-
原发性甲状旁腺功能亢进症是由甲状旁腺原发病变引起的甲状旁腺激素水平明显增高而导致的全身多系统改变的疾病,以甲状旁腺腺瘤最为多见[1],而骨棕色瘤是在此基础上发生的骨骼系统的一种良性病变,比较罕见,极易误诊。笔者报道了1例由甲状旁腺腺瘤继发多发骨棕色瘤患者的18F-FDG PET/CT影像学特点及诊断过程,并进行相关文献复习及鉴别诊断,旨在为临床诊疗提供参考。
-
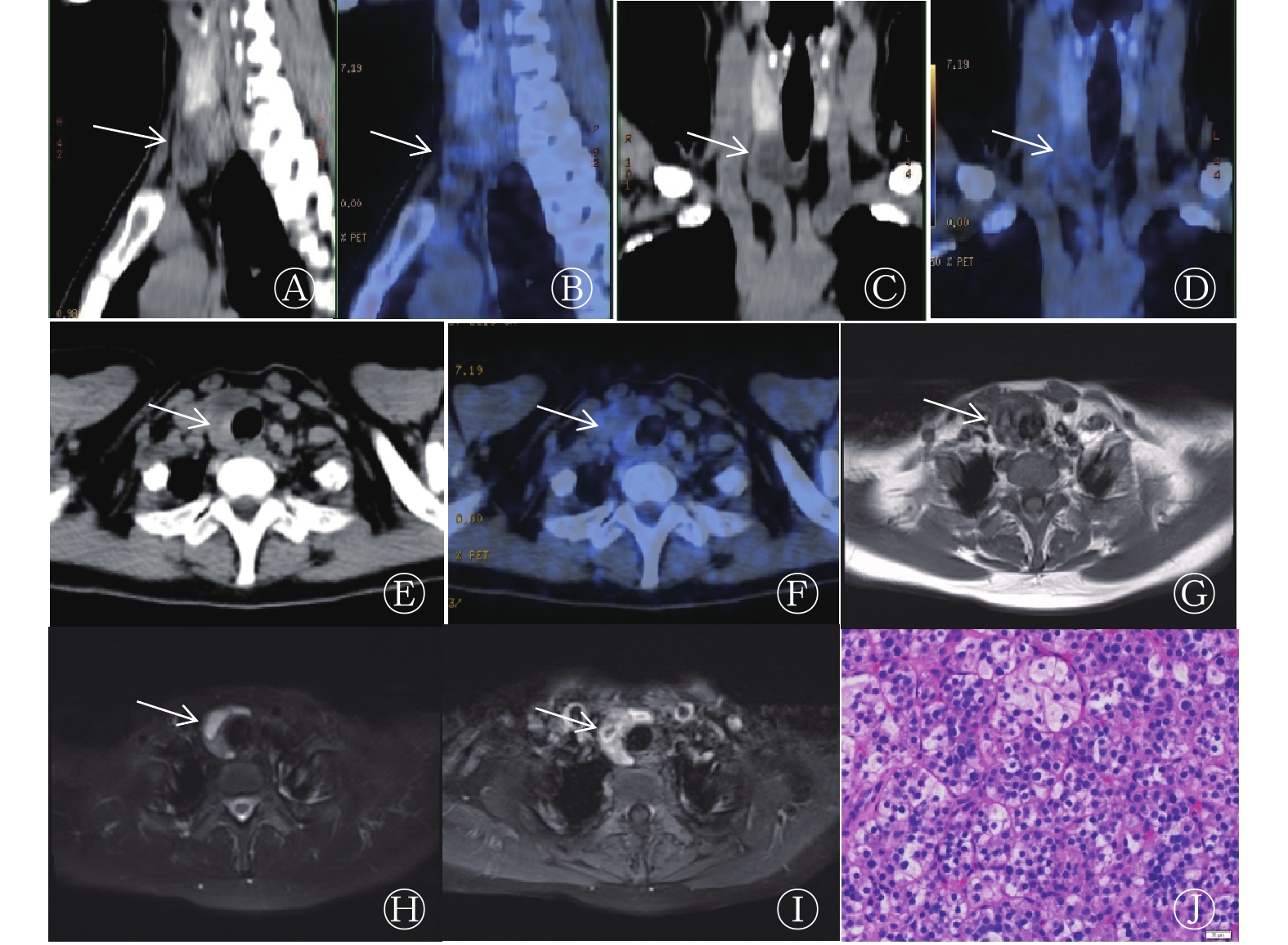
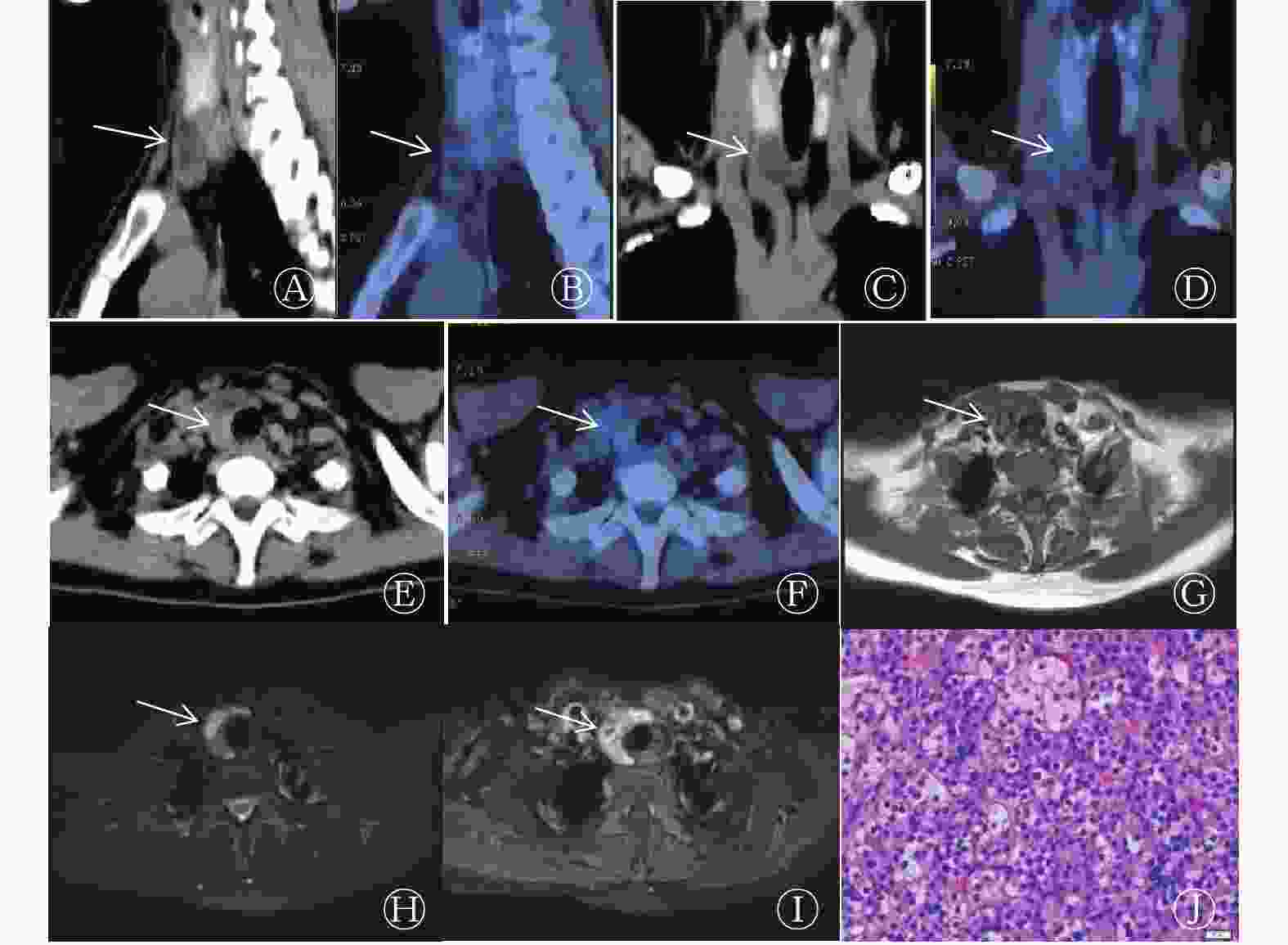
患者女性,48岁,因“右胸间断性隐痛3年,加重半月余”于湖北省肿瘤医院就诊。既往因胆囊结石行胆囊切除。入院查体结果:浅表淋巴结未扪及明显肿大;双肺呼吸音正常,未闻及明显干湿性啰音;心脏听诊结果正常;腹平软,未扪及包块,无压痛及反跳痛,无移动性浊音;双下肢无肿胀。18F-FDG PET/CT显像结果:甲状腺右侧叶前下方见一大小约2.1 cm×1.5 cm×2.4 cm的低密度结节影,边界清晰,未见明显异常放射性浓聚影(图1A~F);多处肋骨、多个胸腰椎、双侧髂骨见囊状骨质破坏区,边界清晰,边缘无硬化,其内及周围无钙化,未见明显软组织肿块,破坏区可见不同程度的放射性摄取增高,SUVmax为1.0~8.0(图2A~E);所探测范围内绝大部分骨骼骨密度普遍减小;双肾各见一长径约5 mm的结石。根据18F-FDG PET/CT表现,拟诊为多发性骨髓瘤,建议行穿刺活检对右髂骨高代谢病灶定性;甲状腺右侧叶病灶代谢不高,考虑为肿瘤性病变;双肾结石。实验室检查结果:降钙素水平为1.46 ng/L(女性正常参考值为0~6.40 ng/L),碱性磷酸酶水平为932 U/L(正常参考值为15~121 U/L),甲状旁腺激素水平为1734 pg/mL(正常参考值为15~65 pg/mL),血磷水平为0.68 mmol/L(正常参考值为0.81~1.65 mmol/L),血钙水平为3.21 mmol/L(正常参考值为1.97~2.85 mmol/L),甲状腺功能五项结果均正常。右髂骨病灶穿刺活检结果提示可能为棕色瘤(图2F~G)。MRI增强扫描结果:甲状腺右侧叶前下方见等T1、等长T2信号结节,边界尚清晰,最大截面大小约2.2 cm×1.7 cm,增强后明显强化(图1G~I)。患者在全麻下行右甲状旁腺肿瘤切除术。术后10 min验血结果显示,甲状旁腺激素水平(223 pg/mL)较手术当天清晨降低85.7%。术后组织病理学检查结果提示为右下甲状旁腺腺瘤(图1J)。免疫组织化学检查结果:CK8/18(+)、GATA-3(+)、CD56(小灶+)、Syn(+)、嗜铬素A(+)、甲状腺转录因子1(−)、 甲状腺球蛋白 (−)、衣原体 (−)、癌胚抗原 (−)、增殖细胞核抗原Ki-67(标记指数,1%)。术后行电解质紊乱对症治疗。出院时,甲状旁腺激素水平为53.81 pg/mL。目前随访发现患者一般情况好,未诉明显不适。
-
甲状旁腺腺瘤是原发性甲状旁腺功能亢进症最常见的病因,多见于中老年人,女性多于男性。功能性腺瘤会导致甲状旁腺激素分泌过多,引起高血钙、低血磷和尿钙磷增多,造成骨损害、肾结石等表现[2]。甲状旁腺功能亢进性骨病的主要表现包括弥漫性骨质疏松、局限性骨吸收并囊样变、出血形成骨棕色瘤[3]以及在此基础上导致的病理性骨折与畸形。由原发性甲状旁腺功能亢进所致的骨棕色瘤并不多见,约占4.5%[4]。骨棕色瘤的组织学特征为破骨细胞增生活跃,在骨吸收的同时骨形成也明显增强,同时伴有成纤维细胞增生[5],棕色是因为其中有丰富的血管及不同时期的出血导致的含铁血黄素沉积。
本例甲状旁腺腺瘤在18F-FDG PET/CT上表现为低密度结节影,放射性摄取不高。对于甲状旁腺腺瘤的18F-FDG PET/CT显像,不同的研究其诊断灵敏度差别很大,一般不提倡使用[6],但18F-FDG PET/CT对骨棕色瘤却有较高的诊断灵敏度[7]。本例骨棕色瘤在CT上表现为多发局限性骨质破坏影,边界较清,周围无硬化,其内及周围无钙化,无软组织肿块形成,PET于相应部位见放射性摄取不均匀,部分病灶代谢增高,部分病灶代谢不高。国内外大部分个案报道均显示骨棕色瘤呈明显异常放射性浓聚影[1, 7-8],只有1篇个案报道中的骨棕色瘤与本例有相似表现[9],但这篇个案与本例的不同之处在于其甲状旁腺腺瘤放射性摄取明显异常增高。对于本例骨棕色瘤的不同代谢表现是否与疾病发生的时间长短或破骨细胞的迁移活动有关,有待进一步研究。
18F-FDG PET/CT显像能提示甲状旁腺腺瘤引起的多系统病变,如甲状旁腺区肿瘤、肾结石、全身骨骼骨质破坏范围及相应的18F-FDG摄取情况等,还能指导临床医师确定穿刺活检的部位,对该病的诊断具有重要意义。但18F-FDG PET/CT显像对该病的诊断并不具有特异性,需要密切结合临床病史及实验室检查指标综合判断,同时需要与以下疾病相鉴别:(1)多发性骨髓瘤,多发于40岁以上男性,易侵犯富含红骨髓的骨骼,本周蛋白可升高,18F-FDG PET/CT显像多表现为溶骨性骨质破坏且代谢不均匀性增高,也可见骨质稀疏,伴高钙血症,与骨棕色瘤难鉴别,也是导致本例误诊的原因;(2)溶骨性骨转移,多见于中轴骨,手足骨罕见,可形成软组织肿块,18F-FDG PET/CT显像代谢一般明显增高。
利益冲突 本研究由署名作者按以下贡献声明独立开展,不涉及任何利益冲突。
作者贡献声明 李蕾负责病例的收集、方法的建立、论文的撰写;彭辽河负责病例的分析;罗娜娜负责方法的建立、文献的查阅;胡晓燕负责论文的审阅。
甲状旁腺腺瘤继发多发骨棕色瘤18F-FDG PET/CT显像一例
18F-FDG PET/CT of multiple brown bone tumors secondary to parathyroid adenoma: a case report
-
摘要: 笔者报道了1例甲状旁腺腺瘤继发多发骨棕色瘤18F-氟脱氧葡萄糖(FDG) PET/CT显像的病例,关于该病的个案报道并不少见,但因该病例的骨棕色瘤18F-FDG代谢特点与以往报道中的病例有所不同,故被误诊为多发骨髓瘤。笔者主要分析了骨棕色瘤18F-FDG PET/CT的显像特点并进行文献复习、病理分析及鉴别诊断,以期为18F-FDG PET/CT显像对骨棕色瘤的诊断提供更多参考。Abstract: The author reported a case of multiple brown bone tumors secondary to parathyroid adenoma by 18F-fluorodeoxyglucose (FDG) PET/CT. Although the disease was not rare, the 18F-FDG metabolic characteristics of this case are different from those of other reported cases, so it was misdiagnosed as multiple myeloma. The author mainly analyzed the characteristics of 18F-FDG PET/CT of brown bone tumor, and carried out literature review, pathological analysis and differential diagnosis, in order to provide more reference for 18F-FDG PET/CT in the diagnosis of brown bone tumor.
-
Key words:
-
-
[1] 胡娜, 肖立志, 吴永港, 等. 原发性甲状旁腺功能亢进症PET-CT表现1例[J]. 中南大学学报(医学版), 2015, 40(6): 697−701. DOI: 10.11817/j.issn.1672-7347.2015.06.021.
Hu N, Xiao LZ, Wu YG, et al. A case of PET-CT imaging for primary hyperparathyroidism[J]. J Cent South Univ: Med Sci, 2015, 40(6): 697−701. DOI: 10.11817/j.issn.1672-7347.2015.06.021.[2] 王慧明, 王仁法. 棕色瘤误诊一例[J]. 临床放射学杂志, 2015, 34(4): 668. DOI: 10.13437/j.cnki.jcr.2015.04.049.
Wang HM, Wang RF. One case of misdiagnosis of brown tumor[J]. J Clin Radiol, 2015, 34(4): 668. DOI: 10.13437/j.cnki.jcr.2015.04.049.[3] 杨玲, 蔡亮, 丁浩源, 等. 18F-NaF PET/CT骨显像在甲状旁腺功能亢进性骨病中的应用[J]. 国际放射医学核医学杂志, 2019, 43(2): 132−139. DOI: 10.3760/cma.j.issn.1673-4114.2019.02.007.
Yang L, Cai L, Ding HY, et al. Application of 18F-NaF PET/CT bone scintigraphy to hyperparathyroid bone disease[J]. Int J Radiat Med Nucl Med, 2019, 43(2): 132−139. DOI: 10.3760/cma.j.issn.1673-4114.2019.02.007.[4] Jouan A, Zabraniecki L, Vincent V, et al. An unusual presentation of primary hyperparathyroidism: severe hypercalcemia and multiple brown tumors[J]. Joint Bone Spine, 2008, 75(2): 209−211. DOI: 10.1016/j.jbspin.2007.03.004. [5] 郑原印, 刘晓斌, 毛瑛玉, 等. 甲状旁腺腺瘤继发纤维囊性骨炎1例[J]. 诊断病理学杂志, 2020, 27(9): 663−664. DOI: 10.3969/j.issn.1007-8096.2020.09.014.
Zheng YY, Liu XB, Mao YY, et al. Fibrocystic osteitis secondary to parathyroid adenoma: a case report[J]. Chin J Diagn Pathol, 2020, 27(9): 663−664. DOI: 10.3969/j.issn.1007-8096.2020.09.014.[6] Kluijfhout WP, Pasternak JD, Drake FT, et al. Use of PET tracers for parathyroid localization: a systematic review and meta-analysis[J]. Langenbeck's Arch Surg, 2016, 401(7): 925−935. DOI: 10.1007/s00423-016-1425-0. [7] Penhoat MG, Drui D, Ansquer C, et al. Contribution of 18-FDG PET/CT to brown tumor detection in a patient with primary hyperparathyroidism[J]. Joint Bone Spine, 2017, 84(2): 209−212. DOI: 10.1016/j.jbspin.2016.06.007. [8] Hu JB, He SH, Yang J, et al. Management of brown tumor of spine with primary hyperparathyroidism: a case report and literature review[J]. Medicine, 2019, 98(14): e15007. DOI: 10.1097/MD.0000000000015007. [9] Guy MS, Jacob C, McDonald SD, et al. 18F-FDG PET/CT metabolic variability in functioning oncocytic parathyroid adenoma with brown tumors[J]. Clin Nucl Med, 2014, 39(4): 393−395. DOI: 10.1097/RLU.0000000000000380. -





 下载:
下载: