-
放疗是乳腺癌治疗的重要组成部分,可降低乳腺癌保乳术后患者的局部复发率和病死率[1-2]。迄今为止,随着放疗技术的进步,三维适形放疗、旋转容积调强放疗及调强适形放疗(intensity modulated radiation therapy,IMRT)成为放疗技术的主流,IMRT在乳腺癌放疗过程中的使用显著增多,在很大程度上改善和提高了放疗的质量,可降低其对心脏、肺等重要脏器的辐射剂量,实现了对肿瘤的精准放疗[3]。但IMRT对摆位的精确度要求较高,系统摆位误差的微小变化,可导致靶区剂量分布的不均匀性增大,因此,摆位误差可能会导致放疗剂量超过危及器官的耐受量[4]。乳腺的形状特殊,活动度大,呼吸运动、手臂上举情况和治疗次数的增加等因素均可影响摆位误差,还可能导致靶点错位[5-7],造成部分靶区剂量不足,降低肿瘤的局部控制率,从而导致严重的并发症或后遗症[8]。模拟定位是保证治疗体位准确和可重复的重要环节[4],因此需要特定的定位方式以提高肿瘤定位的准确性。研究人员已经证明乳腺癌保乳术后采用基于体膜联合开窗定位方式的大分割放疗方案具有一定的可行性,可明显减轻急性放射性皮肤反应,同时并未增加明显的放疗不良反应[9]。本研究通过进一步比较乳腺癌患者保乳术后采用乳腺托架定位与热塑体膜双重标记联合开窗技术定位的放疗摆位误差及放射性皮肤反应,以期选出更好的定位方式,提高摆位精确度。
-
回顾性分析2019年1月至2020年12月郑州大学第五附属医院收治的83例乳腺癌保乳术后的女性患者(0~Ⅲ期)的临床资料,年龄(47.5±10.1)岁,范围31~70岁,其中左乳腺癌患者53例、右乳腺癌患者30例。患者术后TNM分期:Ⅰ期36例、Ⅱ期39例、Ⅲ期8例。根据定位方式将患者分为体膜组(42例)和乳腺托架组(41例)。
患者纳入标准:均为女性;单侧乳腺癌保乳术后,经组织病理学检查结果确诊为乳腺癌;意识清楚,上肢功能良好,摆位配合度好。排除标准:无放疗指征;不能配合CT扫描或治疗。所有患者均于治疗前签署了知情同意书。本研究经郑州大学第五附属医院伦理委员会批准(批准号:KY2021011)。
-
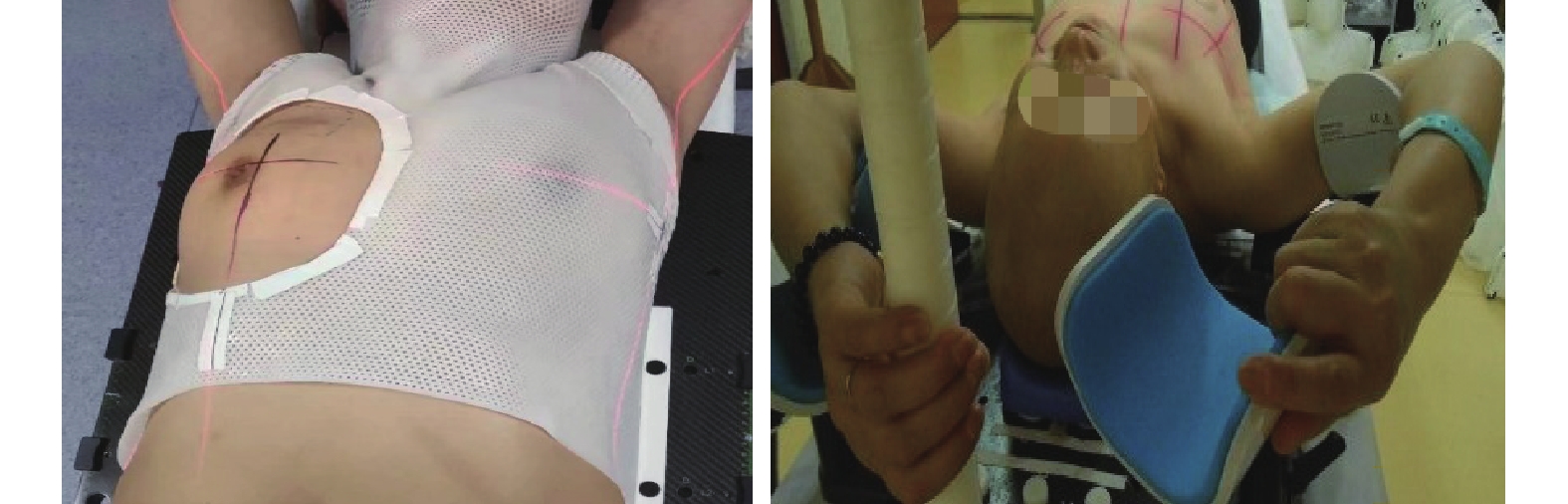
体膜组:患者取仰卧位,选用合适的标准化头枕,双手交叉抱肘置于前额,嘱患者制动,用记号笔在体表标记出患侧乳腺及手术瘢痕。将加热的热塑体膜从恒温水箱中取出,均匀覆盖在患者体表并固定在多功能体架上,待体膜冷却成型后,在体膜上勾画出乳腺的范围,取下体膜修剪后,再次将体膜扣上,使患侧乳腺充分暴露。采用铅丝标记乳腺轮廓及手术瘢痕。选取摆位中心,一般为锁骨中线、腋前线和乳头层交汇处,利用激光在体表上标注出“+”字的中心点,将乳头层与锁骨中线汇合处的“+”直接画在皮肤表面,使体表与体膜上的“+”处于同一平面(图1A)。

图 1 乳腺癌放疗患者的热塑体膜双重标记联合开窗技术定位(A)和乳腺托架(B )定位
Figure 1. Thermoplastic membrane double labeling combined with fenestration technology (A) and breast-bracket (B) positioning for breast cancer patients undergoing radiotherapy
乳腺托架组:将乳腺托架放置在定位床上,调整至合适位置后,患者取仰卧位,调整乳腺托架上各种体位限度辅助装置,包括上臂外展和托举角度、躯体底板倾斜角度,利用激光辅助摆位,在患者两侧腋前线激光水平位置和体中线(胸骨切迹至剑突) 用皮肤墨水画线,作摆位标记,然后用皮肤墨水在皮肤上画出三维激光定位标记线(图1B)。
-
所有患者在瑞典医科达Synergy旋转容积调强放疗直线加速器上行IMRT,全乳的放疗总剂量为50 Gy,分25次完成,同步行瘤床X线加量,瘤床单次剂量为2.3 Gy、总剂量为57.5 Gy。淋巴结转移≥4个应给予区域淋巴结引流区放疗。所有患者均采用锥形束CT(cone-beam CT,CBCT)图像与模拟CT图像配准,配比时选择CBCT图像上1个明显且固定性较好的骨性影像标志为配比参考点,应用计算机配比软件测量骨性标志与照射野各边界之间的距离,配准方式采用自动配准+手动配准,使之完全与治疗计划靶区相重合后完成精确摆位并进行治疗。配准符合要求后,系统自动计算出左右(X轴)、头脚(Y轴)、腹背(Z轴)方向的系统摆位误差。当垂直及水平方向摆位误差≤5 mm时开始治疗。如果摆位误差>5 mm则由主管医师在模拟机下重新核对。开始治疗后每周行1次 CBCT 扫描,收集相关数据以备分析。
-
根据美国肿瘤放射治疗协作组(RTOG)制定的标准[10]评估入组患者的急性和晚期放射性皮肤反应,反应均分为0~4级。其中,急性放射性皮肤反应的0级为无变化;1级为滤泡样暗红色斑、脱发、干性脱皮、出汗减少;2级为触痛性或鲜色红斑、片装湿性脱皮、中度水肿;3级为皮肤皱折以外部位的融合的湿性脱皮、凹陷性水肿;4级为溃疡、出血、坏死。晚期放射性皮肤反应的0级为无变化;1级为轻微的萎缩、色素沉着、些许脱发;2级为片装萎缩、中度毛细血管扩张、全部头发脱落;3级为显著的萎缩、显著的毛细管扩张;4级为溃疡。
-
采用SPSS 22.0软件对数据进行统计学分析,符合正态分布的计量资料以
$\bar x \pm s$ 表示,摆位误差的组间比较采用t检验(方差齐);计数资料以频次和百分比表示,组间比较采用χ2检验。P<0.05为差异有统计学意义。 -
所有患者均按计划完成放疗及摆位验证。83例患者共进行415次CBCT验证,其中体膜组210次,乳腺托架组205次。
-
由表1可知,体膜组在左右(X轴)、头脚(Y轴)、腹背(Z轴)方向的摆位误差均明显小于乳腺托架组,且差异均有统计学意义(t=2.98、2.63、2.49,均P<0.05)。
组别 X轴 Y轴 Z轴 体膜组(n=42) 2.14±0.19 2.49±0.15 2.41±0.22 乳腺托架组(n=41) 2.96±0.20 3.05±0.16 3.14±0.19 t值 2.98 2.63 2.49 P值 <0.05 0.01 0.02 注:体膜组采用热塑体膜双重标记联合开窗技术定位;乳腺托架组采用乳腺托架定位 表 1 2组乳腺癌患者放疗定位的摆位误差比较(
$\bar x\pm s $ Table 1. Comparison of the positioning error of radiotherapy positioning in two groups of breast cancer patients (
$\bar x\pm s $ -
由表2可知,当摆位误差≤3 mm时,在X、Z轴方向上,2组的摆位误差分布比例相近,且差异均无统计学意义(χ2=2.28、3.33,P=0.13、0.07);在Y轴方向上,体膜组的摆位误差分布比例高于乳腺托架组,差异有统计学意义(χ2=7.23,P=0.01);体膜组在摆位误差≤3 mm中的分布比例更高,故体膜组的摆位误差优于乳腺托架组。摆位误差>5 mm时,在X、Y、Z轴方向上,体膜组的摆位误差分布比例均低于乳腺托架组,且差异有统计学意义(均P<0.05)。当摆位误差在3~5 mm时,2组在各方向的摆位误差分布比例差异均无统计学意义(均P>0.05)。
组别 X轴(mm) Y轴(mm) Z轴(mm) ≤3 3~5 >5 ≤3 3~5 >5 ≤3 3~5 >5 体膜组(n=42) 165(78.57) 37(17.62) 8(3.81) 130(72.20) 42(19.02) 38(8.78) 145(69.05) 42(20.00) 23(10.95) 乳腺托架组(n=41) 148(72.20) 39(19.02) 18(8.78) 100(48.78) 37(18.05) 68(33.17) 124(60.49) 30(14.63) 51(24.88) χ2值 2.28 0.14 4.37 7.23 0.26 12.40 3.33 2.28 13.73 P值 0.13 0.71 0.04 0.01 0.61 <0.05 0.07 0.13 <0.05 注:体膜组采用热塑体膜双重标记联合开窗技术定位;乳腺托架组采用乳腺托架定位 表 2 2组乳腺癌放疗患者在不同方向和区间的摆位误差分布比例比较[次(%)]
Table 2. Comparison of the proportion of setup error distribution in different directions and intervals between two groups of breast cancer patients undergoing radiotherapy [times (%)]
-
所有患者均未发生3~4级放射性皮肤反应。2组患者急性放射性皮肤反应发生率的差异有统计学意义(χ2=4.39,P=0.04);2组患者的晚期放射性皮肤反应发生率的差异无统计学意义(χ2=0.24,P=0.63)(表3)。
组别 急性放射性皮肤反应 晚期放射性皮肤反应 0级 1级 2级 总发生率(%) 0级 1级 2级 总发生率(%) 体膜组(n=42) 29 11 2 30.95 40 2 0 4.76 乳腺托架组(n=41) 19 18 4 53.66 38 3 0 7.32 χ2值 4.39 0.24 P值 0.04 0.63 注:体膜组采用热塑体膜双重标记联合开窗技术定位;乳腺托架组采用乳腺托架定位 表 3 2组乳腺癌患者放疗后的皮肤不良反应比较(例)
Table 3. Comparison of skin adverse reactions after radiotherapy in two groups of breast cancer patients (cases)
-
精准放疗是在常规放疗基础上通过精确的肿瘤定位、计划设计、剂量计算及在治疗机上精确执行的一种全新的肿瘤放疗计划,在精准放疗的全过程中,每一步都强调精度,这对常规放疗来说是质的飞跃;其根本目的在于给肿瘤区域足够的治疗剂量,且减少周围正常组织和器官的受照剂量[11]。IMRT是一种新型的适形放射疗法,可以达到最佳剂量分布,并且可以显著改善临床效果,Chau等[12]指出,保乳术后患者进行IMRT具有可行性,并能提供良好的美容效果。国际辐射单位与测量委员会(ICRU)81号报告[13]中指出,IMRT的目标复杂,采用体膜定位时需个体化验证,因为靶区剂量偏离5%就可能使原发灶失控或并发症增加。由于乳腺器官的特殊性,极易造成摆位误差,使靶区内剂量分布不均匀,甚至靶点脱位,继而产生严重的放疗不良反应。因此,在乳腺癌保乳术后精准放疗的实施过程中,体位固定已成为保障分次治疗期间体位重复性和准确性的重要环节[4]。
国内外许多专家学者对乳腺癌保乳术后放疗的体位固定、摆位误差进行了大量的研究[14-15],采用各种各样的体位固定技术降低摆位误差。在乳腺癌放疗体位定位中,乳腺托架的应用较多,其能使身体舒适,通过调整胸壁与床面的水平提高放疗的精度。但李俊禹等[16]研究发现,乳腺癌患者单纯使用乳腺托架摆位误差仍然较大。为确保乳腺癌IMRT顺利开展,多治疗中心[17-18]采用个体化楔形真空垫、湿固化树脂垫、热塑体膜联合固定法对乳腺癌患者进行体位固定,研究乳腺癌保乳术后放疗的摆位误差,其中,谢涛等[19]比较多功能体板联合头部热塑体膜定位与乳腺托架定位方式的摆位误差,得出2组放疗前的误差数据,结果表明,乳腺癌放疗特别是胸壁野结合锁骨上野照射时,多功能体板结合头部热塑体膜固定方式可产生更小的摆位误差和分次内误差。
热塑体膜体位固定技术极大地改善了乳腺癌患者保乳术后IMRT的准确性和重复性,但是在临床工作中,研究者发现该技术具有收缩和二次回缩的特性,同时由于热塑体膜不可避免对乳房造成挤压,影响靶区剂量分布,且乳房放疗的摆位重复性差[6]。本研究在采用多功能体板联合颈胸部体膜的基础上加以改进,即采用热塑体膜双重标记联合开窗技术定位,结果显示,采用此定位方式时,摆位的稳定性及重复性更具有优势;本研究中2组患者急性放射性皮肤反应差异有统计学意义,其主要原因有以下几个方面。单纯采用乳腺托架进行体位固定时:(1)乳腺托架有一定的倾斜,治疗中患者容易往下滑或因治疗时间较长难以保持固定体位而使靶区移位;(2)对于部分乳腺松弛患者,使用乳腺托架时,乳腺活动度大,每次治疗时很难保持乳腺靶区的准确性;(3)使用乳腺托架在IMRT机架等中心旋转时,机头极易与托架或治疗床碰撞造成事故。采用热塑体膜双重标记联合开窗技术定位时:(1)热塑体膜具有较强的可塑性、韧性,不易被折断、破损,更可靠、更安全且操作简捷[20];(2)本研究采用头颈肩热塑体膜固定,患者仰卧在水平的多功能体架上,首先排除了重力作用的影响,同时体膜可以限制呼吸运动、身体下意识挪动,可将摆位控制在最小的范围内;(3)体膜开窗法修剪了体膜,充分暴露患侧乳房,开窗周边可维持乳房形状,将乳头层与锁骨中线汇合处的“+”直接画在皮肤表面,使体表与体膜上的“+”处于同一平面,在摆位时通过激光“+”对准皮肤“+”和激光线对准体膜标记线的双重调整摆位法,使体表平面与体膜上3个点所在平面重合,减少了体表与体膜间的相对位移,使得摆位误差变小,重复性更好,且避免了皮肤褶皱,同时窗口区域乳腺皮肤不再有体膜覆盖,减少了摩擦,同时减少了体膜对皮肤的剂量贡献,这些都可能提高乳腺放疗剂量的准确性,降低皮肤的受照剂量,有助于减少放疗的皮肤不良反应。
乳腺癌放疗是长时间、多次治疗的过程,合适的体位固定装置可以保证分次放疗的体位稳定性和重复性。热塑体膜双重标记联合开窗技术定位是利用双重摆位标记线且充分暴露患侧乳房,比单纯采用乳腺托架定位明显减小了摆位误差并减少了急性放射性皮肤反应,提高了重复性放疗摆位的精确度,且该方法简单易操作,有推广应用潜力。目前,用于乳腺癌手术后IMRT的体位定位器,各放疗中心因条件不同有一定差异,如何更好地使用这些设备来保证乳腺癌放疗的质量需要在未来进行进一步总结和研究。
利益冲突 所有作者声明无利益冲突
作者贡献声明 黄平平负责研究命题的设计、研究过程的实施、论文的撰写与最终版本的修订;李敏杰负责命题的提出、论文的审阅;田玉龙、宋俊华、翟永飞负责数据的收集与分析
热塑体膜双重标记联合开窗技术定位在乳腺癌保乳术后放疗中的应用价值
Application value of thermoplastic membrane double labeling combined with fenestration technology in post-breast conserving radiotherapy for breast cancer
-
摘要:
目的 比较乳腺癌患者保乳术后采用乳腺托架定位与基于热塑体膜双重标记联合开窗技术定位方式的放疗摆位误差及放射性皮肤反应,对热塑体膜双重标记联合开窗技术定位方法的可行性进行研究。 方法 回顾性分析2019年1月至2020年12月郑州大学第五附属医院收治的83例乳腺癌保乳术后女性患者的临床资料,年龄(47.5±10.1)岁。根据定位方式将患者分为乳腺托架组(41例)和体膜组(42例),2组患者在放疗前通过直线加速器在机载锥形束 CT(CBCT)下进行摆位验证。根据美国肿瘤放射治疗协作组制定的标准评估入组患者的急性和晚期放射性皮肤反应。摆位误差的组间比较采用t检验;计数资料的组间比较采用χ2检验。 结果 体膜组在左右(X轴)[(2.14±0.19) mm对(2.96±0.20) mm]、头脚(Y轴)[(2.49±0.15) mm对(3.05±0.16) mm]、腹背(Z轴)[(2.41±0.22) mm对(3.14±0.19) mm]方向的摆位误差明显小于乳腺托架组(t=2.98、2.63、2.49,均P<0.05);且在摆位误差≤3 mm时,Y轴方向体膜组分布比例高于乳腺托架组(72.20%对48.78%,χ2=7.23,P=0.01);在摆位误差>5 mm时,X轴(3.81%对8.78%)、Y轴(8.78%对33.17%)、Z轴(10.95%对24.88%)方向体膜组分布比例均低于乳腺托架组(χ2=4.37、12.40、13.73,均P<0.05);2组患者急性放射性皮肤反应发生率(30.95%对53.66%)的差异有统计学意义(χ2=4.39,P=0.04)。 结论 基于热塑体膜双重标记联合开窗技术定位方式减小了摆位误差、减轻了急性放射性皮肤反应,具有较好的稳定性和重复性,更安全可靠,且操作简捷。 Abstract:Objective To compare the radiotherapy positioning error and radiation skin response of post-breast conserving radiotherapy patients with breast cancer using breast bracket positioning and thermoplastic membrane double labeling combined with fenestration technology. The feasibility of the positioning method based on thermoplastic-membrane double labeling combined with fenestration technology was also explored. Methods The clinical data of 83 female patients post-breast conserving radiotherapy for breast cancer after breast-conserving surgery at the Fifth Affiliated Hospital of Zhengzhou University from January 2019 to December 2020 were retrospectively analyzed. The patients were aged (47.5±10.1) years. According to the positioning method, they were divided into breast-bracket group (41 cases) and body-membrane group (42 cases). Two groups of patients underwent positioning verification using a linear accelerator under airborne cone-beam CT before radiotherapy. Evaluated the acute and late radiation skin reactions in enrolled patients according to the standards established by the Radiation Therapy Oncology Group of United States. Intergroup comparison of the positioning error was conducted using the t-test, and intergroup comparison of the counting data was conducted using the chi-square test. Results Positioning errors in the left and right (X-axis) [(2.14±0.19) mm vs. (2.96±0.20) mm], head and foot (Y-axis) [(2.49±0.15) mm vs. (3.05±0.16) mm], and abdominal back (Z-axis)[(2.41±0.22) mm vs. (3.14±0.19) mm] directions of the body-membrane group were significantly lower than those of the breast-bracket group (t=2.98, 2.63, and 2.49, respectively; all P<0.05). When the positioning error was ≤3 mm, the distribution proportion of the body-membrane group in the Y-axis direction was higher than that of the breast-bracket group (72.20% vs. 48.78%; χ2=7.23, P=0.01), when the positioning error was >5 mm, the distribution proportion of body membrane in the X-axis(3.81% vs. 8.78%), Y-axis (8.78% vs. 33.17%), and Z-axis (10.95% vs. 24.88%) groups was lower than that of the breast-bracket group (χ2=4.37, 12.40, and 13.73, respectively; all P<0.05). The incidence of acute radiation skin reaction was significantly different between the two groups (30.95% vs. 53.66%; χ2=4.39, P=0.04). Conclusions The thermoplastic membrane double labeling combined with fenestration technology reduces the positioning error and alleviates acute radioactive skin reaction. It also has better stability and repeatability, is safer and more reliable, and is easy to operate. -
表 1 2组乳腺癌患者放疗定位的摆位误差比较(
$\bar x\pm s $ Table 1. Comparison of the positioning error of radiotherapy positioning in two groups of breast cancer patients (
$\bar x\pm s $ 组别 X轴 Y轴 Z轴 体膜组(n=42) 2.14±0.19 2.49±0.15 2.41±0.22 乳腺托架组(n=41) 2.96±0.20 3.05±0.16 3.14±0.19 t值 2.98 2.63 2.49 P值 <0.05 0.01 0.02 注:体膜组采用热塑体膜双重标记联合开窗技术定位;乳腺托架组采用乳腺托架定位 表 2 2组乳腺癌放疗患者在不同方向和区间的摆位误差分布比例比较[次(%)]
Table 2. Comparison of the proportion of setup error distribution in different directions and intervals between two groups of breast cancer patients undergoing radiotherapy [times (%)]
组别 X轴(mm) Y轴(mm) Z轴(mm) ≤3 3~5 >5 ≤3 3~5 >5 ≤3 3~5 >5 体膜组(n=42) 165(78.57) 37(17.62) 8(3.81) 130(72.20) 42(19.02) 38(8.78) 145(69.05) 42(20.00) 23(10.95) 乳腺托架组(n=41) 148(72.20) 39(19.02) 18(8.78) 100(48.78) 37(18.05) 68(33.17) 124(60.49) 30(14.63) 51(24.88) χ2值 2.28 0.14 4.37 7.23 0.26 12.40 3.33 2.28 13.73 P值 0.13 0.71 0.04 0.01 0.61 <0.05 0.07 0.13 <0.05 注:体膜组采用热塑体膜双重标记联合开窗技术定位;乳腺托架组采用乳腺托架定位 表 3 2组乳腺癌患者放疗后的皮肤不良反应比较(例)
Table 3. Comparison of skin adverse reactions after radiotherapy in two groups of breast cancer patients (cases)
组别 急性放射性皮肤反应 晚期放射性皮肤反应 0级 1级 2级 总发生率(%) 0级 1级 2级 总发生率(%) 体膜组(n=42) 29 11 2 30.95 40 2 0 4.76 乳腺托架组(n=41) 19 18 4 53.66 38 3 0 7.32 χ2值 4.39 0.24 P值 0.04 0.63 注:体膜组采用热塑体膜双重标记联合开窗技术定位;乳腺托架组采用乳腺托架定位 -
[1] Boyages J. Radiation therapy and early breast cancer: current controversies[J]. Med J Aust, 2017, 207(5): 216−222. DOI: 10.5694/mja16.01020. [2] Corradini S, Ballhausen H, Weingandt H, et al. Left-sided breast cancer and risks of secondary lung cancer and ischemic heart disease: effects of modern radiotherapy techniques[J]. Strahlenther Onkol, 2018, 194(3): 196−205. DOI: 10.1007/s00066-017-1213-y. [3] Ding Z, Zeng Q, Kang KL, et al. Evaluation of plan robustness using hybrid intensity-modulated radiotherapy (IMRT) and volumetric arc modulation radiotherapy (VMAT) for left-sided breast cancer[J/OL]. Bioengineering, 2022, 9(4): 131[2022-05-09]. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9028731. DOI: 10.3390/bioengineering9040131. [4] 殷蔚伯, 余子豪, 徐国镇, 等. 肿瘤放射治疗学[M]. 4版, 北京: 中国协和医科大学出版社, 2008: 208.
Yin WB, Yu ZH, Xu GZ, et al. Radiation oncology[M]. 4th ed. Beijing: Peking Union Medical College Press, 2008: 208.[5] 尹志海, 汪隽琦, 孟怡然, 等. 患者生理特征参数对乳腺癌调强放疗摆位误差影响的研究[J]. 中国癌症杂志, 2021, 31(3): 198−202. DOI: 10.19401/j.cnki.1007-3639.2021.03.006.
Yin ZH, Wang JQ, Meng YR, et al. Investigation of patient characteristics associated with setup errors in intensity-modulated radiotherapy after breast-conserving surgery[J]. China J Oncol, 2021, 31(3): 198−202. DOI: 10.19401/j.cnki.1007-3639.2021.03.006.[6] Lawler G. A review of surface guidance in extracranial stereotactic body radiotherapy (SBRT/SABR) for set-up and intra-fraction motion management[J/OL]. Tech Innov Patient Support Radiat Oncol, 2022, 21: 23−26[2022-05-09]. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8777133. DOI: 10.1016/j.tipsro.2022.01.001. [7] Li G, Lu W, O'Grady K, et al. A uniform and versatile surface-guided radiotherapy procedure and workflow for high-quality breast deep-inspiration breath-hold treatment in a multi-center institution[J/OL]. J Appl Clin Med Phys, 2022, 23(3): e13511[2022-05-09]. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8906224/. DOI: 10.1002/acm2.13511. [8] Jarvis LA, Hachadorian RL, Jermyn M, et al. Initial clinical experience of Cherenkov imaging in external beam radiation therapy identifies opportunities to improve treatment delivery[J]. Int J Radiat Oncol Biol Phys, 2021, 109(5): 1627−1637. DOI: 10.1016/j.ijrobp.2020.11.013. [9] 李敏杰, 黄平平. 基于体膜开窗定位的保乳术后大分割与常规分割的不良反应对比[J]. 中华放射医学与防护杂志, 2021, 41(4): 271−275. DOI: 10.3760/cma.j.issn.0254-5098.2021.04.006.
Li MJ, Huang PP. Comparison of adverse reactions between hypofractionated radiotherapy and conventional radiotherapy after breast conserving surgery based on body membrane fenestration[J]. Chin J Radiat Med Prot, 2021, 41(4): 271−275. DOI: 10.3760/cma.j.issn.0254-5098.2021.04.006.[10] Rubin P, Constine LS, Fajardo LF, et al. RTOG Late Effects Working Group. Overview: Late effects of normal tissues (LENT) scoring system[J]. Int J Radiat Oncol Biol Phys, 1995, 31(5): 1041−1042. DOI: 10.1016/0360-3016(95)00057-6. [11] McKenzie E, Razvi Y, Wronski M, et al. Trends and correlates of mean lung dose in patients receiving breast radiotherapy in a single institution from 2014 to 2018[J]. Clin Oncol (R Coll Radiol), 2020, 32(10): 647−655. DOI: 10.1016/j.clon.2020.05.010. [12] Chau OW, Fakir H, Lock M, et al. Dosimetric planning comparison for left-sided breast cancer radiotherapy: the clinical feasibility of four-dimensional-computed tomography-based treatment planning optimization[J/OL]. Cureus, 2022, 14(5): e24777[2022-05-09]. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9165918. DOI: 10.7759/cureus.24777. [13] Hodapp N. The ICRU report 83: prescribing, recording and reporting photon-beam intensity-modulated radiation therapy (IMRT)[J]. Strahlenther Onkol, 2012, 188(1): 97−99. DOI: 10.1007/s00066-011-0015-x. [14] 王新新, 梁广立, 高晓飞. 基于INFINITY加速器研究iSCOUT图像引导定位系统在乳腺癌保乳术后VMAT中的应用[J]. 吉林医学, 2022, 43(7): 1925−1927. DOI: 10.3969/j.issn.1004-0412.2022.07.066.
Wang XX, Liang GL, Gao XF. Study on the application of iSCOUT image guided localization system in VMAT after breast conserving surgery based on Infinity Accelerator[J]. Jilin Med J, 2022, 43(7): 1925−1927. DOI: 10.3969/j.issn.1004-0412.2022.07.066.[15] Penninkhof J, Fremeijer K, Offereins-van Harten K, et al. Evaluation of image-guided and surface-guided radiotherapy for breast cancer patients treated in deep inspiration breath-hold: a single institution experience[J/OL]. Tech Innov Patient Support Radiat Oncol, 2022, 21: 51−57[2022-05-09]. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8861395. DOI: 10.1016/j.tipsro.2022.02.001. [16] 李俊禹, 李廷廷, 陈吉祥, 等. 体膜联合乳腺托架固定在乳腺癌保乳术后放疗中的应用[J]. 实用癌症杂志, 2017, 32(4): 556−558. DOI: 10.3969/j.issn.1001-5930.2017.04.010.
Li JY, Li TT, Chen JX, et al. Application of body membrane combined with breast bracket in postoperative radiotherapy for breast cancer patients[J]. Pract J Cancer, 2017, 32(4): 556−558. DOI: 10.3969/j.issn.1001-5930.2017.04.010.[17] 黄店, 易海振. 真空垫固定技术在乳腺癌调强放疗中的应用分析[J]. 黑龙江医学, 2020, 44(3): 325−327. DOI: 10.3969/j.issn.1004-5775.2020.03.013.
Huang D, Yi HZ. Analysis of the application of vacuum pad fixed technology intensity-modulated radiotherapy (IMRT) in breast cancer[J]. Heilongjiang Med J, 2020, 44(3): 325−327. DOI: 10.3969/j.issn.1004-5775.2020.03.013.[18] 吴传锋, 吴锦昌, 顾科, 等. 水固化头枕对提高乳腺托架固定下乳腺癌放疗锁骨上野摆位准确性的研究[J]. 中华放射医学与防护杂志, 2017, 37(9): 686−689. DOI: 10.3760/cma.j.issn.0254-5098.2017.09.009.
Wu CF, Wu JC, Gu K, et al. Study on improving accuracy of setup errors of supraclavicular field in radiotherapy for breast cancer by breast bracket and moisture-cured resin cushion[J]. Chin J Radiol Med Prot, 2017, 37(9): 686−689. DOI: 10.3760/cma.j.issn.0254-5098.2017.09.009.[19] 谢涛, 许青, 彭佳元, 等. 乳腺癌胸壁野结合锁骨上野放疗时头部固定的重要性研究[J]. 中华放射肿瘤学杂志, 2018, 27(5): 500−503. DOI: 10.3760/cma.j.issn.1004-4221.2018.05.013.
Xie T, Xu Q, Peng JY, et al. Study of significance of head fixation in the chest wall field combined with supraclavicular field radiotherapy for breast cancer[J]. Chin J Radiat Oncol, 2018, 27(5): 500−503. DOI: 10.3760/cma.j.issn.1004-4221.2018.05.013.[20] 史俊俊. 不同体位固定技术在胸腹部肿瘤放射治疗中的应用差异分析[J]. 临床医药文献杂志, 2017, 4(36): 6960−6961. DOI: 10.16281/j.cnki.jocml.2017.36.018.
Shi JJ. Differential analysis of the application of isotope fixation technique in radiotherapy for thoracic and abdominal tumors[J]. J Clin Med Literat, 2017, 4(36): 6960−6961. DOI: 10.16281/j.cnki.jocml.2017.36.018. -





 下载:
下载: