-
老年性骨质疏松症(osteoporosis,OP)患者易发生骨质疏松性椎体压缩性骨折(osteoporotic vertebral compression fractures,OVCF)。CT、X射线、MRI和99Tcm-MDP全身骨显像常用于OVCF的诊断,在确诊OVCF的患者中,MRI和99Tcm-MDP全身骨显像能鉴别新鲜与陈旧性OVCF,有利于临床尽早干预。本研究回顾性分析104例因急慢性腰背部疼痛行99Tcm-MDP全身骨显像的老年性OP患者的临床资料和其他影像学资料,评价99Tcm-MDP身骨显像对老年性OP患者新鲜OVCF的筛查价值。
-
回顾性分析2017年1月至2019年12月于厦门大学附属中山医院因急慢性腰背部疼痛行99Tcm-MDP全身骨显像的104例老年性OP患者的临床资料和其他影像学资料(发生急性腰背部疼痛的患者均在1周内完成99Tcm-MDP全身骨显像),其中男性33例、女性71例,年龄62~88(78.8±7.7)岁。所有患者均有本院椎体X射线检查结果,其中,37例患者有本院胸椎或腰椎MRI检查结果。根据患者年龄分为60~69岁组(42例)、70~79岁组(43例)和≥80岁组(19例);根据疼痛发作时间分为急性疼痛组(78例)和慢性疼痛组(26例),急性疼痛是指疼痛发作时间在1个月之内,或原有慢性疼痛在近1个月内新发剧烈疼痛;慢性疼痛是指持续性腰背部疼痛,多在3个月以上,且近期无新发剧烈疼痛。纳入标准:(1)OP诊断明确[1],有骨密度检查报告,经双能X射线吸收检测确诊为OP,X射线检查结果显示有椎体存在OVCF;(2)病史长,病程2年以上;(3)意识清晰,能正常交流和表述。排除标准:有肿瘤病史或严重感染性疾病。所有患者均于检查前签署了知情同意书。本研究符合《赫尔辛基宣言》的原则。
-
骨显像剂99Tcm-MDP由厦门大学附属中山医院核医学科制备,放射化学纯度>95%。钼-锝发生器由北京原子高科股份有限公司提供,MDP试剂盒由北京师宏药物研制中心提供。显像仪器为美国GE公司Infinia Hawkeye型SPECT扫描仪,配低能高分辨准直器。
-
患者经静脉注射99Tcm-MDP 740~925 MBq,嘱其多饮水(约1 500 mL)、多排尿;2~3 h后行全身骨显像,显像前排空膀胱尿液。显像条件:矩阵1024×256,扫描速度13~18 cm/min,放大倍数1.0。
-
由2位高年资核医学科医师(副高级职称及以上)对99Tcm-MDP全身骨显像图像进行分析,对X射线检查结果显示的OVCF椎体在99Tcm-MDP全身骨显像中是否有放射性浓聚及浓聚的程度作出新鲜或陈旧性OVCF的诊断,意见不一致时由2位医师讨论以作出最终诊断。新鲜OVCF的诊断:X射线检查结果显示椎体出现OVCF,在99Tcm-MDP全身骨显像中病灶椎体表现为显著增强的条状或线状放射性浓聚;陈旧性OVCF的诊断:X射线检查结果显示椎体变扁,99Tcm-MDP全身骨显像显示相应椎体无放射性浓聚或轻度浓聚;既往陈旧性OVCF的近期99Tcm-MDP全身骨显像显示放射性浓聚则按照新鲜OVCF处理。
-
应用SPSS 17.0软件进行统计学分析。各组数据以例数和百分比表示,组间比较采用χ2检验。P<0.05为差异有统计学意义。
-
在104例因急慢性腰背部疼痛行99Tcm-MDP全身骨显像的老年性OP患者中共检出75例(72.1%)患有新鲜OVCF的患者,且急性疼痛组患者新鲜OVCF的检出率高于慢性疼痛组[87.2%(68/78)对26.9%(7/26),χ2=35.209,P<0.001];在60~69岁组、70~79岁组和≥80岁组患者中,新鲜OVCF的检出率分别为66.7%(28/42)、76.7%(33/43)、73.7%(14/19),差异无统计学意义(χ2=1.101,P>0.05);在60~69岁组、70~79岁组和≥80岁组中,发生急性疼痛的患者新鲜OVCF的检出率均高于发生慢性疼痛的患者(83.9%对18.2%、88.6%对25.0%、91.7%对42.9%,均P<0.05,表1)。
组别 急性疼痛 慢性疼痛 χ2值 P值 阳性
(n=68)阴性
(n=10)阳性
(n=7)阴性
(n=19)60~69岁组(n=42) 26(83.9) 5(16.1) 2(18.2) 9(81.8) 12.948 <0.001 70~79岁组(n=43) 31(88.6) 4(11.4) 2(25.0) 6(75.0) 11.398 <0.001 ≥80岁组(n=19) 11(91.7) 1(8.3) 3(42.9) 4(57.1) 5.456 0.020 注:阳性表示99Tcm-MDP全身骨显像检出新鲜骨质疏松性椎体压缩性骨折的患者;阴性表示99Tcm-MDP全身骨显像未检出新鲜骨质疏松性椎体压缩性骨折的患者。MDP为亚甲基二膦酸盐 表 1 不同年龄组的老年性骨质疏松症患者99Tcm-MDP全身骨显像对新鲜骨质疏松性椎体压缩性骨折检出率的比较[例(%)]
Table 1. Comparison of detection rates of fresh osteoporotic vertebral compression fractures by 99Tcm-MDP whole-body bone scan in geriatric patients with osteoporosis in different age groups (case (%))
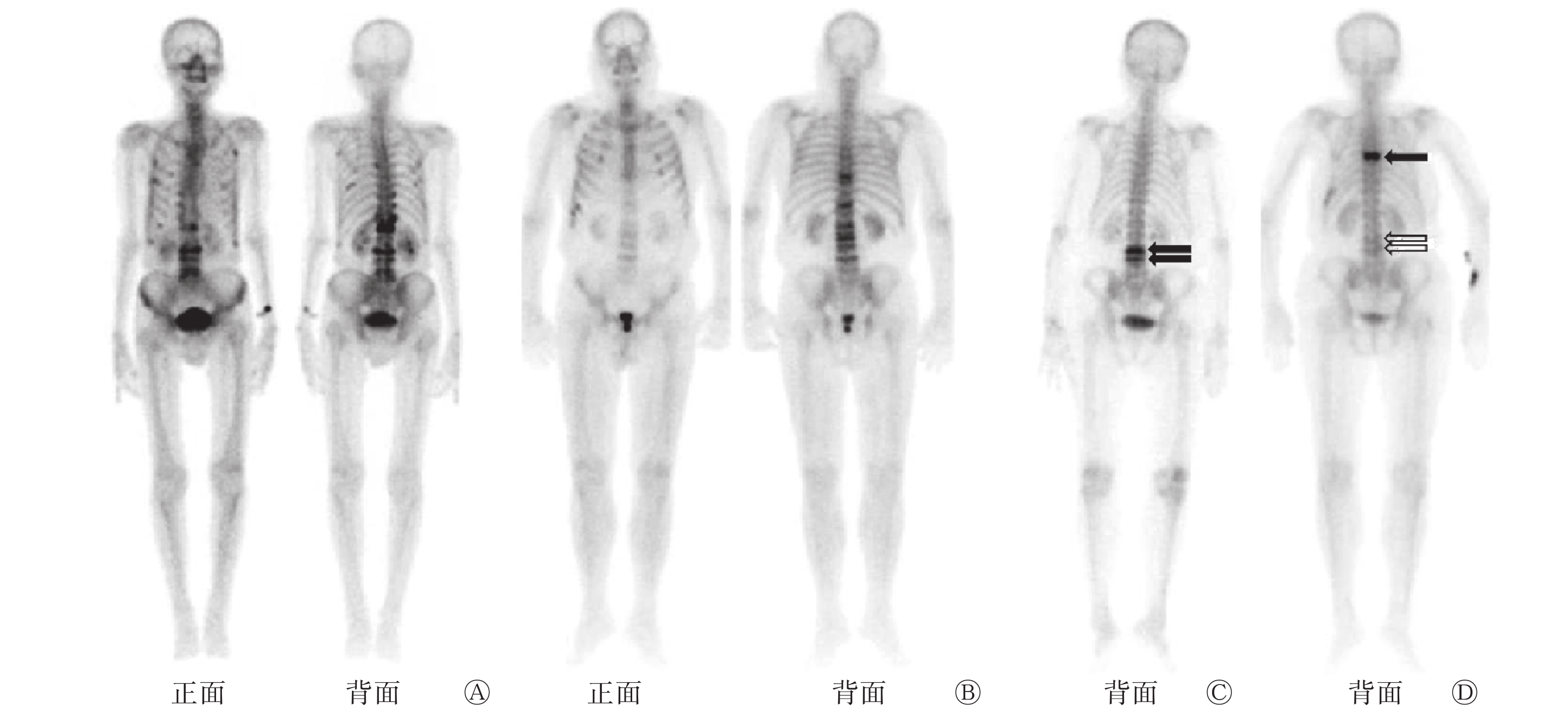
在检出新鲜OVCF的75例患者中,15例患者(20.0%)有2个或2个以上椎体同时新发OVCF,其中2例患者因发生急性腰背部疼痛行99Tcm-MDP全身骨显像均检出4个以上椎体发生新鲜OVCF(图1A、B);其余60例患者(80.0%)均为单个椎体发生新鲜OVCF,其中3例患者前后2次因急性腰背部疼痛行99Tcm-MDP全身骨显像均检出新鲜OVCF。图1C、D所示的患者2年前因急性腰背部疼痛发现L3、L4椎体发生新鲜OVCF,经骨水泥治疗后转为慢性腰背部疼痛并逐渐缓解,2年后该患者再发急性腰背部疼痛,行99Tcm-MDP全身骨显像发现T7椎体有放射性异常浓聚,L3、L4椎体有放射性轻度浓聚,并已转为陈旧性OVCF。此外,有7例患者(9.3%)同时合并双侧或单侧多枚肋骨斜形条状放射性浓聚,诊断为肋骨新鲜骨折。

图 1 3例急性腰背部疼痛的老年性骨质疏松症患者的99Tcm-MDP全身骨显像图
Figure 1. 99Tcm-MDP whole-body bone scan images of 3 geriatric patients with osteoporosis after acute low back pain
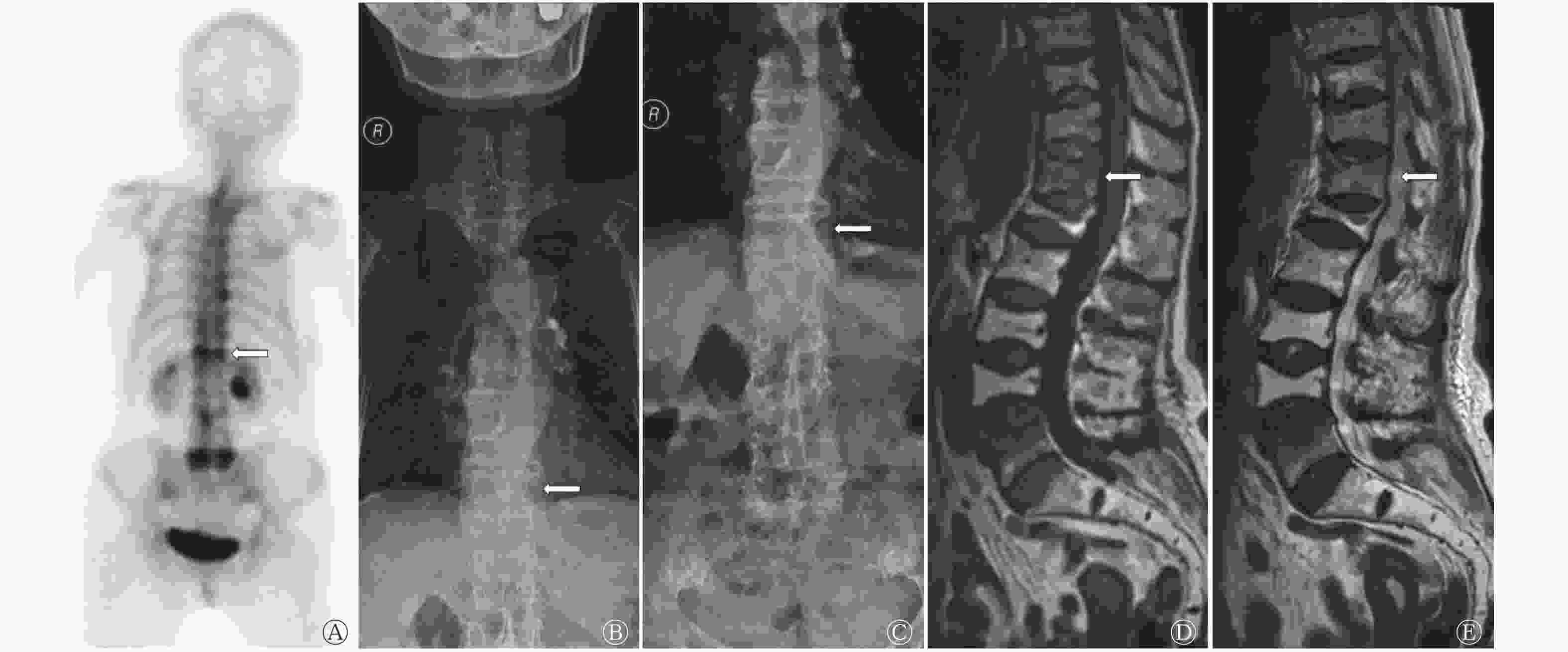
MRI能够依据椎体T1、T2信号的长短来判断OVCF的新旧程度,99Tcm-MDP全身骨显像则可以依据放射性浓聚程度进行判断。如图2所示,1例慢性腰背部疼痛近期加重的74岁老年女性OP患者的X射线检查结果显示,其胸腰椎体均有不同程度的OVCF;99Tcm-MDP全身骨显像显示,其T12、L5椎体条状异常放射性浓聚,提示为新鲜OVCF,其余椎体轻度放射性浓聚,且多位于椎体边缘,为陈旧OVCF;MRI显示其T12、L5椎体呈长T1、长T2信号,提示为新鲜OVCF,其余椎体提示为陈旧性OVCF。
-
OVCF的起因多是长期骨质疏松导致椎体骨密度和骨质量下降、骨强度降低,从而使椎体在轻微外力的作用下甚至无明显外力时发生骨折。OVCF在老年性OP患者中非常常见,且随着患者年龄的增大和骨质疏松程度的加深而更易发生[1]。OVCF在临床上的主要症状是胸部和(或)腰背部疼痛,伴有或不伴有下肢神经症状[2]。由于多无明显外伤史,除非发生剧烈疼痛,否则OP患者很容易忽视腰背部疼痛的症状,从而失去早期诊治的机会。
本研究中有78例OP患者为近期出现程度不等的腰背部疼痛,或在原腰背部疼痛的基础上出现新的疼痛部位(即急性疼痛组),其中99Tcm-MDP全身骨显像共检出68例患者(87.2%)存在新鲜OVCF,在≥80岁组的12例患者中检出11例患者(91.7%)存在新鲜OVCF。在各年龄分组的OP患者中,因急性疼痛而检出新鲜OVCF的比率均超过83%,在26例发生慢性疼痛的OP患者中,99Tcm-MDP全身骨显像检出7例患者(26.9%)存在新鲜OVCF,在≥80岁组的7例患者中检出3例患者(42.9%)存在新鲜OVCF。以上结果提示,老年性OP患者应重视腰背部疼痛症状,特别是急性腰背部疼痛,无论有无明显外伤史,均应及时就诊,及时治疗,从而改善生活质量。杨慧林等[3]与雷涛和申勇[4]的研究结果也显示,老年性OP患者腰背部疼痛是发生新鲜OVCF的重要提示信号,早诊断、早治疗对于减轻疼痛、促进椎体修复和尽早恢复生活自理能力意义重大。
经1次或多次X射线检查已确诊OVCF的老年性OP患者通过1次99Tcm-MDP全身骨显像即可显示全部椎体,椎体条状异常放射性浓聚提示为新鲜OVCF,轻度放射性浓聚提示为陈旧性OVCF,同时,99Tcm-MDP全身骨显像还可以显示其他部位的骨折,且灵敏度较高[5-6]。图1A、B所示的2例老年性OP患者因慢性腰背部疼痛近期加重而进行99Tcm-MDP全身骨显像,均检出4个以上椎体的新鲜OVCF,同时检出多根肋骨的新鲜骨折,部分椎体呈轻度放射性摄取,这表明该患者OVCF的发生时间有先后之分,部分OVCF经治疗和骨代谢修复后已转为陈旧性。
发生新鲜OVCF的患者经抗骨质疏松治疗、卧床休息和支具保护等保守治疗,或行经皮椎体成形术(PVP)、球囊扩张椎体后凸成形术(PKP)等手术治疗后多可缓解疼痛,恢复脊柱力学稳定性及神经稳定性,并提高生活质量[7]。多数老年性OP患者的病程较长,有的长达几十年,在长期的疾病过程中,不同椎体的OVCF会依次出现,新旧并存[8]。因此,及时检出新鲜OVCF、对责任椎体进行准确定位能为后续的治疗提供重要依据。图1C、D所示的老年性OP患者2年前因急性腰背部疼痛检出L3、L4椎体新鲜OVCF,并行骨水泥治疗,2年后该患者再发急性腰背部疼痛,其99Tcm-MDP全身骨显像显示L3、L4椎体结构稳定,呈轻度放射性摄取,即为陈旧性OVCF,而T7椎体为责任椎体。研究结果表明,在老年性OP患者发生急性腰背部疼痛时,99Tcm-MDP全身骨显像可作为筛查手段[9],特别是骨SPECT/CT可明确责任椎体[10],从而有利于临床尽早、准确地干预,减轻患者疼痛[11]。
99Tcm-MDP通过离子交换或化学吸附的方式沉积于骨上,99Tcm-MDP全身骨显像可反映骨骼的局部血流和骨代谢情况[12]。当发生骨折时,骨折部位的血流灌注增加,周边出现血肿及炎性细胞浸润,成骨细胞增殖活跃,这些因素促进了99Tcm-MDP的浓聚,骨显像可以灵敏地检出骨折部位。有研究结果表明,椎体骨折时骨小梁中断,早期即在骨小梁周围产生炎症反应,局部血流量增加,成骨细胞活跃,在伤后6~72 h即可表现为放射性浓聚[13]。新发骨折时放射性摄取显著增加,随着骨折修复,放射性浓聚程度缓慢下降。故在筛查新鲜OVCF时,99Tcm-MDP全身骨显像具有很大的优势[14],其不仅可以尽早明确是否为新鲜骨折,也可以鉴别新鲜与陈旧性骨折,并找出责任椎体,从而有利于临床积极干预。对于高度怀疑新鲜的隐匿性OVCF,常规X射线检查不能确诊时,99Tcm-MDP全身骨显像可用于早期筛查和诊断[15]。有文献报道,并非所有的骨显像放射性浓聚均在修复期后迅速消失,部分患者的放射性浓聚表现可以持续很长时间,甚至可达2年以上,其原因有待进一步研究,但此类患者仍可视为新鲜骨折[16]。针对新鲜OVCF进行积极治疗可以缓解患者的症状,减轻患者的生理和心理负担[17-18]。
MRI可以清晰显示椎体序列以及椎间盘、脊髓、血肿和韧带等软组织损伤,具有较高的诊断灵敏度和准确率,故被认为是诊断新鲜OVCF的“金标准”[19]。本研究对比在发生急慢性腰背部疼痛时,同时期进行X射线检查、99Tcm-MDP全身骨显像和MRI检查的37例患者的诊断结果,发现99Tcm-MDP全身骨显像和MRI对OVCF的检出率基本一致。本研究图2所示的老年性OP患者的X射线检查结果和MRI提示多个椎体呈压缩性改变,MRI可以清晰显示新鲜和陈旧性OVCF,但1次MRI检查无法评估所有椎体情况,难免遗漏,且部分安装起搏器或幽闭恐惧症患者不适合行MRI检查。本研究中104例老年性OP患者均行99Tcm-MDP全身骨显像,急性疼痛组的78例患者中有68例检出责任椎体,慢性疼痛组的26例患者中有7例检出责任椎体,未检出责任椎体的患者的其他影像学检查结果(特别是MRI)亦未发现新鲜OVCF。99Tcm-MDP全身骨显像是老年性OP患者发生急性腰背部疼痛时的检查手段之一,可作为临床检查的重要补充。
近年来,随着SPECT/CT装机数量的增加,其在诊断骨相关疾病中的应用愈加广泛,SPECT/CT在诊断OP所致的新鲜OVCF中具有很大的优势,灵敏度和特异度均较高。据报道,SPECT/CT骨扫描和MRI对新鲜OVCF具有相近的高检出率[13, 20]。在指导手术定位及后续治疗等方面,SPECT/CT骨扫描对新鲜OVCF的检出率明显高于全身骨显像,但因SPECT/CT设备并未普及,故其应用还不能全面展开。对于有条件的医院,我们积极建议常规或者对可疑病灶行SPECT/CT骨扫描以筛查新鲜OVCF,对尚未普及SPECT/CT的医院,全身骨显像具有方便、快捷和费用低廉等优势,老年性OP患者一旦发生急性腰背部疼痛,可第一时间进行99Tcm-MDP全身骨显像,辅以X射线检查,并对检出的可疑病灶进一步行MRI或CT予以鉴别诊断,从而引起患者的重视,提高患者的就诊率和对该病的检出率。
利益冲突 本研究由署名作者按以下贡献声明独立开展,不涉及任何利益冲突。
作者贡献声明 王卫星负责命题的提出与设计、研究过程的指导、数据的分析、论文的撰写;马超负责命题的提出、数据的获取与分析、论文的审阅与修订。
99Tcm-MDP全身骨显像对老年性骨质疏松症患者新鲜骨质疏松性椎体压缩性骨折的筛查价值
Value of 99Tcm-MDP whole-body bone scan in screening fresh osteoporotic vertebral compression fractures in geriatric patients with osteoporosis
-
摘要:
目的 探讨99Tcm-亚甲基二膦酸盐(MDP)全身骨显像在老年性骨质疏松症(OP)患者发生急慢性腰背部疼痛时对新鲜骨质疏松性椎体压缩性骨折(OVCF)的筛查价值。 方法 回顾性分析2017年1月至2019年12月于厦门大学附属中山医院因急慢性腰背部疼痛行99Tcm-MDP全身骨显像的104例老年性OP患者的临床资料和其他影像学资料,其中男性33例、女性71例,年龄62~88(78.8±7.7)岁。将患者根据年龄分为60~69岁组(42例)、70~79岁组(43例)和≥80岁组(19例);根据疼痛发作时间分为急性疼痛组(78例)和慢性疼痛组(26例)。参考X射线检查结果,分析所有患者的99Tcm-MDP全身骨显像图像,计算其对新鲜OVCF的检出率。组间比较采用χ2检验。 结果 99Tcm-MDP全身骨显像对104例老年性OP患者新鲜OVCF的检出率为72.1%(75/104),急性疼痛组患者新鲜OVCF的检出率高于慢性疼痛组[87.2%(68/78)对26.9%(7/26),χ2=35.209,P<0.001],60~69岁组、70~79岁组、≥80岁组患者新鲜OVCF的检出率分别为66.7%(28/42)、76.7%(33/43)、73.7%(14/19),差异无统计学意义(χ2=1.101,P>0.05)。在3个年龄组患者中,发生急性疼痛的患者新鲜OVCF的检出率均高于发生慢性疼痛的患者[83.9%(26/31)对18.2%(2/11)、88.6%(31/35)对25.0%(2/8)、91.7%(11/12)对42.9%(3/7),χ2=12.948、11.398、5.456,均P<0.05]。已检出的新鲜OVCF中累及单个椎体的患者占80.0%(60/75),累及2个及2个以上椎体的患者占20.0%(15/75)。 结论 99Tcm-MDP全身骨显像在老年性OP患者发生腰背部疼痛(特别是急性腰背部疼痛)时对新鲜OVCF具有临床筛查价值。 Abstract:Objective To investigate the value of 99Tcm-methylenediphosphonate (MDP) whole-body bone scan in screening fresh osteoporotic vertebral compression fractures (OVCF) in geriatric patients with osteoporosis (OP) and acute or chronic low back pain. Methods The clinical data and other imaging data of 104 geriatric patients with OP who underwent 99Tcm-MDP whole-body bone scan for acute or chronic low back pain in Zhongshan Hospital Xiamen University from January 2017 to December 2019 were analyzed retrospectively. The patients included 33 males and 71 females aged 62–88 (78.8±7.7) years old. The patients were divided into 60–69 years old group (n=42), 70–79 years old group (n=43), and ≥80 years old group (n=19) according to their age and were divided into acute pain group (n=78) and chronic pain group (n=26) according to the pain onset time. With reference to X-ray examination results, the 99Tcm-MDP whole-body bone scan images of all patients were analyzed, and the detection rates of fresh OVCF were calculated. χ2 test was used for comparison among groups. Results The detection rate of fresh OVCF in 104 geriatric patients with OP by 99Tcm-MDP whole-body bone scan was 72.1% (75/104), and the detection rate of fresh OVCF in the acute pain group was higher than that in the chronic pain group (87.2% (68/78) vs. 26.9% (7/26), χ2=35.209, P<0.001). The detection rates of fresh OVCF in the three age groups were 66.7% (28/42), 76.7% (33/43), and 73.7% (14/19), respectively, and the difference was not statistically significant (χ2=1.101, P>0.05). Among the three age groups, the detection rates of fresh OVCF in patients with acute pain was higher than that in patients with chronic pain (83.9% (26/31) vs. 18.2% (2/11), 88.6% (31/35) vs. 25.0% (2/8), 91.7% (11/12) vs. 42.9% (3/7); χ2=12.948, 11.398, 5.456; all P<0.05). Among the fresh OVCF detected, 80.0% (60/75) involved a single vertebral body, and 20.0% (15/75) involved two or more vertebral bodies. Conclusion 99Tcm-MDP whole-body bone scan has clinical screening value for fresh OVCF when low back pain (especially acute low back pain) occurs in geriatric patients with OP. -
表 1 不同年龄组的老年性骨质疏松症患者99Tcm-MDP全身骨显像对新鲜骨质疏松性椎体压缩性骨折检出率的比较[例(%)]
Table 1. Comparison of detection rates of fresh osteoporotic vertebral compression fractures by 99Tcm-MDP whole-body bone scan in geriatric patients with osteoporosis in different age groups (case (%))
组别 急性疼痛 慢性疼痛 χ2值 P值 阳性
(n=68)阴性
(n=10)阳性
(n=7)阴性
(n=19)60~69岁组(n=42) 26(83.9) 5(16.1) 2(18.2) 9(81.8) 12.948 <0.001 70~79岁组(n=43) 31(88.6) 4(11.4) 2(25.0) 6(75.0) 11.398 <0.001 ≥80岁组(n=19) 11(91.7) 1(8.3) 3(42.9) 4(57.1) 5.456 0.020 注:阳性表示99Tcm-MDP全身骨显像检出新鲜骨质疏松性椎体压缩性骨折的患者;阴性表示99Tcm-MDP全身骨显像未检出新鲜骨质疏松性椎体压缩性骨折的患者。MDP为亚甲基二膦酸盐 -
[1] 章振林, 金小岚, 夏维波. 原发性骨质疏松症诊疗指南(2017版)要点解读[J]. 中华骨质疏松和骨矿盐疾病杂志, 2017, 10(5): 411−412. DOI: 10.3969/j.issn.1674-2591.2017.05.001.
Zhang ZL, Jin XL, Xia WB. Guidelines for diagnosis and treatment of primary osteoporosis (2017 edition): essential introduction[J]. Chin J Osteoporos Bone Miner Res, 2017, 10(5): 411−412. DOI: 10.3969/j.issn.1674-2591.2017.05.001.[2] 王复案, 陈允震. 骨质疏松性椎体压缩性骨折诊疗现状及其对策[J]. 中国骨质疏松杂志, 2019, 25(5): 590−594, 599. DOI: 10.3969/j.issn.1006-7108.2019.05.004.
Wang FA, Chen YZ. The current diagnosis and treatment status and strategies for osteoporotic vertebral compression fracture[J]. Chin J Osteoporos, 2019, 25(5): 590−594, 599. DOI: 10.3969/j.issn.1006-7108.2019.05.004.[3] 杨惠林, 刘强, 唐海. 重视我国骨质疏松性椎体压缩骨折的规范化诊疗[J]. 中华医学杂志, 2016, 96(48): 3857−3861. DOI: 10.3760/cma.j.issn.0376-2491.2016.48.001.
Yang HL, Liu Q, Tang H. Attach importance to the standardized diagnosis and treatment of osteoporotic vertebral compression fractures in China[J]. Natl Med J China, 2016, 96(48): 3857−3861. DOI: 10.3760/cma.j.issn.0376-2491.2016.48.001.[4] 雷涛, 申勇. 老年骨质疏松性椎体骨折若干问题的探讨[J/OL]. 中华老年骨科与康复电子杂志, 2017, 3(4): 248−251[2020-10-22]. DOI: 10.3877/cma.j.issn.2096-0263.2017.04.010. http://zhlngkykfdzzz.cthhmu.com/oa/DArticle.aspx?type=view&id=201704010.
Lei T, Shen Y. A brief discussion of osteoporotic vertebral fractures in elderly patients[J/OL]. Chin J Geriatr Orthop Rehbil: Electron Ed, 2017, 3(4): 248−251[2020-10-22]. DOI: 10.3877/cma.j.issn.2096-0263.2017.04.010. http://zhlngkykfdzzz.cthhmu.com/oa/DArticle.aspx?type=view&id=201704010.[5] 周义, 赵御森, 张志敏, 等. SPECT/CT骨显像诊断新发骨质疏松性椎体压缩骨折的价值[J]. 中国医学影像技术, 2019, 35(4): 630−632. DOI: 10.13929/j.1003-3289.201811081.
Zhou Y, Zhao YS, Zhang ZM, et al. Value of SPECT/CT bone imaging in diagnosis of new-onset osteoporotic vertebral compression fractures[J]. Chin J Med Imaging Technol, 2019, 35(4): 630−632. DOI: 10.13929/j.1003-3289.201811081.[6] 江晓兵, 莫凌, 姚珍松, 等. SPECT、SPECT-CT与MRI对新鲜骨质疏松性椎体压缩骨折的诊断价值[J]. 中国脊柱脊髓杂志, 2013, 23(10): 891−897. DOI: 10.3969/j.issn.1004-406X.2013.10.05.
Jiang XB, Mo L, Yao ZS, et al. The value of SPECT, SPECT-CT and MRI in the diagnosis of fresh osteoporotic vertebral compressive fracture[J]. Chin J Spine Spinal Cord, 2013, 23(10): 891−897. DOI: 10.3969/j.issn.1004-406X.2013.10.05.[7] Rousing R, Hansen KL, Andersen MO, et al. Twelve-months follow-up in forty-nine patients with acute/semiacute osteoporotic vertebral fractures treated conservatively or with percutaneous vertebroplasty: a clinical randomized study[J]. Spine (Phila Pa 1976), 2010, 35(5): 478−482. DOI: 10.1097/BRS.0b013e3181b71bd1. [8] 莫欣, 陈奇凡, 黄海. 骨质疏松性椎体压缩性骨折椎体成形术后再发骨折的影响因素分析[J]. 微创医学, 2020, 15(4): 433−436, 445. DOI: 10.11864/j.issn.1673.2020.04.05.
Mo X, Chen QF, Huang H. Analysis of influencing factors for recurrent fractures after vertebroplasty for osteoporotic vertebral compression fracture[J]. J Minim Invasive Med, 2020, 15(4): 433−436, 445. DOI: 10.11864/j.issn.1673.2020.04.05.[9] Lee I, Budiawan H, Moon JY, et al. The value of SPECT/CT in localizing pain site and prediction of treatment response in patients with chronic low back pain[J]. J Korean Med Sci, 2014, 29(12): 1711−1716. DOI: 10.3346/jkms.2014.29.12.1711. [10] 王中兴, 王睿. 早期与延迟经皮椎体后凸成形术治疗老年椎体压缩性骨折的疗效及1年随访比较[J]. 中国现代手术学杂志, 2018, 22(5): 366−370. DOI: 10.16260/j.cnki.1009-2188.2018.05.010.
Wang ZX, Wang R. Comparison of efficacy and long-term follow-up results between early and delayed percutaneous kyphoplasty for vertebral compression fractures in the elderly[J]. Chin J Mod Oper Surg, 2018, 22(5): 366−370. DOI: 10.16260/j.cnki.1009-2188.2018.05.010.[11] 林玉江, 杨利民, 杨健. 放射性核素骨显像对骨质疏松性椎体压缩骨折诊断定位的应用[J]. 实用医学杂志, 2017, 33(3): 408−411. DOI: 10.3969/j.issn.1006-5725.2017.03.020.
Lin YJ, Yang LM, Yang J. Application of radionuclide bone imaging in diagnosis and localization of osteoporotic vertebral compressive fracture[J]. J Pract Med, 2017, 33(3): 408−411. DOI: 10.3969/j.issn.1006-5725.2017.03.020.[12] 孟庆龙, 宋少莉. 99Tcm-二膦酸盐及18F-NaF动态骨显像的机制及临床应用[J]. 中华核医学与分子影像杂志, 2019, 39(1): 53−61. DOI: 10.2967/jnumed.112.114298.
Meng QL, Song SL. Dynamic bone imaging with 99Tcm-labeled diphosphonates and 18F-NaF: mechanisms and applications[J]. Chin J Nucl Med Mol Imaging, 2019, 39(1): 53−61. DOI: 10.2967/jnumed.112.114298.[13] 王善容, 丁月云, 石德道, 等. SPECT/CT与MRI对新鲜和陈旧性骨质疏松性椎体压缩骨折的鉴别价值[J]. 青岛大学学报: 医学版, 2018, 54(6): 647−651, 655. DOI: 10.11712/jms201806005.
Wang SR, Ding YY, Shi DD, et al. Value of single photon emission computed tomography/computed tomography versus magnetic resonance imaging in the differential diagnosis of fresh and old osteoporotic vertebral compression fracture[J]. J Qingdao Univ: Med Sci, 2018, 54(6): 647−651, 655. DOI: 10.11712/jms201806005.[14] Li YB, Zheng X, Wang R, et al. SPECT-CT versus MRI in localizing active lesions in patients with osteoporotic vertebral compression fractures[J]. Nucl Med Commun, 2018, 39(7): 610−617. DOI: 10.1097/MNM.0000000000000857. [15] Damgaard M, Nimb L, Madsen JL. The role of bone SPECT/CT in the evaluation of lumbar spinal fusion with metallic fixation devices[J]. Clin Nucl Med, 2010, 35(4): 234−236. DOI: 10.1097/RLU.0b013e3181d18cdd. [16] 林玉江, 林勇, 王德春, 等. 单光子发射计算机断层显像/CT在脊柱外科精准诊断定位应用中的临床问题分析[J]. 中国组织工程研究, 2019, 23(12): 1915−1920. DOI: 10.3969/j.issn.2095-4344.1129.
Lin YJ, Lin Y, Wang DC, et al. Clinical problems of single photon emission computed tomography/CT applied in accurate diagnosis and location of spinal surgery[J]. Chin J Tissue Eng Res, 2019, 23(12): 1915−1920. DOI: 10.3969/j.issn.2095-4344.1129.[17] Lin X, Xiong D, Peng YQ, et al. Epidemiology and management of osteoporosis in the People's Republic of China: current perspectives[J]. Clin Interv Aging, 2015, 10: 1017−1033. DOI: 10.2147/CIA.S54613. [18] Yang DH, Zhang YL, Ma X, et al. Resources utilisation and economic burden of percutaneous vertebroplasty or percutaneous kyphoplasty for treatment of osteoporotic vertebral compression fractures in China: a retrospective claim database study[J/OL]. BMC Musculoskelet Disord, 2020, 21(1): 255[2020-10-22]. https://bmcmusculoskeletdisord.biomedcentral.com/articles/10.1186/s12891-020-03279-1. DOI: 10.1186/s12891-020-03279-1. [19] Park SY, Lee SH, Suh SW, et al. Usefulness of MRI in determining the appropriate level of cement augmentation for acute osteoporotic vertebral compression fractures[J]. J Spinal Disord Tech, 2013, 26(3): E80−E85. DOI: 10.1097/BSD.0b013e318261f438. [20] 陈前程. 骨质疏松性椎体压缩骨折SPECT-CT及MRI的对比分析[J]. 河北医学, 2019, 25(4): 539−542. DOI: 10.3969/j.issn.1006-6233.2019.04.004.
Chen QC. Comparative analysis of SPECT-CT and MRI in osteoporotic vertebral compression fractures[J]. Hebei Med, 2019, 25(4): 539−542. DOI: 10.3969/j.issn.1006-6233.2019.04.004. -





 下载:
下载: