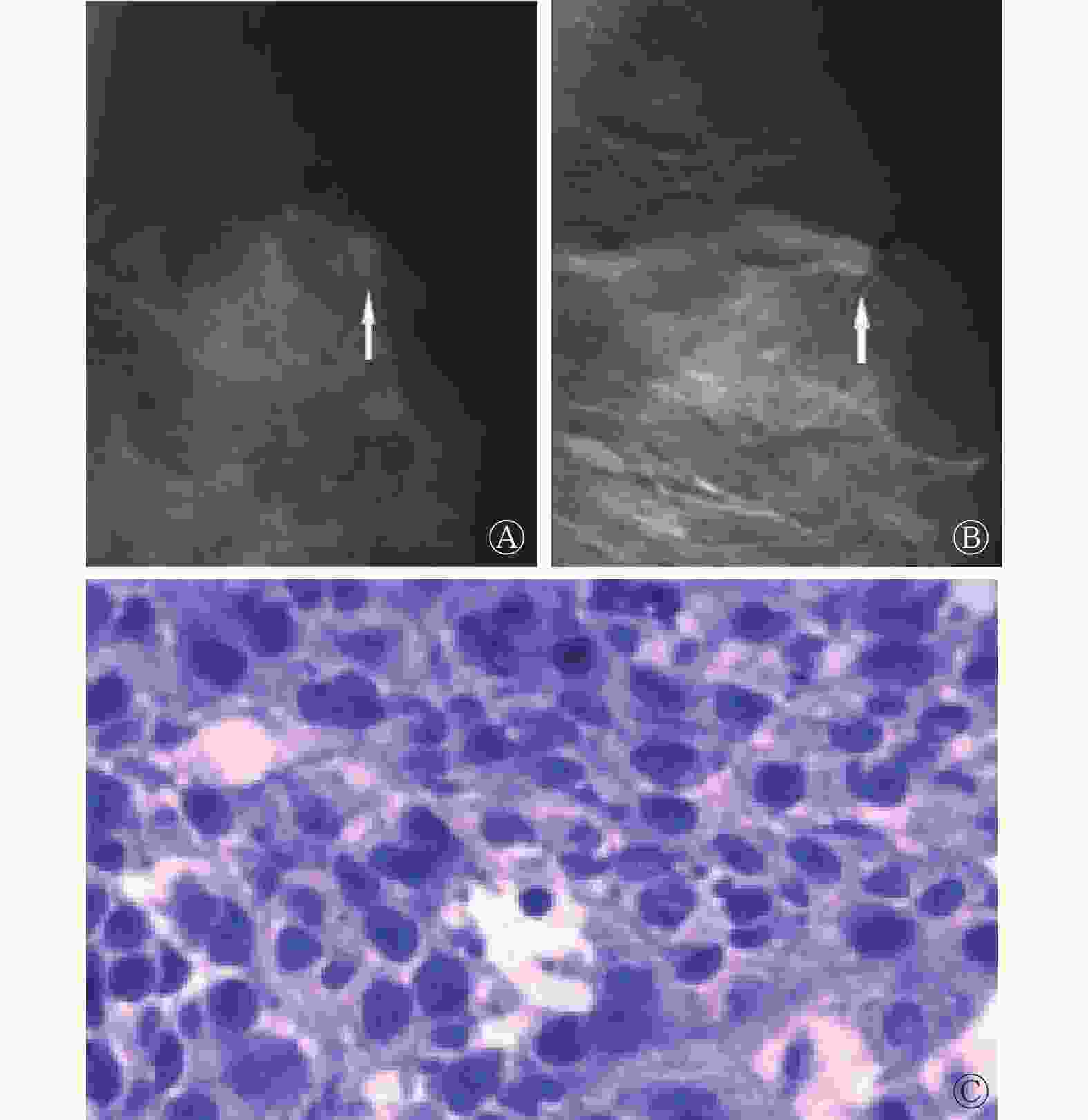
-
近年来,乳腺癌的发病率持续上升,且发病人群年龄逐渐趋于年轻化,其已成为威胁女性健康的重大恶性疾病之一[1]。乳腺癌筛查的普及、早期发现和诊断可以指导临床及时制定合理的手术方案,是降低乳腺癌患者病死率的重要举措[2]。早期乳腺癌是指肿瘤长径<2 cm、腋窝无淋巴结转移、无远处转移的乳腺癌。目前,乳腺癌的早期筛查主要通过乳腺自检、临床触诊检查以及影像检查等方法,虽然乳腺肿块是早期乳腺癌最常见的症状,但部分早期乳腺癌可无明显症状与体征,存在临床触诊阴性的情况,因此,定期进行影像检查很有必要。常规全数字化乳腺X射线摄影(full-field digital mammography,FFDM)因具有操作简单、分辨率良好、经济及可重复操作等优势,成为目前临床乳腺癌筛查的主要影像检查手段之一,但由于其属于二维图像,存在组织重叠效应,容易出现漏诊及误诊情况,进而影响了筛查结果的准确率[3]。随着影像技术的发展,数字乳腺断层融合X射线成像(digital breast tomosynthesis,DBT)技术出现在人们的视野中,其作为一种三维成像技术,可以在不同角度获得乳腺的影像,明显降低组织重叠的影响,因此能更清晰地显示乳腺内部结构和病灶,提高乳腺病灶的检出率及筛查的准确率[4]。但因乳腺对X射线较敏感,DBT对其的辐射危害亦需要重视。有研究者报道,可通过降低X射线机球管的管电压和管电流,从而降低辐射剂量,实现低剂量X射线摄影成像[5]。而低剂量DBT是否对早期乳腺癌具有良好的诊断价值尚需进一步探讨。基于此,本研究探讨了低剂量DBT和FFDM在早期乳腺癌筛查中的应用价值,现报道如下。
-
前瞻性选取2020年1月至2022年3月在聊城市第二人民医院就诊的以乳腺肿块、乳腺胀痛为主要表现的246例患者,患者均为女性,年龄(47.3±6.2)岁,范围28~65岁。临床表现:乳房肿块246例、乳腺胀痛95例;临床触诊乳腺肿块长径(3.0±0.8)cm,范围0.7~6.4 cm。纳入标准:①均存在乳腺肿块,伴或不伴乳腺胀痛;②无X射线检查禁忌证,均接受FFDM和低剂量DBT检查;③接受超声引导下的穿刺活检。排除标准:①既往有手术治疗或放、化疗史;②既往乳腺癌病史;③合并严重的心、肝、肾功能障碍;④合并精神疾病或认知功能障碍;⑤合并其他恶性肿瘤;⑥凝血功能异常者;⑦合并全身性感染或自身免疫性疾病等;⑧处于妊娠期或哺乳期。
所有患者均于检查前签署了知情同意书。本研究获得了聊城市第二人民医院伦理委员会批准(批准号:201912-001)。
-
使用美国Hologic公司Selenia Dimensions数字乳腺X射线摄影系统进行FFDM和DBT检查。所有患者常规体位选择双侧乳腺头尾(craniocaudal,CC)位及乳腺内外斜(mediolateral oblique,MLO)位,必要时根据患者个体差异和检查情况进行特殊体位或局部放大处理。同一患者先行低剂量DBT检查(以降低X射线机球管管电流来实现),再行FFDM检查。DBT检查:曝光时选取适当的压力值对乳腺组织予以适度加压,采用OPDOSE曝光模式自动曝光,维持压迫,将X射线机球管在围绕乳房−25°~25°角度范围内进行旋转,曝光次数为每旋转2°自动曝光1次,均采取低剂量曝光方式,X射线管电压20~49 kV,步长1 kV,电功率3.0 kW,管电流10~400 mA,扫描时间<4 s,DBT重建层厚1 mm,重建时间2~5 s,总层数与患者乳腺组织厚度相等。另在同一压迫条件下(仍在自动曝光模式下),计算机再自动将所有断层图像重新组合在一起,融合成二维图像进行FFDM检查。记录曝光时所检测的每例患者的腺体剂量(CC位及MLO位)。
-
由2名具有5年以上乳腺影像阅片及诊断经验的影像科医师分别独立判断FFDM和DBT图像,在Hologic工作站5M显示器上进行分析。2名医师在阅片时可参考患者就诊时的临床症状表现、病史及一般乳腺查体记录,但并不知晓组织病理学检查结果,且在阅读DBT图像时,可根据需要选择不同层厚的图像进行观察。对于同一例患者的FFDM和DBT图像,选择不同时间(阅片时间间隔2周)进行判读。观察与记录乳腺病灶形态、乳腺构成分类,其中病灶形态包括肿块、钙化、结构扭曲和不对称致密影;乳腺构成分类和乳腺影像报告和数据系统(breast imaging reporting and data system,BI-RADS)病灶分类均参照《乳腺影像数据与报告系统:2013版》[6]进行判定。2名医师在阅读图像时均参照BI-RADS病灶分类标准[6]进行独立阅片和分析,当意见不统一时,则由第3位更高年资的影像科医师根据该标准来进行判断。影像科医师阅读FFDM、DBT图片时,分别对病灶进行BI-RADS 0~5类诊断,将BI-RADS 4B、4C、5类病灶定义为阳性,4A类及以下病灶定义为阴性。FFDM联合DBT筛查的诊断标准为FFDM和DBT图像的综合诊断结果,即通过FFDM和DBT分别对病灶进行BI-RADS 0~5类诊断,综合这两种影像诊断结果,若任意一项影像检查对病灶定义为阳性,则联合诊断为阳性。
-
所有患者均于影像检查后在超声引导下行穿刺活检,活检组织由聊城市第二人民医院病理检验科进行检查。对于活检结果存有疑问或不能完全明确诊断者,则进一步通过手术取病变组织行组织病理学检查。对于接受手术治疗者,于术中切除病变组织,并于术后行组织病理学检查。由2名具有高级职称的病理科医师对组织病理学检查结果进行判读,并将最终组织病理学检查结果作为诊断早期乳腺癌的“金标准”。
-
采用SPSS 26.0软件对数据进行统计学分析。符合正态分布的计量资料以
$ \bar x \pm {{s}} $ 表示,两组间比较采用t检验(方差齐),多组间比较采用单因素方差分析;计数资料以率(%)表示,组间比较采用χ2检验;采用Kappa检验对FFDM、低剂量DBT、FFDM联合低剂量DBT诊断结果与组织病理学检查结果的一致性进行分析(0.81≤Kappa值≤1.00表示一致性优,0.61≤Kappa值<0.81表示一致性良好,0.41≤Kappa值<0.61表示一致性中等,0.21≤Kappa值<0.41表示一致性一般,Kappa值<0.21表示一致性差)。P<0.05为差异有统计学意义。 -
纳入本研究的246例患者中,经组织病理学检查结果确诊为早期乳腺癌192例(共计199个病灶),其中浸润性导管癌154例、导管原位癌15例、浸润性导管癌合并导管原位癌8例、浸润性小叶癌4例、导管原位癌伴局部微小浸润6例、其他5例。经组织病理学检查结果确诊为乳腺良性病变54例(共计57个病灶),其中乳腺囊性增生36例、乳腺纤维瘤18例。有112例患者行手术治疗,术后组织病理学检查结果显示:浸润性导管癌96例、导管原位癌6例、浸润性导管癌合并导管原位癌4例、导管原位癌伴局部微小浸润6例。
-
由表1可知,246例患者中,经FFDM诊断为早期乳腺癌154例(其中假阳性10例)、乳腺良性病变92例(其中假阴性48例);经低剂量DBT诊断为早期乳腺癌169例(其中假阳性2例)、乳腺良性病变77例(其中假阴性25例);经FFDM联合低剂量DBT诊断为早期乳腺癌177例(其中假阳性3例)、乳腺良性病变69例(其中假阴性18例)。由表2可知,低剂量DBT单独诊断以及FFDM联合低剂量DBT诊断早期乳腺癌的灵敏度、特异度、准确率、阳性预测值和阴性预测值均高于FFDM单独诊断,差异均有统计学意义(均P<0.05);而与FFDM联合低剂量DBT相比,低剂量DBT单独诊断早期乳腺癌的灵敏度、特异度、准确率、阳性预测值和阴性预测值的差异均无统计学意义(均P>0.05)。
影像检查 组织病理学检查 合计 阳性(n=192) 阴性(n=54) FFDM 阳性 144 10 154 阴性 48 44 92 低剂量DBT 阳性 167 2 169 阴性 25 52 77 FFDM联合低剂量DBT 阳性 174 3 177 阴性 18 51 69 注:FFDM为全数字化乳腺X射线摄影;DBT为数字乳腺断层融合X射线成像 表 1 FFDM、低剂量DBT及二者联合与组织病理学检查对早期乳腺癌诊断的结果比较(例)
Table 1. Comparison between full-field digital mammography (FFDM), low-dose digital breast tomosynthesis (DBT), the combination of the two and histopathological examination in the diagnosis of early breast cancer (case)
影像检查 灵敏度 特异度 准确率 阳性预测值 阴性预测值 FFDM 75.00%(144/192) 81.48%(44/54) 76.42%(188/246) 93.51%(144/154) 47.83%(44/92) 低剂量DBT 86.98%a(167/192) 96.30%a(52/54) 89.02%a(219/246) 98.82%a(167/169) 67.53%a(52/77) FFDM联合低剂量DBT 90.63%b(174/192) 94.44%b(51/54) 91.46%b(225/246) 98.31%b(174/177) 73.91%b(51/69) χ2值 19.289 8.376 26.064 11.110 12.965 P值 <0.001 0.015 <0.001 0.003 0.001 注:FFDM为全数字化乳腺X射线摄影;DBT为数字乳腺断层融合X射线成像;a表示与FFDM比较,差异均有统计学意义(χ2=6.000~13.677,均P<0.05);b表示与FFDM比较,差异均有统计学意义(χ2=4.285~20.644,均P<0.05) 表 2 FFDM、低剂量DBT及二者联合诊断早期乳腺癌的效能比较
Table 2. Comparison of efficacy among full-field digital mammography (FFDM), low-dose digital breast tomosynthesis (DBT), and the combination of the two in the diagnosis of early breast cancer
-
FFDM诊断早期乳腺癌结果与组织病理学检查结果具有良好的一致性(Kappa值=0.655),低剂量DBT诊断早期乳腺癌结果与组织病理学检查结果具有良好的一致性(Kappa值=0.722),二者联合诊断早期乳腺癌结果与组织病理学检查结果具有良好的一致性(Kappa值=0.792)。
-
FFDM的腺体剂量为(1.03±0.18) mGy,低剂量DBT的腺体剂量为(1.04±0.19) mGy,二者联合检查的腺体剂量为(1.06±0.21) mGy。FFDM、低剂量DBT、二者联合检查的腺体剂量之间的差异无统计学意义(F=1.529,P=0.217)。FFDM的检查时间为(6.25±0.52) min,低剂量DBT的检查时间为(6.33±0.57) min,两者的差异无统计学意义(t=1.626,P=0.105)。
-
乳腺癌的发病率在我国女性恶性肿瘤中居首位,病死率居第六位,且其发展形势较为严峻[7]。相关报道指出,早期诊断和治疗可使乳腺癌的治愈率达到90%以上[8]。乳腺癌的早期筛查能够帮助患者尽早得到明确诊断和治疗,对促进疾病预后的改善、治愈率的提高具有重要意义。相关研究结果表明,对适龄女性开展有组织、有规律的乳腺癌筛查,以发现癌前病变和早期癌变,并实施规范化的早诊早治,是乳腺癌预防控制的重中之重[9]。近年来,随着乳腺癌筛查技术的不断进步,早期乳腺癌的检出率得到提高,其中FFDM是目前临床应用较为广泛及得到公认的最基本的乳腺癌筛查方法,但对于致密型、多量纤维腺体组织病灶的诊断准确率较低[10]。DBT由传统体层摄影技术发展而来,具有成像时间短、三维成像、连续多点拍照等特点,已在乳腺疾病的筛查和诊断中得到了较好的应用[11]。但低剂量DBT是否对早期乳腺癌的筛查具有较高的灵敏度和特异度尚有待研究探讨。
本研究结果显示,低剂量DBT及其与FFDM联合诊断早期乳腺癌的灵敏度、特异度、准确率、阳性预测值、阴性预测值均高于FFDM单独诊断,但低剂量DBT单独诊断与二者联合诊断的效能的差异无统计学意义。另外,本研究结果显示,低剂量DBT诊断早期乳腺癌结果与组织病理学检查结果的一致性(Kappa值=0.722)较FFDM诊断结果与组织病理学检查结果的一致性(Kappa值=0.655)更优,但较二者联合诊断结果与组织病理学检查结果的一致性(Kappa值=0.792)更差。上述结果提示相较于FFDM,低剂量DBT在早期乳腺癌诊断中具有较高的临床价值,与组织病理学检查结果的一致性良好,但二者联合诊断结果与组织病理学检查结果的一致性更优。FFDM在诊断乳腺癌时,X射线机球管处于固定状态,获得的受检者体位的图像较少,但因乳腺肿块的上方或下方可能存在一部分正常腺体,在进行FFDM诊断时容易出现乳腺肿块与正常纤维腺体组织重叠的情况,导致诊断结果出现假阳性或假阴性,最终影响乳腺癌诊断的准确率[12]。另外,如果正常腺体较致密,则会对乳腺肿块的位置、大小、形态和边缘造成遮盖,且二维图像无法很好地排除正常致密纤维腺体组织对病变的干扰,进而影响阅片医师的判断,导致对乳腺癌的漏诊。DBT检查时,X射线机球管在围绕乳房−25°~25°角度范围内进行多次低剂量曝光,通过不同的投射角度,可将二维图像重组并融合成层厚为1 mm的三维断层图像,使X射线摄影的分辨率得到优化,能够对因组织重叠而藏匿于致密纤维腺体组织中的病灶进行清晰地显示,亦能够检测出FFDM未能发现的小结节病灶,减少了正常纤维腺体组织对病灶显示的影响。同时DBT对单纯肿块、肿块毛刺或分叶征、微小钙化、结构扭曲等的显示较FFDM更好,对致密型病灶的大小、形状和边缘等的成像亦较FFDM更优[13-14],因此可提高乳腺癌的检出率并降低乳腺X射线检查复筛率,提高诊断效能。周蜀川等[15]的研究结果表明,DBT对致密型乳腺纤维腺体组织病变的诊断灵敏度、特异度、准确率分别为88.57%、80.81%、82.83%,优于FFDM[15]。而本研究中得到的低剂量DBT对早期乳腺癌诊断的特异度(96.30%)、准确率(89.02%)及FFDM的诊断效能均较周蜀川等[15]的研究结果有所提高。分析原因可能与样本间存在差异性有关,文献[15]针对的是致密型乳腺患者,而致密型乳腺纤维腺体组织重叠较多,导致致密型乳腺癌的漏诊率和误诊率较高。另外,也有研究结果显示,相较于FFDM,采用DBT诊断乳腺癌可更加准确地测量出病灶大小,并对长径1.0~2.0 cm的肿块显示出更高的诊断特异度[16]。梁畅等[17]的研究结果亦表明,DBT对乳腺“结构扭曲”样病变的诊断效能较FFDM更优,可提高对病灶的检出率。综上,低剂量DBT在早期乳腺癌诊断方面的临床应用价值优于FFDM,可弥补FFDM的不足并突破其局限性,提高诊断的灵敏度、特异度、准确率,提升整体筛查效能,并能够对高危人群进行有效地早期筛查,在早期乳腺癌的诊断中具有良好的应用前景。但是,DBT检查在不同投射过程中可出现运动伪影和钙化点夸大的情况,导致漏诊和误诊,因此,DBT诊断早期乳腺癌的准确率仍有待提升。临床在对乳腺癌高危人群进行筛查时,可将FFDM与低剂量DBT联合应用,以提高筛查和诊断效能。
此外,本研究结果显示,FFDM、低剂量DBT、二者联合检查的腺体剂量的差异无统计学意义,表明低剂量DBT使患者受到的辐射剂量较低,且其与FFDM检查联合时,患者所接受的辐射剂量与单独FFDM检查相当,联合检查并未使患者受到的辐射剂量增加。因此,低剂量DBT及其与FFDM联合使用均具有良好的安全性。另外,FFDM检查时间与低剂量DBT检查时间相近,表明低剂量DBT检查并不会增加患者的检查时间。
综上所述,FFDM、低剂量DBT均是早期乳腺癌诊断的重要影像检查方法,低剂量DBT对早期乳腺癌诊断的灵敏度、特异度和准确率相对更高,且与组织病理学检查结果的一致性良好,为临床对早期乳腺癌的筛查提供了一个灵敏、可靠及安全的检查方法。
利益冲突 所有作者声明无利益冲突
作者贡献声明 姜金杰负责研究命题的提出和设计、研究过程的实施、论文的撰写;韩海林负责数据的获取和分析;付焕杰、杜群、李丹负责病例的收集及随访追踪;肖纪涛负责研究方法的建立、论文最终版本的修订
低剂量DBT成像技术和FFDM在早期乳腺癌筛查中的价值研究
Value research of low-dose DBT and FFDM in screening early breast cancer
-
摘要:
目的 探讨低剂量数字乳腺断层融合X射线成像(DBT)和全数字化乳腺X射线摄影(FFDM)在早期乳腺癌筛查中的价值。 方法 前瞻性选取2020年1月至2022年4月在聊城市第二人民医院就诊的以乳腺肿块、乳腺胀痛为主要表现的246例女性患者[年龄(47.3±6.2)岁,范围28~65岁],均进行常规FFDM及低剂量DBT检查,并在超声引导下行穿刺活检。将活检组织病理学检查结果作为“金标准”,对比分析FFDM、低剂量DBT及二者联合筛查早期乳腺癌的灵敏度、特异度、准确率、阳性预测值、阴性预测值,并分析比较FFDM、低剂量DBT单独检查及二者联合检查与组织病理学检查结果的一致性。比较不同检查方法的腺体剂量和检查时间。计量资料的组间比较采用t检验或单因素方差分析,计数资料的组间比较采用χ2检验,不同检查方法与组织病理学检查结果的一致性分析采用Kappa检验。 结果 纳入研究的246例患者中,经组织病理学检查确诊为早期乳腺癌192例、乳腺良性病变54例;经FFDM诊断为早期乳腺癌154例、乳腺良性病变92例;经低剂量DBT诊断为早期乳腺癌169例、乳腺良性病变77例;经FFDM联合低剂量DBT诊断为早期乳腺癌177例、乳腺良性病变69例。低剂量DBT诊断早期乳腺癌的灵敏度(86.98%)、特异度(96.30%)、准确率(89.02%)、阳性预测值(98.82%)和阴性预测值(67.53%)均高于FFDM(75.00%、81.48%、76.42%、93.51%、47.83%),且差异均有统计学意义(χ2=6.000~13.677,均P<0.05);FFDM联合低剂量DBT诊断早期乳腺癌的灵敏度(90.63%)、特异度(94.44%)、准确率(91.46%)、阳性预测值(98.31%)和阴性预测值(73.91%)均高于FFDM,且差异均有统计学意义(χ2=4.285~20.644,均P<0.05);与FFDM联合低剂量DBT相比,低剂量DBT单独诊断早期乳腺癌的灵敏度、特异度、准确率、阳性预测值和阴性预测值的差异均无统计学意义(χ2=0.159~1.283,均P>0.05)。FFDM诊断早期乳腺癌结果与组织病理学检查结果具有良好的一致性(Kappa值=0.655),低剂量DBT诊断早期乳腺癌结果与组织病理学检查结果具有良好的一致性(Kappa值=0.722),FFDM联合低剂量DBT诊断早期乳腺癌结果与组织病理学检查结果具有良好的一致性(Kappa值=0.792)。FFDM[(1.03±0.18)mGy]、低剂量DBT[(1.04±0.19)mGy]及二者联合检查[(1.06±0.21)mGy]的腺体剂量的差异无统计学意义(F=1.529,P>0.05),FFDM检查时间[(6.25±0.52)min]与低剂量DBT检查时间[(6.33±0.57)min]的差异无统计学意义(t=1.626,P>0.05)。 结论 相较于FFDM,低剂量DBT在早期乳腺癌筛查中的应用价值更高,且与组织病理学检查结果的一致性良好,可作为临床对早期乳腺癌进行筛查的重要检查手段。 Abstract:Objective To explore the value of low-dose digital breast tomosynthesis (DBT) and full-field digital mammography (FFDM) in screening early breast cancer. Methods 246 female patients (age (47.3±6.2) years old, ranging from 28 to 65 years old) with breast lumps and breast swelling pain treated in the Second People's Hospital of Liaocheng from January 2020 to April 2022 were prospectively selected. All patients underwent routine FFDM and low-dose DBT examinations, and underwent ultrasound-guided puncture biopsy. The pathological examination results of biopsy tissue was taken as the "gold standard", and the sensitivity, specificity, accuracy, positive predictive value and negative predictive value of FFDM, low-dose DBT and combination of the two in screening early breast cancer were compared and analyzed, and the consistency (Kappa value) between FFDM, low-dose DBT, alone and combination examination of the two and histopathological examination results were analyzed and compared. The average glandular dose and examination time of different examination methods were compared. The intergroup comparison of quantitative data adopted t test or one-way analysis of variance, while the intergroup comparison of counting data adopted χ2 test, and analysis of consistency between different examination methods and histopathological examination results adoptedKappa test. Results Of the 246 patients included in the study, 192 cases were diagnosed as early breast cancer and 54 cases were diagnosed as benign breast lesions by histopathological examination. 154 cases of early breast cancer and 92 cases of benign breast lesions were diagnosed by FFDM. 169 cases of early breast cancer and 77 cases of benign breast lesions were diagnosed by low-dose DBT. 177 cases of early breast cancer and 69 cases of benign breast lesions were diagnosed by FFDM combined with low-dose DBT. The sensitivity (86.98%), specificity (96.30%), accuracy (89.02%), positive predictive value (98.82%) and negative predictive value (67.53%) of low-dose DBT in the diagnosis of early breast cancer were higher than those of FFDM (75.00%, 81.48%, 76.42%, 93.51% and 47.83%), and the differences were statistically significant (χ2=6.000~13.677, all P<0.05). The sensitivity (90.63%), specificity (94.44%), accuracy (91.46%), positive predictive value (98.31%) and negative predictive value (73.91%) of FFDM combined with low-dose DBT in the diagnosis of early breast cancer were higher than those of FFDM, and the differences were statistically significant (χ2 =4.285~20.644, all P<0.05). There was no significant difference in the sensitivity, specificity, accuracy, positive predictive value and negative predictive value between low-dose DBT alone and FFDM combined with low-dose DBT in diagnosing early breast cancer (χ2=0.159~1.283, all P>0.05). The results of FFDM in the diagnosis of early breast cancer has good consistency with the histopathological examination results (Kappa value=0.655), and the results of low-dose DBT in the diagnosis of early breast cancer has good consistency with the histopathological examination results (Kappa value=0.722), and the combination diagnostic results of the two has good consistency with the histopathological examination results (Kappa value=0.792).. There was no statistically significant difference in the average glandular dose among FFDM [(1.03±0.18)mGy], low-dose DBT [(1.04±0.19) mGy]and combined examination of the two [(1.06±0.21) mGy] (F=1.529, P>0.05), and there was no statistically significant difference between FFDM examination time [(6.25±0.52) min] and low-dose DBT examination time [(6.33±0.57) min] (t=1.626, P>0.05). Conclusions Compared with FFDM, low-dose DBT has higher application value in screening early breast cancer, and it has good consistency with histopathological examination results, which can be used as an important examination method for clinical screening of early breast cancer. -
Key words:
- Breast neoplasms /
- Mammography /
- Early diagnosis
-
表 1 FFDM、低剂量DBT及二者联合与组织病理学检查对早期乳腺癌诊断的结果比较(例)
Table 1. Comparison between full-field digital mammography (FFDM), low-dose digital breast tomosynthesis (DBT), the combination of the two and histopathological examination in the diagnosis of early breast cancer (case)
影像检查 组织病理学检查 合计 阳性(n=192) 阴性(n=54) FFDM 阳性 144 10 154 阴性 48 44 92 低剂量DBT 阳性 167 2 169 阴性 25 52 77 FFDM联合低剂量DBT 阳性 174 3 177 阴性 18 51 69 注:FFDM为全数字化乳腺X射线摄影;DBT为数字乳腺断层融合X射线成像 表 2 FFDM、低剂量DBT及二者联合诊断早期乳腺癌的效能比较
Table 2. Comparison of efficacy among full-field digital mammography (FFDM), low-dose digital breast tomosynthesis (DBT), and the combination of the two in the diagnosis of early breast cancer
影像检查 灵敏度 特异度 准确率 阳性预测值 阴性预测值 FFDM 75.00%(144/192) 81.48%(44/54) 76.42%(188/246) 93.51%(144/154) 47.83%(44/92) 低剂量DBT 86.98%a(167/192) 96.30%a(52/54) 89.02%a(219/246) 98.82%a(167/169) 67.53%a(52/77) FFDM联合低剂量DBT 90.63%b(174/192) 94.44%b(51/54) 91.46%b(225/246) 98.31%b(174/177) 73.91%b(51/69) χ2值 19.289 8.376 26.064 11.110 12.965 P值 <0.001 0.015 <0.001 0.003 0.001 注:FFDM为全数字化乳腺X射线摄影;DBT为数字乳腺断层融合X射线成像;a表示与FFDM比较,差异均有统计学意义(χ2=6.000~13.677,均P<0.05);b表示与FFDM比较,差异均有统计学意义(χ2=4.285~20.644,均P<0.05) -
[1] Chlebowski RT, Anderson GL, Aragaki AK, et al. Association of menopausal hormone therapy with breast cancer incidence and mortality during long-term follow-up of the women's health initiative randomized clinical trials[J]. JAMA, 2020, 324(4): 369−380. DOI: 10.1001/jama.2020.9482. [2] Duffy SW, Vulkan D, Cuckle H, et al. Effect of mammographic screening from age 40 years on breast cancer mortality (UK Age trial): final results of a randomised, controlled trial[J]. Lancet Oncol, 2020, 21(9): 1165−1172. DOI: 10.1016/S1470-2045(20)30398-3. [3] Şendur HN, Cerit MN, Gültekin S, et al. Comparison of mass size measurements: synthesized mammography versus full-field digital mammography[J]. Acad Radiol, 2020, 27(6): 766−773. DOI: 10.1016/j.acra.2019.08.016. [4] Ko MJ, Park DA, Kim SH, et al. Accuracy of digital breast tomosynthesis for detecting breast cancer in the diagnostic setting: a systematic review and meta-analysis[J]. Korean J Radiol, 2021, 22(8): 1240−1252. DOI: 10.3348/kjr.2020.1227. [5] 戴工华, 马承军, 姚杰, 等. 不同附加滤过与管电压和管电流组合对小儿床边X射线摄影图像质量和辐射剂量的影响[J]. 中华放射医学与防护杂志, 2019, 39(1): 31−36. DOI: 10.3760/cma.j.issn.0254-5098.2019.01.007.
Dai GH, Ma CJ, Yao J, et al. Influence of different combinations of additional filters and tube voltage and tube current on crib side X-ray image quality and radiation dose[J]. Chin J Radiol Med Prot, 2019, 39(1): 31−36. DOI: 10.3760/cma.j.issn.0254-5098.2019.01.007.[6] 美国放射学院. 乳腺影像报告与数据系统图谱: 2013版[M]. 王殊, 洪楠, 译. 北京: 北京大学医学出版社, 2016: 13−14.
American College of Radiology. ACR BI-RADS® ATLAS: breast imaging reporting and data system[M]. Wang S, Hong N, trans. Beijing: Peking University Medical Press, 2016: 13−14.[7] 丁贤彬, 吕晓燕, 焦艳, 等. 2012—2020年重庆市女性乳腺癌发病率与死亡率变化趋势分析[J]. 中国肿瘤, 2022, 31(1): 37−42. DOI: 10.11735/j.issn.1004-0242.2022.01.A003.
Ding XB, Lyu XY, Jiao Y, et al. Trends of incidence and mortality of female breast cancer from 2012 to 2020 in Chongqing[J]. China Cancer, 2022, 31(1): 37−42. DOI: 10.11735/j.issn.1004-0242.2022.01.A003.[8] Clèries R, Ameijide A, Buxó M, et al. Excess mortality among breast cancer patients in early stages in Tarragona and Gerona (Spain)[J]. Gac Sanit, 2020, 34(4): 356−362. DOI: 10.1016/j.gaceta.2018.09.008. [9] Mizukoshi MM, Hossian SZ, Poulos A. Comparative analysis of breast cancer incidence rates between Australia and Japan: screening target implications[J]. Asian Pac J Cancer Prev, 2020, 21(7): 2123−2129. DOI: 10.31557/APJCP.2020.21.7.2123. [10] Chikarmane SA, Cochon LR, Khorasani R, et al. Screening mammography performance metrics of 2D digital mammography versus digital breast tomosynthesis in women with a personal history of breast cancer[J]. AJR Am J Roentgenol, 2021, 217(3): 587−594. DOI: 10.2214/AJR.20.23976. [11] Caumo F, Montemezzi S, Romanucci G, et al. Repeat screening outcomes with digital breast tomosynthesis plus synthetic mammography for breast cancer detection: results from the prospective verona pilot study[J]. Radiology, 2021, 298(1): 49−57. DOI: 10.1148/radiol.2020201246. [12] Asbeutah AM, AlMajran AA, Brindhaban A, et al. Comparison of radiation doses between diagnostic full-field digital mammography (FFDM) and digital breast tomosynthesis (DBT): a clinical study[J]. J Med Radiat Sci, 2020, 67(3): 185−192. DOI: 10.1002/jmrs.405. [13] Ban K, Tsunoda H, Togashi S, et al. Breast cancer screening using digital breast tomosynthesis compared to digital mammography alone for Japanese women[J]. Breast Cancer, 2021, 28(2): 459−464. DOI: 10.1007/s12282-020-01180-2. [14] Alabousi M, Zha NX, Salameh JP, et al. Digital breast tomosynthesis for breast cancer detection: a diagnostic test accuracy systematic review and meta-analysis[J]. Eur Radiol, 2020, 30(4): 2058−2071. DOI: 10.1007/s00330-019-06549-2. [15] 周蜀川, 张雪琴, 王紫薇, 等. 探讨数字乳腺三维断层融合与X线摄影在致密型乳腺诊断中的剂量差异及临床运用价值[J]. 中国医疗设备, 2020, 35(4): 75−78. DOI: 10.3969/j.issn.1674-1633.2020.04.020.
Zhou SC, Zhang XQ, Wang ZW, et al. Exploration of the dose difference and clinical application value of digital breast three-dimensional tomographic fusion and X-ray photography in the diagnosis of dense breast[J]. China Med Devices, 2020, 35(4): 75−78. DOI: 10.3969/j.issn.1674-1633.2020.04.020.[16] 谭琬琳, 孙剑宁, 李艳辉. 数字化乳腺X线摄影与三维断层摄影对乳腺癌初诊价值的比较分析[J]. 中国医疗设备, 2020, 35(10): 160−163. DOI: 10.3969/j.issn.1674-1633.2020.10.036.
Tan WL, Sun JN, Li YH. A comparative analysis of full-field digital mammography and digital breast tomosynthesis in the diagnosis of breast cancer[J]. China Med Devices, 2020, 35(10): 160−163. DOI: 10.3969/j.issn.1674-1633.2020.10.036.[17] 梁畅, 张伟, 王慧颖. 数字乳腺X线与断层摄影对乳腺“结构扭曲”样病变的诊断效能分析[J]. 中国临床医学影像杂志, 2020, 31(11): 797−800, 808. DOI: 10.12117/jccmi.2020.11.009.
Liang C, Zhang W, Wang HY. The assessment of diagnostic efficacy in breast architectural distortion on mammography vs digital breast tomosynthesis[J]. J China Clin Med Imaging, 2020, 31(11): 797−800, 808. DOI: 10.12117/jccmi.2020.11.009. -





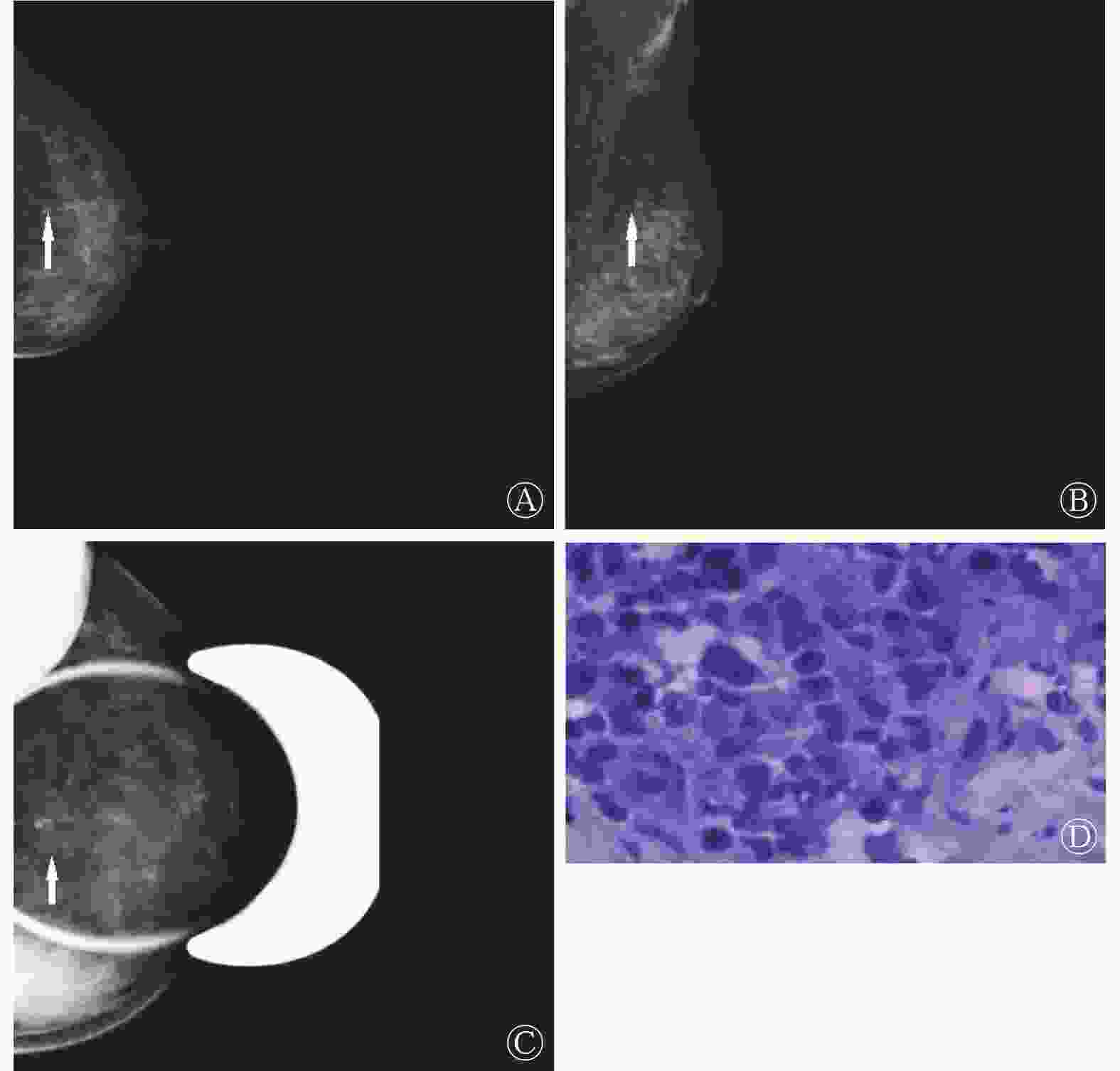
 下载:
下载: