-
随着社会的发展和饮食结构的变化,牙髓病和根尖周疾病患者的数量逐年增加。目前,根管治疗(root canal treatment,RCT)是临床治疗牙髓病和根尖周疾病最为有效的方法[1]。近年来,口腔学的研究逐渐深入和成熟,超声治疗器械、镍钛器械、显微镜系统的使用使RCT的成功率不断提高,但根管的解剖结构较为复杂且根管口至根尖区的形态变化较大,因此RCT的术前诊断和成像尤为重要[2]。影像技术是辅助RCT重要的检查和成像手段,目前常见的影像检查方法为数字化根尖片,其可以显示牙冠的全貌、根管的弯曲程度以及根尖周的硬组织情况,具有操作简单方便、辐射剂量小等特点[3]。但数字化根尖片为二维图像,对情况较为复杂的牙齿进行拍摄易出现影像重叠、变形等问题,给医师阅片带来了较大困难[4]。锥形束CT(cone beam computed tomography,CBCT)是一种较为先进的口腔影像检查方法[5]。其采用锥形X射线束投照,射线围绕患者扫描后由平板探测器接收,最后由计算机接收信号并进行分析,完成三维成像[6]。CBCT可以通过矢状面、冠状面和横断面成像,具有较高的空间分辨率,可以有效避免数字化根尖片出现的影像重叠、变形等问题,但可能会受到射线硬化和散射现象的影响导致图像清晰度降低[5]。本研究对比了CBCT联合数字化根尖片与根尖片评估RCT疗效的作用,以期为临床医师评估RCT的疗效提供理论依据。
-
回顾性分析2021年1至12月于沧州市人民医院就诊的需行RCT的84例患者的临床资料,其中男性45例、女性39例,年龄(42.7±10.4)岁。纳入标准:(1)牙根完整,无内吸收、外吸收或根管钙化等;(2)既往病史、用药史等病历资料完整;(3)无严重全身性疾病;(4)患牙为上颌或下颌第一或第二磨牙。排除标准:(1)患其他口腔疾病;(2)存在认知和精神障碍;(3)失访。采用随机数字表法将患者分为观察组(42例)和对照组(42例)。其中对照组男性21例、女性21例,年龄20~65(42.9±10.4)岁。观察组男性24例、女性18例,年龄18~64(42.6±10.6)岁。2组患者一般资料的差异均无统计学意义(均P>0.05)。
对照组患者共54颗患牙,其中上颌第一磨牙11颗、第二磨牙12颗,下颌第一磨牙13颗、第二磨牙18颗。观察组患者共56颗患牙,其中上颌第一磨牙13颗、第二磨牙10颗,下颌第一磨牙14颗、第二磨牙19颗。
所有作者均在检查前签署了知情同意书。本研究经沧州市人民医院伦理委员会批准[批准号:K2020-批件-144(12.9)]。
-
对照组患者使用显微镜(德国蔡司OPMI PROergo型)行RCT,治疗前需利用牙片机(芬兰SOREDEX公司INTR型)拍摄初始根尖片,大致了解患牙牙根形态及数目。行RCT时常规开髓拔髓,使用K锉疏通根管,使用电子根尖定位仪(德国VDW公司RAYPEX6型)对根尖定长,结合主尖片,在距离根尖孔0~5 mm处确定根管长度,彻底清理根管后将牙胶尖放入根管,上下轻轻提拉排除气泡,去除根管口外多余牙胶尖并垂直加压。设置携热器(德国VDW公司ReciprocBlue型)的温度,将选定的携热器工作尖间断加热、加压插入主牙胶尖的根管内,到达距根尖3~5 mm处稍作停顿,再次间断加热并切断主牙胶尖,将上段牙胶无阻力取出,用对应的小号垂直加压器向根尖适度加压,使牙胶尖严密填充根尖处及侧枝根管,之后用热牙胶回填根管冠方2/3部分,每次填充长度约2 mm,并垂直加压。填充完成后进行图像的后处理并阅片。
观察组患者采用数字化根尖片联合CBCT扫描辅助行RCT。RCT前患者先行CBCT(美国Kodak公司DirectView DR9500型)扫描,扫描参数:管电压84 kV、管电流10 mA,曝光时间10.8 s,体素0.3 mm×0.3 mm,扫描视野15 cm×18 cm。扫描后在系统自带软件中进行图像后处理,对患牙的矢状面、冠状面及横断面进行三维重建并阅片。CBCT扫描完成并阅片后开始辅助行RCT,使用电子根尖定位仪对根尖定长,结合主尖片,在距离根尖孔0~5 mm处确定根管长度,具体操作方式同对照组,完成RCT后在系统自带软件中进行图像后处理和阅片。
-
比较2组患者根管的填充长度,评价标准分为以下3种。(1)超填:填充材料超出根尖孔(图1A);(2)恰填:填充材料距根尖0.5~2 mm,根尖封闭严密(图1B);(3)欠填:填充材料距根尖>2 mm,根尖封闭不严密(图1C)。计算恰填率,其公式为:恰填率(%)=恰填根管数/(恰填根管数+超填根管数+欠填根管数)×100%。
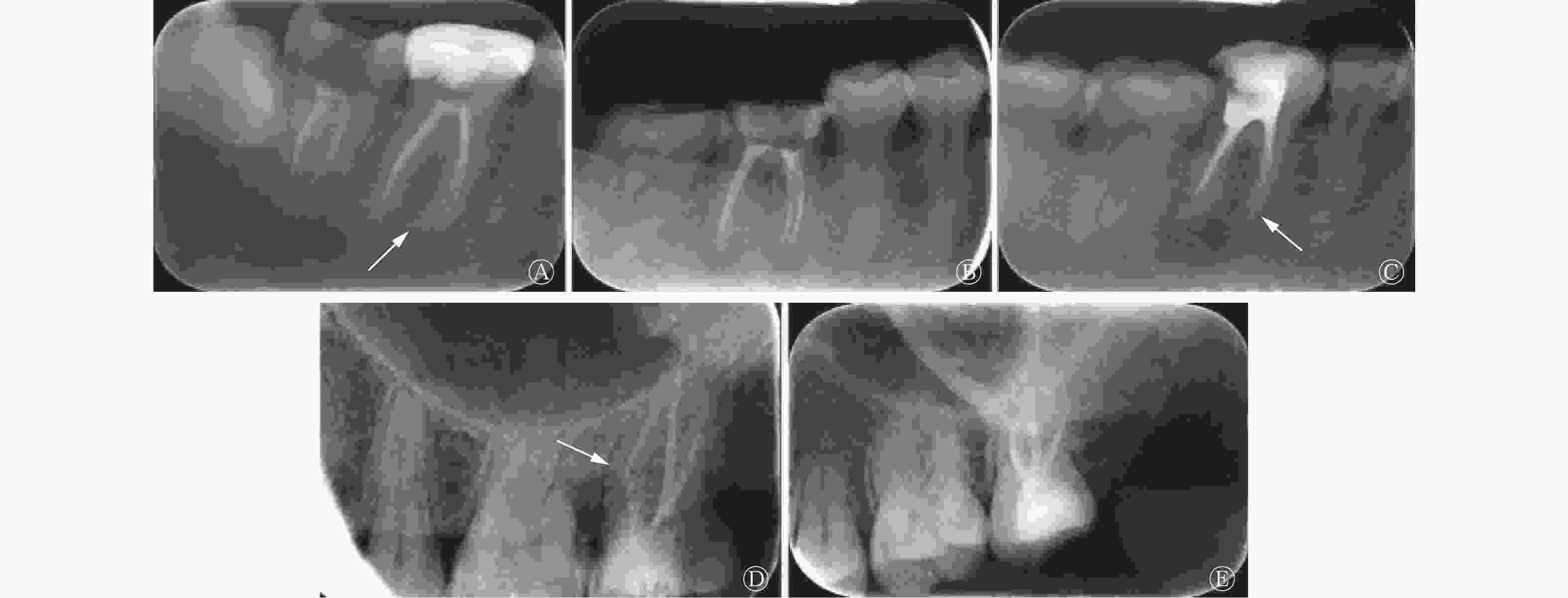
图 1 根管治疗患者患牙根管填充情况示意图
Figure 1. Root canal filling images of affected teeth in patients with root canal treatment
比较2组患者根管填充的致密度,评价标准分为以下2种。(1)不致密:根管填充材料与根管壁间有明显可见的空隙或填充密度稀疏(图1D);(2)致密:根管填充物与根管壁紧密贴合,致密均匀,无空隙(图1E)。计算2组患者的填充致密度合格率,其公式为:填充致密度合格率(%)=填充致密患牙数/(填充致密患牙数+填充不致密患牙数)×100%。
由2名具有10年以上工作经验的影像科主任医师对患者的根尖图像进行分析,并独立判断根管填充的长度和致密度,意见不一致时以第3位主任医师的意见为准。所有患者均每3个月复诊1次,共复诊3次。
比较2组患者的预后,预后评价分为治愈、缓解和失败。(1)治愈:患者主诉无不适,根尖封闭严密,影像检查无根尖低密度影;(2)缓解:患者主诉无不适,根尖封闭严密,影像检查示根尖低密度影缩小;(3)失败:患者主诉有不适或填充材料超出根尖孔或者可见明显空隙,影像检查示根尖低密度影未变小或增大。计算2组患者的治愈率,其公式为:治愈率(%)=治愈患者数/(治愈患者数+缓解患者数+失败患者数)×100%。
-
应用SPSS 22.0软件对数据进行统计学分析。计数资料以百分比(%)表示,组间比较采用χ2检验。P<0.05为差异有统计学意义。
-
对照组上颌第一磨牙的恰填率为65.71%(23/35),明显低于观察组[88.10%(37/42)],且差异有统计学意义(χ2=5.560,P=0.018)。对照组上颌第二磨牙的恰填率为71.43%(25/35),与观察组[85.71%(24/28)]的差异无统计学意义(χ2=1.837,P=0.294)。
对照组下颌第一磨牙的恰填率为74.00%(37/50),与观察组[86.27%(44/51)]的差异无统计学意义(χ2=2.395,P=0.194)。对照组下颌第二磨牙的恰填率为68.29%(28/41),明显低于观察组[87.50%(42/48)],且差异有统计学意义(χ2=4.858,P=0.028)。
-
对照组患者根管填充致密度合格率为68.52%(37/54),明显低于观察组[85.71%(48/56)],且差异有统计学意义(χ2=4.630,P=0.031)。
-
对照组患者3次复诊后的治愈率为76.19%(32/42),明显低于观察组[92.86%(39/42)],且差异有统计学意义(χ2=4.459,P=0.034)。
-
随着口腔医学的发展,医学影像与口腔疾病治疗的关系越来越紧密,其中数字化根尖片是目前辅助行RCT的主要方法之一[7]。但数字化根尖片为二维平面图像,在临床上常出现影像重叠、变形等问题,给临床医师的判读带来一定困难[8]。CBCT由X线发生器以10 mA左右的电流发射射线,围绕牙齿进行数字式投照,被照射的牙齿进行连续投照后获取的数据在计算机中重组并获得三维图像[9]。相较于传统的二维数字化根尖片,CBCT对圆形根、扁圆形根、C形根以及各种融合根牙齿的观察更为立体,可以从矢状面、冠状面和横断面任一平面对牙体进行观察,更加真实地重现牙体的原有结构和形态,为指导和评价RCT提供可靠的依据,同时也降低了医生阅片的难度[10]。Talabani等[11]研究发现,CBCT能够无创地对根管成像并进行高精度的形态分析,对根管数目、解剖形态、根尖孔位置的评价更为准确,对形态复杂的牙齿具有更好的成像效果。本研究结果表明,CBCT可以清晰地显示患者根管的形态和根尖的填充情况,与Talabani等[11]的研究结果一致。Chen等[12]研究发现,CBCT的辐射剂量高于X射线检查,三维图像的清晰度也不及常规影像检查。Hyun等[13]的研究结果表明,CBCT较高的辐射剂量会对一些特殊患者造成影响,相比X射线检查,其拍摄时间也更长,费用也较高。Patel等[14]的研究结果表明,如果患者的牙齿中存在金属镶嵌物,如种植体、牙冠和填充物,CBCT图像会有严重的条纹和阴影伪影,导致牙齿的形态结构不清晰。因此,本研究中对照组采用数字化根尖片辅助行RCT,观察组采用数字化根尖片联合CBCT扫描辅助行RCT,比较2组患者根管填充质量和患者的预后情况。
恰填率是评价根管填充质量的重要指标之一,恰填率越高说明填充前对牙齿结构的观察越准确[15-16]。本研究中,对照组患者上颌第一磨牙和下颌第二磨牙的恰填率分别为65.71%和68.29%,明显低于观察组的88.10%和87.50%,对照组和观察组患者上颌第二磨牙和下颌第一磨牙恰填率的差异均无统计学意义。不同位置的牙齿使用2种方法的恰填率不同,可能是因为不同位置牙齿结构的复杂程度不同,上颌第一磨牙为体积最大,牙根和根管最复杂的“六龄牙”, 其根管系统在所有牙齿中最复杂多样,出现C型根管的概率也较大,存在一些管间交通、根尖分歧和侧支根管等异常结构,在临床常规术前检查中易漏诊[17]。采用数字化根尖片联合CBCT扫描能够最大程度地降低RCT前的误诊和漏诊,相比单纯使用数字化根尖片检查,其诊断效能有显著的提高。上、下颌第二磨牙是出现C1和C2型根管概率最高的牙齿,C1和C2型根管中存在根尖分歧和侧支根管结构,因此常规的成像无法清晰地显示该区域,难以进行有效的根管填充。因此,数字化根尖片难以满足对牙齿全面观察的要求,CBCT的扇形扫描可以真实地重现牙体的原有结构和形态,有效辅助医师行RCT,减少填充不致密或者超填现象的出现,提高RCT的成功率,改善患者的预后。
CBCT与数字化根尖片结合能够在保证原有根尖片清晰度的同时提高图像的三维空间分辨率,可作为口腔临床诊断和治疗的重要工具,是未来口腔科影像学发展的趋势。根管填充致密度是评价RCT的常见指标之一,根管系统是否能够有效清理是影响根管填充致密度的重要因素之一。我们发现,对照组患者根管填充致密度合格率为68.52%,明显低于观察组的85.71%。这可能是由于RCT前通过影像观察根管的形状和数量可以有效辅助清理根管,增加根管填充的致密度,这与Alhablain等[18]的研究结果一致。本研究对行RCT的患者进行了3次复查,结果表明,对照组患者的治愈率为76.19%,明显低于观察组的92.86%。观察组患者行RCT的成功率较高,患者术后预后较好。在使用数字化根尖片和CBCT时应结合患者的情况,注意使用范围及适应证,在RCT前进行准确评估,改善患者的预后。
本研究的样本量有限,在后续的研究中,我们将扩大样本量,收集更多的数字化根尖片联合CBCT对根管进行治疗的病例,并对患者进行更长时间的随访,更为准确地评估其预后情况。
利益冲突 所有作者声明无利益冲突
作者贡献声明 梁亮负责研究命题的提出与设计、论文的撰写;沈悦、时炳正负责数据的分析;徐志媛、李翠梅负责论文的审阅
数字化根尖片联合锥形束CT对根管治疗疗效评价和预后评估的研究
Evaluation of curative effect and prognosis of root canal therapy by digital apical film combined with cone beam CT
-
摘要:
目的 探究数字化根尖片联合锥形束CT(CBCT)对根管治疗(RCT)疗效评价和预后评估的作用。 方法 回顾性分析2021年1至12月于沧州市人民医院行RCT的84例患者的临床资料,其中男性45例、女性39例,年龄(42.7±10.4)岁。采用随机数字表法将患者分为观察组(42例)和对照组(42例)。对照组采用数字化根尖片辅助行RCT,观察组采用数字化根尖片联合CBCT扫描辅助行RCT。对照组患者共54颗患牙,其中上颌第一、第二磨牙分别为11颗和12颗,下颌第一、第二磨牙分别为13颗和18颗;观察组患者共56颗患牙,其中上颌第一、第二磨牙分别为13颗、10颗,下颌第一、第二磨牙分别为14颗、19颗。采用χ2检验比较2组患者上颌和下颌第一磨牙、第二磨牙的恰填率、根管填充致密度合格率和治愈率。 结果 对照组上颌第一磨牙、下颌第二磨牙的恰填率均低于观察组[65.71%(23/35)对88.10%(37/42)、68.29%(28/41)对87.50%(42/48)],且差异均有统计学意义(χ2=5.560、4.858,均P<0.05)。对照组上颌第二磨牙、下颌第一磨牙的恰填率均低于观察组[71.43% (25/35) 对85.71% (24/28)、74.00% (37/50) 对86.27% (44/51)],差异均无统计学意义(χ2=1.837、2.395,均P>0.05)。对照组患者根管填充致密度合格率低于观察组[68.52%(37/54)对85.71%(48/56)],且差异有统计学意义(χ2=4.630,P<0.05)。对照组3次复诊后的治愈率低于观察组[76.19%(32/42)对92.86%(39/42)],且差异有统计学意义(χ2=4.459,P<0.05)。 结论 联合使用CBCT与数字化根尖片作为RCT疗效的评估手段,对RCT根管填充长度及严密程度的评价更为准确,可有效改善患者的预后。 -
关键词:
- 锥束计算机体层摄影术 /
- 根管治疗 /
- 数字化根尖片
Abstract:Objective To explore the role of digital apical film combined with cone beam computed tomography (CBCT) in the evaluation of curative effect and prognosis of root canal therapy (RCT). Methods The clinical data of 84 patients who underwent RCT, including 45 males and 39 females, aged (42.7±10.4) years, in Cangzhou People's Hospital from January 2021 to December 2021 were analyzed retrospectively. The patients were divided into observation (n=42) and control (n=42) groups using the random number table method. Apical film was used to assist in the RCT of the control group, and apical film combined with CBCT scanning was used during the RCT of the observation group. A total of 54 teeth, including 11 maxillary first molars, and 12 maxillary second molars, 13 mandibular first molars, and 18 mandibular second molars were observed in the control group. A total of 56 teeth were detected in the observation group, exactly 13 maxillary first molars and 10 maxillary second molars were recorded, respectively, meanwhile, 14 and 19 mandibular first and second molars were identified, respectively. Proper filling rates and qualified rates of dense root canal filling of the maxillary first and second molars and mandibular first and second molars in two groups were compared by χ2 test. Results The control group showed lower proper filling rates of the maxillary first molars and mandibular second molars compared with the observation group (65.71%(23/35) vs. 88.10%(37/42), 68.29%(28/41) vs. 87.50%(42/48)), and the differences were statistically significant (χ2=5.560, 4.858; both P<0.05). The control group also presented lower proper filling rates of maxillary second molars and mandibular first molars than the observation group (71.43% (25/35) vs. 85.71% (24/28), 74.00% (37/50) vs. 86.27% (44/51)), but the differences showed no statistical significance (χ2=1.837, 2.395; both P>0.05). A lower qualified rate of dense root canal filling was observed in the control group than that in the observation group (68.52% (37/54) vs. 85.71% (48/56)), and the difference was statistically significant (χ2=4.630, P<0.05). The control group exhibited a lower cure rate after three revisits compared with the observation group (76.19% (32/42) vs. 92.86% (39/42)), and the difference was statistically significant (χ2=4.459, P<0.05). Conclusions CBCT combined with digital apical film as evaluation methods for the curative effect of RCT, the evaluation of the length and severity of root canal filling of RCT becomes more accurate and can effectively improve the prognosis of patients. -
Key words:
- Cone-beam computed tomography /
- Root canal treatment /
- Digital apical film
-
[1] Adam M. 'Combined endo-perio lesions'-what is the best treatment[J]. Evid Based Dent, 2021, 22(4): 158−159. DOI: 10.1038/s41432-021-0230-y. [2] Lamira A, Mazzi-Chaves JF, Nicolielo LFP, et al. CBCT-based assessment of root canal treatment using micro-CT reference images[J]. Imaging Sci Dent, 2022, 52(3): 245−258. DOI: 10.5624/isd.20220019. [3] Meirinhos J, Martins JNR, Pereira B, et al. Prevalence of apical periodontitis and its association with previous root canal treatment, root canal filling length and type of coronal restoration–a cross-sectional study[J]. Int Endod J, 2020, 53(4): 573−584. DOI: 10.1111/iej.13256. [4] Yapp KE, Brennan P, Ekpo EU. Endodontic disease detection: digital periapical radiography versus cone-beam computed tomography-a systematic review[J]. J Med Imaging (Bellingham), 2021, 8(4): 041205. DOI: 10.1117/1.JMI.8.4.041205. [5] Quaresma SA, Da Costa RP, Ferreira Petean IB, et al. Root canal treatment of severely calcified teeth with use of cone-beam computed tomography as an intraoperative resource[J]. Iran Endod J, 2022, 17(1): 39−47. DOI: 10.22037/iej.v17i1.36153. [6] Chogle S, Zuaitar M, Sarkis R, et al. The recommendation of cone-beam computed tomography and its effect on endodontic diagnosis and treatment planning[J]. J Endod, 2020, 46(2): 162−168. DOI: 10.1016/j.joen.2019.10.034. [7] Setzer FC, Lee SM. Radiology in endodontics[J]. Dent Clin North Am, 2021, 65(3): 475−486. DOI: 10.1016/j.cden.2021.02.004. [8] Mark AM. Dental X-rays[J]. J Am Dent Assoc, 2019, 150(7): 636. DOI: 10.1016/j.adaj.2019.05.002. [9] Pereira ABN, Almeida R, Artese F, et al. External root resorption evaluated by CBCT 3D models superimposition[J]. Dental Press J Orthod, 2022, 27(2): e2219315. DOI: 10.1590/2177-6709.27.2.e2219315.oar. [10] Nasseh I, Al-Rawi W. Cone beam computed tomography[J]. Dent Clin North Am, 2018, 62(3): 361−391. DOI: 10.1016/j.cden.2018.03.002. [11] Talabani RM. Assessment of root canal morphology of mandibular permanent anterior teeth in an Iraqi subpopulation by cone-beam computed tomography[J]. J Dent Sci, 2021, 16(4): 1182−1190. DOI: 10.1016/j.jds.2021.02.010. [12] Chen LY, Liang X, Shen CY, et al. Synthetic CT generation from CBCT images via deep learning[J]. Med Phys, 2020, 47(4): 1115−1125. DOI: 10.1002/mp.13978. [13] Hyun CM, Bayaraa T, Yun HS, et al. Metal artifact reduction with intra-oral scan data for 3D low dose maxillofacial CBCT modeling[J]. 2022, 8(2): 1−13. DOI: 10.48550/arXiv.2202.03571. [14] Patel S, Durack C, Abella F, et al. European Society of Endodontology position statement: the use of CBCT in endodontics[J]. Int Endod J, 2014, 47(6): 502−504. DOI: 10.1111/iej.12267. [15] Brochado Martins JF, Guerreiro Viegas O, Cristescu R, et al. Outcome of selective root canal retreatment-a retrospective study[J]. Int Endod J, 2023, 56(3): 345−355. DOI: 10.1111/iej.13871. [16] Worthington HV, Khangura S, Seal K, et al. Direct composite resin fillings versus amalgam fillings for permanent posterior teeth[J/OL]. Cochrane Database Syst Rev, 2021, 8(8): CD005620[2023-07-05]. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8407050/. DOI: 10.1002/14651858.CD005620.pub3. [17] Krishnamurthy NH, Athira P, Umapathy T, et al. A CBCT study to evaluate the root and canal morphology of permanent maxillary first molars in children[J]. Int J Clin Pediatr Dent, 2022, 15(5): 509−513. DOI: 10.5005/jp-journals-10005-2441. [18] Alhablain EA, Durr-e-Sadaf, Ahmad MZ, et al. Quality of root canal therapy (RCT) performed by the undergraduate students at the Qassim University, Kingdom of Saudi Arabia (KSA)[J]. Med Forum, 2018, 29(6): 80−84. -





 下载:
下载:

