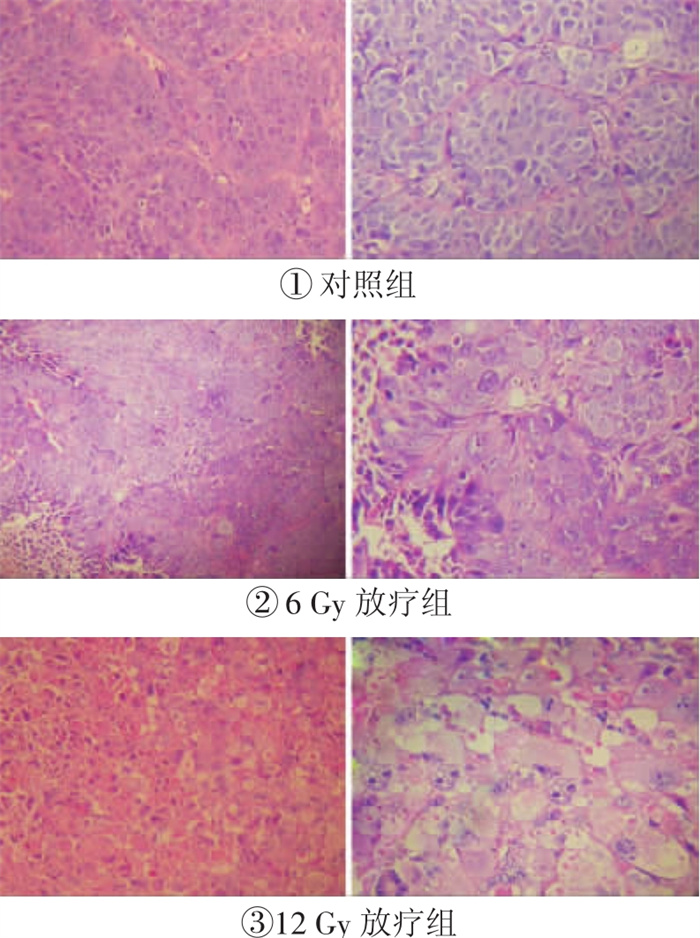
对照组裸鼠移植瘤内肿瘤细胞死亡率均小于25%;6 Gy放疗组裸鼠移植瘤内可见约半数肿瘤细胞变性坏死, 死亡率在26%~75%之间; 12 Gy放疗组移植瘤内可见大量肿瘤细胞空泡变性、坏死, 肿瘤周围可见出血及炎性细胞浸润, 其中4只裸鼠肿瘤细胞死亡率在75%以上。(图 1、表 1)
肿瘤细胞死亡率(%) ≤25 25~50 51~75 > 75 对照组 5 0 0 0 6 Gy放疗组 0 3 2 0 12 Gy放疗组 0 1 0 4 表 1 不同实验组裸鼠的肿瘤细胞死亡率情况
-
12 Gy放疗组裸鼠移植瘤在放疗后T/NT值不断降低: 放疗前平均T/NT值为2.17±0.31, 放疗6 Gy后平均T/NT值为1.68±0.42, 放疗12 Gy后2 d平均T/NT值为1.41±0.40, 放疗12 Gy后6 d平均T/NT值为0.70±0.12。放疗前与放疗6 Gy时平均T/NT值没有统计学差异(t=2.108, P > 0.05);放疗12 Gy后2 d与放疗前、放疗6 Gy时比较明显减低(与放疗前比较, t=2.80, P < 0.05;与放疗6 Gy时比较t=3.14, P < 0.05);放疗12 Gy后6 d, 移植瘤平均T/NT值较放疗后2 d进一步减低(与放疗后2 d比较, t=3.49, P < 0.05;与放疗前比较, t=8.01, P < 0.01)。
-
(1) 鼻咽癌移植瘤Ki67的表达随放疗剂量的增加明显降低, 对照组Ki67的平均表达率为(67.28±9.80)%, 6 Gy放疗组Ki67的平均表达率为(31.94±15.92)%, 12 Gy放疗组Ki67的平均表达率为(9.44±15.22)%, 不同组别间Ki67的表达有明显差异(F=21.95, P < 0.01): 12 Gy放疗组显著低于对照组(t=7.145, P < 0.01)及6 Gy放疗组(t=2.384, P < 0.05);6 Gy放疗组Ki67表达水平也低于对照组(t=4.320, P < 0.01)。
(2) 放疗前移植瘤T/NT值与Ki67表达之间无相关性(P=0.391);放疗过程中移植瘤T/NT值与Ki67表达水平的变化呈正相关(r=0.532, P < 0.05)。
-
目前, 鼻咽癌患者放疗后常规采用传统影像CT或MRI对其放疗疗效进行监测, 但这些传统影像学监测主要依赖于病灶的形态学变化, 并且难以区分肿瘤残留与放疗引起的组织水肿、肉芽组织增生等改变。Fang等[5]利用CT对101例单纯根治性放疗的鼻咽癌患者进行放疗前后的病灶体积比较, 发现放疗中肿瘤退缩程度与原发灶的局部控制率以及患者的生存率均无相关性。本研究对比了放疗前后移植瘤的病理变化, 在放疗后6 d肿瘤细胞已经出现大量的空泡变性、坏死, 但在瘤体的形态上却未见明显的缩小, 说明肿瘤的退缩程度并不是早期评估放疗疗效的理想参考指标。
18F-FDG PET-CT除了监测病灶形态的变化, 还可以提供代谢方面的信息。在恶性病变组织中, 由于葡萄糖转运蛋白的过度表达(主要是葡萄糖转运蛋白1和葡萄糖转运蛋白3的表达), 引起葡萄糖摄取的增加, 并且糖酵解活性增高, 因此, 利用18F-FDG PET-CT可以区分病灶与正常组织。Brun等[6]利用18F-FDG PET-CT在放疗初期对头颈部鳞状细胞癌患者放疗疗效进行监测发现, 在给予中位数24 Gy的初始放疗后5~10 d, 放疗敏感患者的肿瘤葡萄糖代谢率已经出现明显减低。本研究在对鼻咽癌移植瘤放疗过程的监测中发现, 移植瘤的T/NT值逐渐减低, 放疗后2 d时移植瘤的T/NT值减低较放疗前已有统计学差异(t=2.80, P < 0.05), 放疗后6 d时T/NT值减低的统计学差异更明显(t=8.01, P < 0.01), 结合病理结果显示的肿瘤细胞大量死亡(其中4只裸鼠移植瘤肿瘤细胞死亡率超过75%), 提示18F-FDG PET-CT对早期评估鼻咽癌的放疗疗效具有重要价值。
由于放疗早期所诱发的炎性改变可以引起照射区域短暂性的18F-FDG摄取增加, 影响18F-FDG PET-CT对肿瘤放疗疗效的准确判断, 因而选择合适的时间点监测放疗疗效非常重要。目前对于评估鼻咽癌放疗效果的最佳时间仍存在着争议, Molthoff等[7]对裸鼠鳞状细胞癌移植瘤的18F-FDG PET研究指出, 放疗后4 d时瘤体的T/NT值出现显著降低并一直保持。而本实验在不同时间点对裸鼠鼻咽癌移植瘤进行监测发现, 放疗后2 d及放疗后6 d时移植瘤的T/NT值均较放疗前明显减低, 但放疗后6 d时减低更加显著, 与放疗后2 d平均T/NT水平也有明显统计学差异(t=3.49, P < 0.05);另外, 放疗后6 d时移植瘤葡萄糖代谢率低于非瘤组织(平均T/NT值为0.70±0.12), 与病理切片所观察到的大量肿瘤细胞死亡的结果相符合, 显示受炎性细胞的影响很小, 并且考虑到放疗后肿瘤细胞凋亡需要渐变的过程, 作为评估鼻咽癌放疗疗效的时间, 放疗后6 d显然较放疗后2 d更加合适, 也更加准确。由于鼻咽癌移植瘤与临床鼻咽癌间在生长环境、肿瘤血供等方面存在差别, 这一时间点能否适用于临床尚待进一步的临床研究证实。
-
Ki67只在增殖细胞中表达, 且生物半衰期短, 是反映细胞增殖活性最敏感的指标之一。Ki67的表达与肿瘤细胞18F-FDG摄取之间是否有联系目前仍存在很大的争议, Cher等[8]和Shimoda等[9]研究发现18F-FDG摄取与恶性肿瘤的增殖活性呈正相关, 但Buck等[10]却认为两者之间没有相关性。本研究通过对比放疗前移植瘤的T/NT值与Ki67的表达情况, 发现两者之间没有相关性, 提示放疗前肿瘤对18F-FDG的摄取与Ki67表达的高低无关。
组织缺氧是影响放疗疗效的一个重要影响因素, 在缺氧环境下, 细胞对放疗的敏感性会降低, 影响放疗的效果。而细胞在缺氧状态下一般处于G0期, Ki67表达水平会减低, 因而Ki67表达与放疗的敏感性密切相关。然而Mary等[11]研究表明, 放疗敏感者与放疗不敏感者在放疗前Ki67的表达并没有统计学差异, 但在给予单次2 Gy的放疗剂量后, 两者之间Ki67表达水平便产生明显分化, 显示与放疗敏感性密切相关的是放疗中Ki67表达的变化, 而不是放疗前Ki67表达的水平。本实验显示Ki67表达随着放疗的进行显著降低, 给予6 Gy放疗时Ki67表达水平已经从(67.28±9.80)%减低至(31.94±15.92)%, 给予12 Gy时更进一步减低至(9.44±15.22)%; 而肿瘤T/NT值也随着放疗的进行显著降低, 与Ki67的表达变化之间存在着正相关(r=0.532, P < 0.05), 提示18F-FDG PET-CT可以反映Ki67表达的变化, 从而间接反映鼻咽癌放疗的敏感性。
综上所述, 18F-FDG PET-CT能够早期反映裸鼠鼻咽癌移植瘤放疗后的变化, 对早期评估鼻咽癌移植瘤的放疗疗效具有重要价值, 第6 d可能是一个合适的时间选择点; 此外, 鼻咽癌的T/NT值的变化与Ki67表达的变化呈正相关, 18F-FDG PET-CT还可以通过间接反映肿瘤细胞Ki67表达水平的变化, 对鼻咽癌的放疗敏感性作出判断, 为临床放疗提供重要的依据。
18F-FDG PET-CT对裸鼠鼻咽癌移植瘤放疗疗效的早期评估及与Ki67表达的相关性研究
18F-FDG PET-CT in early assessing the therapeutic effects of nasopharyngeal carcinoma xenograft in nude mice after radiotherapy and it's relativity to the expression of Ki67
-
摘要:
目的 探讨18F-FDG PET-CT早期评估裸鼠鼻咽癌移植瘤放疗疗效的价值,并初步分析18F-FDG PET-CT与肿瘤细胞增殖因子Ki67表达之间的关系,为临床进一步研究提供依据。 方法 将15只鼻咽癌裸鼠移植瘤动物模型随机分成3组:每组5只,对照组:行18F-FDG PET-CT后并处死;6 Gy放疗组:于放疗前及放疗后1 d分别给予显像后处死;12 Gy放疗组:于放疗前、放疗6 Gy时、放疗12 Gy后第2 d及6 d时分别行18F-FDG PET-CT,并于最后一次显像后处死。所有裸鼠处死后取移植瘤行病理学检查及Ki67染色,分析放疗疗效与Ki67表达的相关性。 结果 ① 12 Gy放疗组放疗前平均T/NT值为2.17±0.31,放疗6 Gy时平均T/NT值为1.68±0.42,放疗12 Gy后2 d时平均T/NT值为1.41±0.40,放疗12 Gy后6 d时平均T/NT值为0.70±0.12,放疗前与放疗6 Gy时没有统计学差异(t=2.108, P > 0.05);放疗12 Gy后2 d与放疗前、放疗6 Gy时比较明显减低,有统计学差异(与放疗前比较,t=2.80,P < 0.05;与放疗6 Gy时比较,t=3.14,P < 0.05);放疗12 Gy后6 d移植瘤的T/NT值较放疗后2 d进一步减低(与放疗后2 d比较,t=3.49,P < 0.05;与放疗前比较,t=8.01,P < 0.01)。②鼻咽癌移植瘤Ki67的表达随放疗剂量的增加明显降低,不同组别间Ki67的表达有明显差别(F=21.95,P < 0.01):12 Gy放疗组Ki67表达显著低于对照组(t=7.145,P < 0.01)及6 Gy放疗组(t=2.384,P < 0.05);6 Gy放疗组Ki67的表达较对照组减低同样存在统计学意义(t=4.320,P < 0.01)。③放疗前移植瘤T/NT值与Ki67表达之间无相关性。④放疗过程中移植瘤T/NT值的变化与Ki67表达水平呈正相关(r=0.532,P < 0.05)。 结论 18F-FDG PET-CT对早期评估裸鼠鼻咽癌移植瘤的放疗疗效具有重要价值,放疗后6d是一个合适的时间点;18F-FDG PET-CT结合Ki67的表达变化可以反映鼻咽癌的放疗敏感性。 -
关键词:
- 鼻咽肿瘤 /
- 小鼠, 裸 /
- X线疗法 /
- 氟脱氧葡萄糖F18 /
- 正电子发射断层显像术 /
- 体层摄影术, X线计算机 /
- Ki-67, 抗原
Abstract:Objective To investigate the value of 18F-FDG PET-CT scans on early assessing the therapeutic effects on human nasopharyngeal carcinoma(NPC)xenograft in nude mice after radiotherapy, and preliminarily analyze the relation of 18F-FDG PET-CT scans and the positive expression rate of Ki67, and provide a basis for further clinical studies. Methods Fifteen xenograft nude mice of NPC were randomly divided into three groups(5 nude mice per group).Control group: all mice immediately executed after the 18FFDG PET-CT scans and taken pathology; 6 Gy radiotherapy group: all mice took 18F-FDG PET-CT scans before and 1 d after receiving 6 Gy irradiation, and were killed immediately to take pathology; 12 Gy radiotherapy group: all mice received 12 Gy irradiation(6 Gy each time, totally 2 times).They took 18F-FDG PET-CT scans before radiotherapy, after receiving the first 6 Gy irradiation, 2 d and 6 d after receiving 12 Gy irradiation respectively, and then were executed to take pathology after the last scan. The expression of Ki67 in xenografts of different groups was detected and the relation between their changes and T/NT were analyzed. Results ① For 12 Gy radiotherapy group, the average T/NT ratios of the NPC xenograft of pre-radiotherapy, after the first 6 Gy irradiation, 2 d and 6 d after 12 Gy radiotherapy were 2.17±0.31, 1.68±0.42, 1.41±0.40, and 0.70±0.12, respectively. The average T/NT ratios were not statistically difference before and after the first 6 Gy irradiation. The average T/NT ratio of 2 d after radiotherapy decreased significantly than pre-radiotherapy (t=2.80, P < 0.05) and after the first 6 Gy irradiation(t=3.14, P < 0.05); The average T/NT ratio of 6d after radiotherapy was decreased seriously than 2 d after radiotherapy (t=3.49, P < 0.05, compared with pre-radiotherapy t=8.01, P < 0.01). ② The positive expression rates of Ki67 of NPC xenograft markedly decreased after receiving irradiation. There were significant differences in the positive expressions of Ki67 between different groups(F=21.95, P < 0.01).The positive expression of Ki67 in the 12 Gy radiotherapy group decreased significantly compared with the control group (t=7.145, P < 0.01) and the 6 Gy radiotherapy group (t=2.384, P < 0.05). The positive expression of Ki67 in the 6 Gy radiotherapy group was less than the control group, also have statistical significance(t=4.320, P < 0.01).③There was no correlation between the T/NT ratio of NPC xenograft and the positive expression of Ki67. ④Positive correlation was found between the variance of T/NT ratio and the variance of the positive expression of Ki67 of NPC xenograft (r=0.532, P < 0.05). Conclusions 18F-FDG PET-CT imaging has an important value on early assessing the therapeutic effects of NPC xenograft in nude mice after radiotherapy, and the 6th day after radiotherapy is an appropriate time point.18F-FDG PET-CT imaging can reflect the variance of the positive expression of Ki67 of NPC, and yet indirectly reflect the sensitivity of NPC to radiotheraphy. -
表 1 不同实验组裸鼠的肿瘤细胞死亡率情况
肿瘤细胞死亡率(%) ≤25 25~50 51~75 > 75 对照组 5 0 0 0 6 Gy放疗组 0 3 2 0 12 Gy放疗组 0 1 0 4 -
[1] Teo PM, Kwan WH, Chan AT, et al. How successful is highdose(> or=60 Gy)reirradiation using mainly external beams in salvaging local failures of nasopharyngeal carcinoma?. Int J Radiat Oncol Biol Phys, 1998, 40(4): 897-913. doi: 10.1016/S0360-3016(97)00854-7 [2] Lee AW, Foo W, Law SC, et al. Reirradiation for recurrent nasoph-aryngeal carcinoma: factors affecting the therapeutic ratio and ways for improvement. Int J Radiat Oncol Biol Phys, 1997, 38(1): 43-52. doi: 10.1016/S0360-3016(97)00244-7 [3] 韦祝新, 王绍丰. Ki67基因在鼻咽癌中的表达及其意义. 广西医科大学学报, 2002, 19(6): 787-789. doi: 10.3969/j.issn.1005-930X.2002.06.008
[4] 石小燕, 胡国清, 曹荣华. Ki67在鼻咽癌中的表达及意义. 肿瘤防治研究, 2004, 31(1): 4-6. doi: 10.3971/j.issn.1000-8578.2043
[5] Fang FM, Tsai WL, Go SF, et al. Imp lications of quantitative tumor and nodal regression rates for nasopharyngeal carcinomas after 45Gy of radiotherapy. Int J Radiat Oncol Biol Phys, 2001, 50(4): 961-969. doi: 10.1016/S0360-3016(01)01531-0 [6] Brun E, Kjellen E, Tennvall J, et al. FDG PET studies during treat-ment: prediction of therapy outcome in head and neck squamous cell carcinoma. Head Neck, 2002, 24(2): 127-135. doi: 10.1002/hed.10037 [7] Molthoff CF, Klabbers BM, Berkhof J, et al. Monitoring response to radiotherapy in human squamous cell cancer bearing nude mice: comparison of 2′-deoxy-2′-[18F]fluoro-D-glucose(FDG)and 3′-[18F]fluoro-3′-deoxythymidine(FLT). Mol Imaging Biol, 2007, 9(6): 340-347. doi: 10.1007/s11307-007-0104-5 [8] Cher LM, Murone C, Lawrentschuk N, et al. Correlation of hypoxic cell fraction and angiogenesis with glucose metabolic rate in gliomas using18F-fluoromisonidazole, 18F-FDG PET, and immuno histochemi-cal studies. J Nucl Med, 2006, 47(3): 410-418. [9] Shimoda W, Hayashi M, Murakami K, et al. The relationship between FDG uptake in PET scans and biological behavior in breast cancer. Breast Cancer, 2007, 14(3): 260-268. doi: 10.2325/jbcs.14.260 [10] Buck AC, Schirrmeister HH, Guhlmann CA, et al. Ki-67 immunost aining in pancreatic cancer and chronic active pancreatitis: does in vivo FDG uptake correlate with proliferative activity?. J Nucl Med, 2001, 42(5): 721-725. [11] Sheridan MT, O′Dwyer T, Seymour CB, et al. Potential indicators of radiosensitivity in squamous cell carcinoma of the head and neck. Radiat Oncol Investig, 1997, 5(4): 180-186. doi: 10.1002/(SICI)1520-6823(1997)5:4<180::AID-ROI3>3.0.CO;2-U -






 下载:
下载: