-
特发性嗜酸性粒细胞增多症是一种原因不明,以外周血同骨髓中嗜酸性粒细胞持续增多和组织中嗜酸性粒细胞浸润为特征的疾病[1]。当该病出现肝脏浸润时,在影像学诊断方面,常与肝脏其他良恶性肿瘤相混淆,容易误诊。笔者报道了1例特发性嗜酸性粒细胞增多症肝脏浸润18F-FDG PET/CT显像的病例。
-
患者男性,50岁,因“低热3个月余,发现嗜酸性粒细胞增多1 d”于2022年5月8日就诊于大连医科大学附属第二医院。患者3个月前无明显诱因出现低热,体温最高37.5℃,伴轻度畏寒、背部肌肉酸痛,无咳嗽咳痰,无头晕头痛,发热时间多在夜间,每4~5 d发热1次,物理降温及服用莲花清瘟胶囊后体温可逐渐降至正常。
入院检查血常规,结果显示:外周血嗜酸性粒细胞百分比为46.50%(正常参考值为0.40%~8.00 %);外周血嗜酸性粒细胞绝对值为7.04×109/L(正常参考值为0.02×109~0.52×109/L);C反应蛋白为13.44 mg/L(正常参考值为0~10 mg/L);WBC计数为15.13×109/L(正常参考值为3.50×109~9.50×109/L);淋巴细胞绝对值为3.99×109/L(正常参考值为1.10×109~3.20×109/L);中性粒细胞绝对值为3.57×109/L(正常参考值为1.80×109~6.30×109/L)。
肝功能生化检查结果显示:总蛋白为 59.93 g/L(正常参考值为65.00~85.00 g/L);白蛋白为38.54 g/L(正常参考值为40.00~55.00 g/L);γ-谷氨酰基转移酶为129.67 U/L(正常参考值为10.00~60.00 U/L);碱性磷酸酶为188 U/L(正常参考值为45~125 U/L)。患者既往无肝脏病变,无乙肝病史,无疫区旅居史及否认近期进食生鲜类食物。
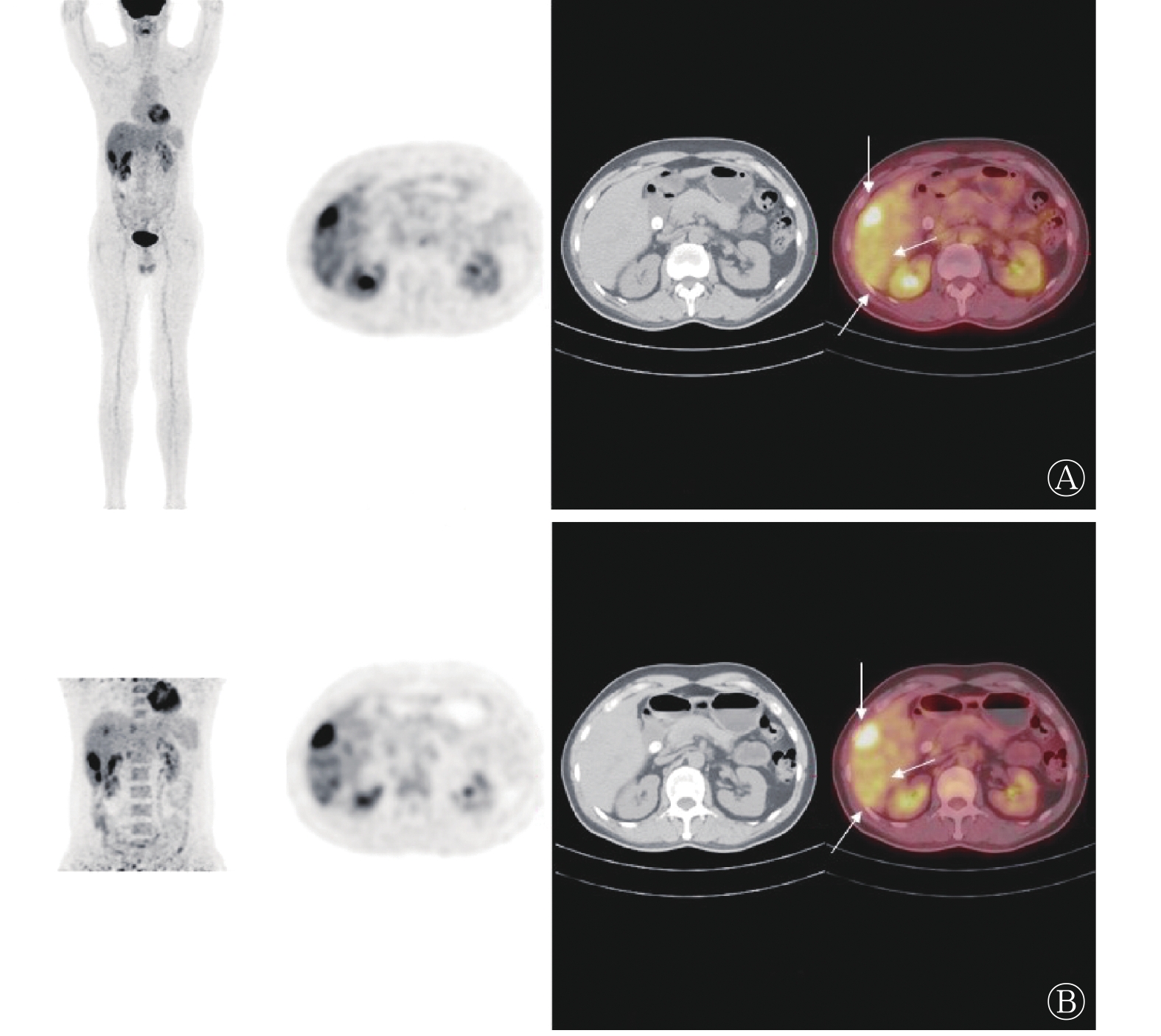
患者于2022年5月9日行骨髓穿刺术,骨髓细胞学检查结果显示:骨髓及外周血嗜酸性粒细胞增多,占比分别为28%和38%。患者于2022年5月12日行18F-FDG PET/CT,结果显示,肝脏内有多发稍低密度灶,伴结节状高代谢(图1),其中早期显像发现14个病灶,SUVmax为3.1~6.7;延迟1 h显像发现18个病灶, SUVmax为3.5~8.4,结合病史,考虑可能为嗜酸性粒细胞增多症肝脏浸润,建议行增强MRI及组织病理学检查。2022年5月17日患者行增强MRI,结果显示:肝脏有多发异常信号,结合病史,考虑可能为嗜酸性粒细胞增多症肝脏浸润(图2)。患者于2022年5月20日行增强CT,结果显示:肝脏有多发低密度影,结合病史,考虑可能为嗜酸性粒细胞增多症肝脏浸润(图3)。患者于2022年5月20日行CT介入引导下肝脏穿刺,组织病理学结果显示:肝板及小叶结构正常,肝细胞未见异型,汇管区及肝板间见多量嗜酸性粒细胞浸润(>30个/高倍视野)(图4)。其他检查结果:肿瘤标志物(−)、布鲁氏菌免疫球蛋白G抗体(−)、疟原虫检查(−)、骨髓增生异常综合征免疫分型(−)、血培养细菌及厌氧菌(−)。综合上述检查结果,患者被确诊为特发性嗜酸性粒细胞增多症肝脏浸润,口服泼尼松治疗,30 mg/次,2次/d。

图 1 特发性嗜酸性粒细胞增多症肝脏浸润患者(男性,50岁)的18F-FDG PET/CT图
Figure 1. 18F-FDG PET/CT images of liver in a patient (male, 50 years old) with idiopathic eosinophilia hepatic infiltration

图 2 特发性嗜酸性粒细胞增多症肝脏浸润患者(男性,50岁)的增强磁共振显像图
Figure 2. MRI images of liver in a patient (male, 50 years old) with idiopathic eosinophilia hepatic infiltration

图 3 特发性嗜酸性粒细胞增多症肝脏浸润患者(男性,50岁)的增强CT图
Figure 3. CT images of liver in a patient (male, 50 years old) with idiopathic eosinophilia hepatic infiltration

图 4 特发性嗜酸性粒细胞增多症肝脏浸润患者(男性,50岁)的组织病理学检查图(苏木精-伊红染色,×40)
Figure 4. Histopathological examination (hematoxylin eosin staining, ×40) image of liver in a patient (male, 50 years old) with idiopathic eosinophilia hepatic infiltration
2022年6月1日复查血常规,结果显示:外周血嗜酸性粒细胞百分比为3.50%;外周血嗜酸性粒细胞绝对值为0.32×109/L;C反应蛋白水平为0.75 mg/L;WBC计数为9.14×109/L;淋巴细胞绝对值为2.81×109/L;中性粒细胞绝对值为5.24×109/L。2022年7月12日复查腹部增强MRI,结果显示:病灶较治疗前明显缩小(图5)。
-
嗜酸性粒细胞增多症是以外周血和骨髓中嗜酸性粒细胞持续增多、组织中嗜酸性粒细胞浸润为特征的一组罕见疾病[1]。嗜酸性粒细胞增多症的分类包括继发性(反应性)、遗传性(家族性)、原发性(克隆性)和特发性4大类[2]。发病原因主要包括寄生虫感染、过敏性疾病、遗传、血液系统肿瘤克隆等。特发性嗜酸性粒细胞增多症为未发现导致嗜酸性粒细胞增多的潜在原因,非反应性、非家族性、非肿瘤性的意义未定的嗜酸性粒细胞增多症,是一种排除诊断结果,本例患者即为特发性嗜酸性粒细胞增多症。
嗜酸性粒细胞增多症的发病机制复杂,异质性较强,临床表现多样,轻者可无症状或仅表现为发热、咳嗽,重者可累及多个器官系统,导致被浸润器官的病理改变甚至不可逆的器官损害[3]。损害可由单纯的嗜酸性粒细胞浸润、嗜酸性粒细胞诱导的纤维化、过敏机制或嗜酸性粒细胞促进高凝状态引起,可累及皮肤、呼吸道、心脏、消化道、眼、神经系统和血液系统[4],表现为:(1)肺、心脏、消化道、皮肤等的纤维化[5];(2)血栓形成[6];(3)皮肤受累,多为红斑、水肿、溃疡、瘙痒和丘疹[7-8];(4)反复的神经功能障碍[9]等。嗜酸性粒细胞肝脏浸润是一种以嗜酸性粒细胞持续过量增殖为特征,局部肝组织浸润所致的肝脏病变临床少见,其发生率仅为0.41%~0.68%,且多数患者无特异性症状[10-11],少数可表现为肝脏体积增大、上腹痛、腹泻、肝功能异常、肝脓肿及重型肝炎。
嗜酸性粒细胞增多症肝脏浸润的影像学表现为多发性、结节性浸润,单发浸润少见。郭保亮等[12]研究发现,肝内病灶数与外周血嗜酸性粒细胞计数呈正相关,病灶主要分布于肝包膜下及门静脉周围肝实质;门静脉周围病灶多呈圆形或类圆形,肝包膜下的病灶则以楔形为主[13],这种分布情况与本例患者一致。CT平扫可表现为稍低或等密度影,动脉期未见明显变化,门脉期可见明显低密度,延迟期恢复稍低或等密度,表现为“等-低-等”的强化方式。在MRI T1WI及增强扫描时,其影像学特征类似于增强CT的表现,在T2WI上表现为高信号[14],这种密度(信号)表现和强化方式与本例患者一致。另外,“门静脉穿行征”即病灶内有门静脉分支穿行,走行自然,无门静脉受压推移的占位征象,这对本病的诊断有重要价值。
18F-FDG是目前临床最常用的PET/CT显像剂,能反映病灶的葡萄糖代谢情况,在肝脏疾病的辅助诊断上具有重要意义,且能早期发现病灶[15],本例患者的肝脏病灶即为18F-FDG PET/CT最早发现。既往的一项研究结果表明,嗜酸性粒细胞增多症肝脏浸润所形成的结节可摄取18F-FDG,但该研究14例患者的21个病灶中,仅4个病灶摄取18F-FDG,其平均SUV为4.0,且高摄取18F-FDG的结节长径明显大于未摄取的结节(26.5 mm对11.8 mm),摄取18F-FDG的结节的SUVmax为2.0~7.4;同时,研究者还发现,摄取18F-FDG组的病灶与邻近正常肝实质在门脉期CT上的平均密度差明显大于未摄取18F-FDG组。在T2WI上,摄取18F-FDG的病灶的平均信号强度差也明显大于不摄取18F-FDG的病灶,其潜在机制可能为病灶中嗜酸性粒细胞大量聚集,白细胞的活化与招募及其葡萄糖转运蛋白表达增加[16]。另外一项单纯性肺嗜酸性粒细胞增多症的研究结果显示,在14例患者的42个病灶中,有12个病灶摄取18F-FDG,其SUVmax为0.6~5.3,实性结节摄取18F-FDG的比例明显大于磨玻璃密度结节,因此认为这可能与结节中炎性细胞的密度相关[17]。本研究中,患者早期显像发现的14个肝脏病灶的SUVmax为3.1~6.7,延迟1 h显像后发现了18个肝脏病灶,且所有肝脏病灶的18F-FDG摄取均较早期显像明显升高,SUVmax为3.5~8.4,这提示延迟显像在嗜酸性粒细胞增多症肝脏病灶18F-FDG PET/CT显像中的重要性。此外,嗜酸性粒细胞增多症可导致多系统、多器官的病变[18],18F-FDG PET/CT作为全身检查方法相对于其他影像学检查方法可以发现更多器官的受累情况。
嗜酸性粒细胞增多症肝脏浸润在诊断时应与肝脏其他良恶性疾病相鉴别,包括:(1)肝细胞肝癌,可伴随乙肝病史,增强后呈典型“快进快出”的强化方式,肿瘤标志物甲胎蛋白常升高,18F-FDG摄取因肿瘤分化程度而不同;(2)胆管细胞癌,增强扫描具有“延迟强化”的影像学特征,可伴随胆管扩张,肿瘤标志物CA199水平常升高,18F-FDG可轻度摄取,也可表现为高摄取;(3)肝脓肿,临床表现多有高热、寒战伴白细胞增高,增强扫描可表现为环形强化方式,MRI扩散加权成像序列可见脓肿中央高信号,18F-FDG PET/CT显像可呈高摄取;(4)肝淋巴瘤,可伴肝脏体积增大及其他淋巴结或结外组织受累;(5)肝转移瘤,有明确的原发肿瘤病史,可见典型的“牛眼征”。
综上所述,嗜酸性粒细胞增多症肝脏浸润临床少见,且多无特异性症状及体征,易漏诊及误诊。临床上可根据其CT、MRI平扫及强化的影像学特征辅助鉴别诊断,18F-FDG PET/CT可提供病灶的代谢信息及全身分布情况,其优势在于早期发现,全身显像以及延迟显像可发现隐匿病灶,缺点在于部分病灶低摄取或无摄取18F-FDG。
利益冲突 所有作者声明无利益冲突
作者贡献声明 林润龙负责病例的采集、数据的获取、论文的撰写;于璟负责研究命题的设计;袁欣负责临床资料的随访;王晓梅负责影像图像的分析;田爱娟负责研究命题的设计与论文的修改
特发性嗜酸性粒细胞增多症肝脏浸润18F-FDG PET/CT显像1例
Idiopathic eosinophilia hepatic infiltration revealed by 18F-FDG PET/CT imaging: a case report
-
摘要: 笔者报道了1例特发性嗜酸性粒细胞增多症肝脏浸润18F-氟脱氧葡萄糖(FDG)PET/CT显像病例。18F-FDG PET/CT显像不仅能更早地发现肝脏病灶,提供其糖代谢信息,还能评估全身多器官受累分布情况。笔者拟通过对该病例进行分析并对相关文献进行复习,以加深对特发性嗜酸性粒细胞增多症肝脏浸润影像学特征的认识。Abstract: The authors reported a case of idiopathic eosinophilia hepatic infiltration by 18F-fluorodeoxyglucose (FDG) PET/CT. 18F-FDG PET/CT imaging can not only detect hepatic lesions earlier and provide information on glucose metabolism, but also evaluate the distribution of multiple organ involved in the whole body. The authors intend to analyze the case and review the relevant literature in order to deepen the understanding of the imaging characteristics of hepatic infiltration in idiopathic eosinophilia.
-
Key words:
-
-
[1] 王健民, 龚胜蓝. 原发性嗜酸粒细胞增多症的诊断与治疗[J]. 临床血液学杂志, 2021, 34(11): 753−757. DOI: 10.13201/j.issn.1004-2806.2021.11.001.
Wang JM, Gong SL. Diagnosis and treatment of primary hypereosinophilia[J]. J Clin Hematol, 2021, 34(11): 753−757. DOI: 10.13201/j.issn.1004-2806.2021.11.001.[2] 中华医学会血液学分会白血病淋巴瘤学组. 嗜酸粒细胞增多症诊断与治疗中国专家共识(2017年版)[J]. 中华血液学杂志, 2017, 38(7): 561−565. DOI: 10.3760/cma.j.issn.0253-2727.2017.07.001.
Leukemia and Lymphoma Group, Chinese Society of Hematology, Chinese Medical Association. Chinese expert consensus on the diagnosis and treatment of eosinophilia (2017)[J]. Chin J Hematol, 2017, 38(7): 561−565. DOI: 10.3760/cma.j.issn.0253-2727.2017.07.001.[3] 王子熹. 嗜酸性粒细胞增多综合征的诊断与治疗[J]. 中华临床免疫和变态反应杂志, 2021, 15(1): 108−109. DOI: 10.3969/j.issn.1673-8705.2021.01.024.
Wang ZX. Diagnosis and treatment of eosinophil syndrome[J]. Chin J Allergy Clin Immunol, 2021, 15(1): 108−109. DOI: 10.3969/j.issn.1673-8705.2021.01.024.[4] 戴新羽, 段立伟, 张凯, 等. 特发性嗜酸性粒细胞增多症1例报道[J]. 胃肠病学和肝病学杂志, 2020, 29(6): 714−715. DOI: 10.3969/j.issn.1006-5709.2020.06.023.
Dai XY, Duan LW, Zhang K, et al. Idiopathic hypergranulocytosis: one case report[J]. Chin J Gastroenterol Hepatol, 2020, 29(6): 714−715. DOI: 10.3969/j.issn.1006-5709.2020.06.023.[5] 李菁, 李嵘娟, 张烨, 等. 嗜酸性粒细胞增多症累及心脏的临床表现及超声心动图特征[J]. 心肺血管病杂志, 2022, 41(4): 399−403. DOI: 10.3969/j.issn.1007-5062.2022.04.014.
Li J, Li RJ, Zhang Y, et al. Clinical manifestation and echocardiographic features of hypereosinophilic syndrome involving the heart[J]. J Cardiovasc Pulm Dis, 2022, 41(4): 399−403. DOI: 10.3969/j.issn.1007-5062.2022.04.014.[6] 高汉林, 卢宇轩, 黄一宁, 等. 高嗜酸性粒细胞增多症与缺血性卒中关系的研究进展[J]. 中华神经科杂志, 2022, 55(7): 770−774. DOI: 10.3760/cma.j.cn113694-20211219-00901.
Gao HL, Lu YX, Huang YN, et al. Research progress on the relationship between hypereosinophilia and ischemic stroke[J]. Chin J Neurol, 2022, 55(7): 770−774. DOI: 10.3760/cma.j.cn113694-20211219-00901.[7] 蒋小妹, 黄龙, 张声, 等. 特发性高嗜酸性粒细胞综合征[J]. 临床皮肤科杂志, 2022, 51(8): 473−476. DOI: 10.16761/j.cnki.1000-4963.2022.08.009.
Jiang XM, Huang L, Zhang S, et al. A case of idiopathic hypereosinophilia syndrome[J]. J Clin Dermatol, 2022, 51(8): 473−476. DOI: 10.16761/j.cnki.1000-4963.2022.08.009.[8] 丁英洁, 李上云, 赵宁, 等. 嗜酸性粒细胞增多性环状红斑一例[J]. 中华皮肤科杂志, 2021, 54(10): 906−907. DOI: 10.35541/cjd.20191173.
Ding YJ, Li SY, Zhao N, et al. A case of eosinophilic annular erythema[J]. Chin J Dermatol, 2021, 54(10): 906−907. DOI: 10.35541/cjd.20191173.[9] 梁玉梅, 连丽丽, 聂冠华, 等. 伴有继发性嗜酸性粒细胞增多的多发性周围神经病1例报告[J]. 中风与神经疾病杂志, 2021, 38(4): 360−361. DOI: 10.19845/j.cnki.zfysjjbzz.2021.0094.
Liang YM, Lian LL, Nie GH, et al. Multiple peripheral neuropathy with secondary eosinophil: a case report[J]. J Apoplexy Nerv Dis, 2021, 38(4): 360−361. DOI: 10.19845/j.cnki.zfysjjbzz.2021.0094.[10] Kwon JW, Kim TW, Kim KM, et al. Clinical features of clinically diagnosed eosinophilic liver abscesses[J]. Hepatol Int, 2011, 5(4): 949−954. DOI: 10.1007/s12072-011-9272-0. [11] Sim DW, Son DJ, Cho E, et al. What are the clinical features and etiology of eosinophilic liver infiltration?[J]. Gut Liver, 2019, 13(2): 183−190. DOI: 10.5009/gnl18266. [12] 郭保亮, 欧阳富盛, 张斌, 等. 肝脏嗜酸性粒细胞浸润的CT和MRI征象分析[J]. 中华放射学杂志, 2017, 51(2): 132−135. DOI: 10.3760/cma.j.issn.1005-1201.2017.02.011.
Guo BL, Ouyang FS, Zhang B, et al. Analysis of CT and MRI signs of hepatic eosinophilic infiltration[J]. Chin J Radiol, 2017, 51(2): 132−135. DOI: 10.3760/cma.j.issn.1005-1201.2017.02.011.[13] Guo BL, Hu QG, Ouyang FS, et al. CT and MRI findings in focal eosinophilic infiltration of the liver[J]. Abdom Radiol, 2017, 42(12): 2874−2881. DOI: 10.1007/s00261-017-1230-4. [14] Claeys W, Delie A, Smeets P, et al. Focal eosinophilic infiltration of the liver, benign or malignant?[J/OL]. Clin Case Rep, 2021, 9(8): e04448[2022-09-11]. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8365548/. DOI: 10.1002/ccr3.4448. [15] 王锦, 林润龙. 肝肺吸虫病18F-FDG PET/CT显像一例[J]. 国际放射医学核医学杂志, 2022, 46(3): 193−196. DOI: 10.3760/cma.j.cn121381-202012043-00143.
Wang J, Lin RL. Hepatic paragonimiasis revealed by 18F-FDG PET/CT: a case report[J]. Int J Radiat Med Nucl Med, 2022, 46(3): 193−196. DOI: 10.3760/cma.j.cn121381-202012043-00143.[16] Kim WH, Kim SH, Kim YH, et al. Fluorine-18-FDG PET findings of focal eosinophilic liver disease: correlation with CT and/or MRI, laboratory, and pathologic findings[J]. Abdom Imaging, 2010, 35(4): 437−446. DOI: 10.1007/s00261-009-9513-z. [17] Kim TJ, Lee KW, Kim HY, et al. Simple pulmonary eosinophilia evaluated by means of FDG PET: the findings of 14 cases[J]. Korean J Radiol, 2005, 6(4): 208−213. DOI: 10.3348/kjr.2005.6.4.208. [18] 苑喜微, 董士铭, 赵素贤, 等. 以多器官损害为主要临床表现的嗜酸粒细胞增多症1例[J]. 中华肝脏病杂志, 2019, 27(5): 391−392. DOI: 10.3760/cma.j.issn.1007-3418.2019.05.014.
Yuan XW, Dong SM, Zhao SX, et al. A case with multiple organ damage mainly clinically manifested through eosinophilia[J]. Chin J Hepatol, 2019, 27(5): 391−392. DOI: 10.3760/cma.j.issn.1007-3418.2019.05.014. -





 下载:
下载: