-
心肌是人体内代谢最旺盛的组织之一,它可利用葡萄糖、脂肪酸、乳酸及酮体等多种底物产生ATP,满足细胞的能量需求。各种底物的利用占比受多种因素的影响,在空腹状态下,心肌细胞以脂肪酸代谢为主,而餐后在糖负荷状态下则以葡萄糖代谢为主。心肌代谢的异常改变与多种心脏疾病相关,如心肌缺血和心力衰竭等[1]。因此,评价心肌代谢状态对于心脏疾病的诊断、评估和治疗策略的制定均具有重要的作用和临床价值。放射性核素心肌代谢显像作为一种无创性诊断方法,在评价心肌能量代谢方面具有独特的优势[2-3]。它通过放射性核素标记心肌细胞能量代谢底物进行显像,辅以量化分析以评价心肌细胞的代谢状态。由于临床常用的正电子核素多为机体组成元素的同位素,如11C、13N、15O、18F等,其标记物能真正反映或模拟人体内的生化代谢过程,且PET具有图像分辨率高,可以动态、定量测量等优势,因此,正电子核素显像剂在临床及科研中的应用非常广泛。目前,根据临床用途可将正电子核素心肌代谢显像剂分为氧代谢显像剂、糖代谢显像剂和脂肪酸代谢显像剂[4]。
-
心肌所需的能量主要依赖于底物的有氧代谢,无氧代谢的占比极低。心肌耗氧量(myocardial oxygen consumption,MVO2)是目前公认的定量测量心肌能量消耗的“金标准”之一,用以评估心脏能量消耗的总量。Kudomi等[5]开发了一种新的方法,使用15O-O2可同步测定左、右心室的MVO2,目前已完成了健康受试者试验,这为不同病理生理状态下MVO2的测定提供了参考。15O-O2能够测定MVO2,且15O半衰期短(T1/2=2 min),可以进行连续多次测定,但需要配备在线回旋加速器,其广泛应用受到一定限制[6]。
目前,临床上常用11C-乙酸盐评价心肌的氧代谢情况,可用于心衰和心肌缺血的诊断[7]。11C-乙酸盐进入心肌细胞后通过三羧酸循环最终转化为11C-CO2和水,由于氧化磷酸化与三羧酸循环的紧密耦合,因此11C-acetate的清除速率近似于MVO2[8],且不受血糖水平和能量代谢底物的影响。通常受检者在静息状态下经静脉注射11C-乙酸盐,采用列表模式进行图像采集,所得数据经软件分析得到心肌氧代谢速率(如Kmono、K1、K2等参数),使用Kmono和K2参数计算MVO2,K1参数计算心肌血流量[9],即一次显像可分别评价心肌的血流和代谢情况。Shi等[10]利用11C-乙酸盐评价酒精性心脏病和高危人群的心肌氧代谢水平,结果表明,重度饮酒组和酒精性心脏病组的MVO2[(0.121±0.018) mL·g−1·min−1和(0.111±0.017) mL·g−1·min−1]明显低于健康对照组和中度饮酒组[(0.144±0.023) mL·g−1·min−1和(0.146±0.027) mL·g−1·min−1,P<0.01]。虽然11C-乙酸盐的物理半衰期较短(T1/2=20 min),但制备工艺简单,现在普遍采用固相萃取技术,校正产率可达80%[11],在一定程度上能够满足临床需要,但同样要求临床机构配备加速器。
-
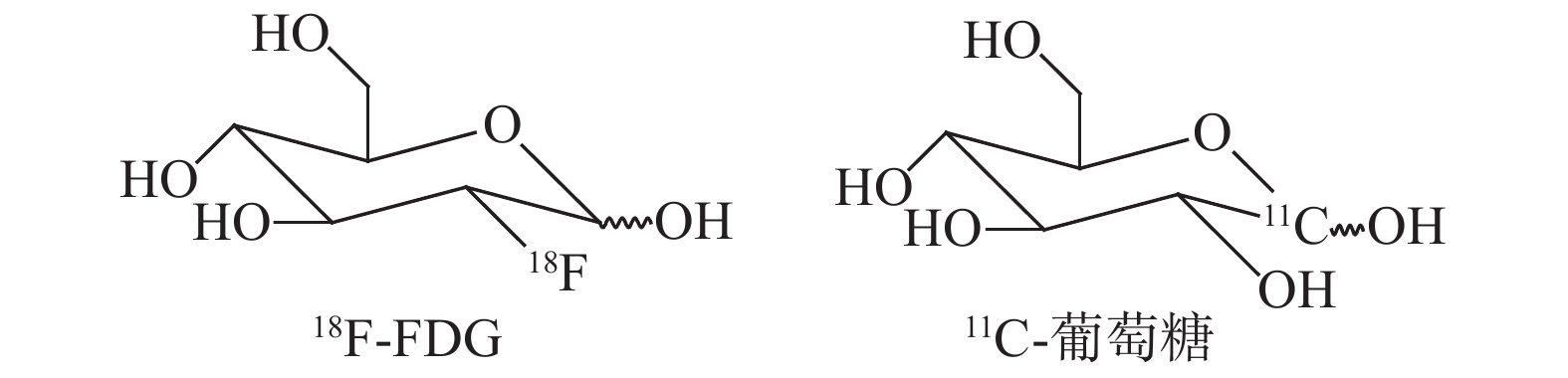
葡萄糖是心肌细胞除脂肪酸以外的另一种重要能量来源。18F-FDG是天然葡萄糖类似物,在临床上通过PET测定组织中葡萄糖的代谢情况来评价心肌细胞活力[12]。18F-FDG心肌代谢显像是目前公认的检测心肌存活的“金标准”,检查时通常采用口服葡萄糖联合静脉注射胰岛素的方法调控血糖水平,同时要避免饮食和药物对图像质量的影响[13]。对于冠心病合并糖尿病的患者需要严格调控血糖水平,其中口服葡萄糖剂量是影响图像质量的关键因素[14]。在临床中通常采用心肌灌注显像和(或)心肌代谢显像评价心肌活性,即灌注-代谢不匹配表示心肌存活;灌注-代谢相匹配表示心肌无活性,这对于指导临床血运重建及评价预后有重要意义[15]。
11C-葡萄糖的C-1位是11C,由于是同位素取代,其体内代谢过程与葡萄糖完全一致。与18F-FDG相比,11C-葡萄糖能够全面反映机体的糖代谢情况:摄取、氧化、糖酵解和糖原化,但由于制备过程较繁琐[16],物理半衰期短,且诊断效果与18F-FDG相比并无明显优势[17],目前11C-葡萄糖多用于科研。糖代谢显像剂的结构式见图1。
-
脂肪酸的氧化代谢是心肌细胞的重要能量来源,机体主要利用油酸和棕榈酸在细胞质中活化,其后转运到线粒体内进行β氧化产生能量。关于脂肪酸代谢显像剂的研究报道很多,根据其代谢特点分为“代谢清除型”和“捕获型”[18]。
-
代谢清除型显像剂是以放射性核素标记内源性脂肪酸,其在体内可参与脂肪酸代谢的全过程,可用来评价脂肪酸的摄取、氧化和存储。既往采用单光子核素标记,如123I-对碘苯基十五烷酸(123I-iodophenylpentadecanoci acid,123I-IPPA),123I半衰期长(T1/2=13.2 h),适合临床应用,但由于SPECT时间分辨率和空间分辨率较低,图像质量相对较差,以及123I供给受限等原因,现多采用正电子核素标记[19]。11C-棕榈酸是一种经典的PET心肌代谢显像剂,经心肌细胞摄取后快速清除[20],能够真实反映机体的脂肪酸代谢情况。11C-棕榈酸制备方法成熟[21],但是目前临床应用相对较少,多用于脂肪酸代谢相关的实验研究[22]。18F半衰期长(T1/2=108 min),可以区域配送,便于临床推广,早期开发的显像剂有18F-17-氟-十七烷酸(18F-FHA)和18F-16-氟-十六烷酸(18F-FHDA),二者代谢过程与11C-棕榈酸类似,但体内稳定性差,存在一定的脱氟现象。Tu等[23]报道了一种结构与IPPA类似,采用18F标记的显像剂15-(4-(2-18F-氟乙氧基)苯基)十五烷酸[15-(4-(2-18F- fluoroethoxy)phenyl)pentadecanoic acid,18F-F7)。动物实验结果表明,18F-F7在小鼠心肌中摄取明显,代谢方式与11C-棕榈酸一致,均为双相清除,但早期清除相速率明显减低,后期清除相速率加快,体内稳定性好,无明显脱氟现象。18F-F7现已进行人体试验阶段,有望进入临床应用。此外,随着68Ge/68Ga发生器的普及,研究人员尝试采用68Ga标记的脂肪酸用于PET心肌代谢显像,初步动物实验结果表明,其在小鼠心肌中快速摄取,但靶向性较差,心/血比值不超过0.5,尚需进一步研究[24]。多种脂肪酸代谢清除型显像剂的结构式见图2。
-
捕获型显像剂通过在脂肪酸的碳链上引入硫原子或增加支链,阻碍了脂肪酸的β氧化进程,从而将显像剂“捕获”在线粒体内并不断累积,因此捕获型显像剂的图像质量优于代谢清除型显像剂,但也存在不足,其只能反映脂肪酸的摄取和氧化过程。DeGrado等[25-26]开发了一系列18F标记的硫代长链脂肪酸显像剂:18F-14-氟-6-硫-十七烷酸(14-18F-fluoro-6-thia-heptadecanoic acid,18F-FTHA)、18F-16-氟-4-硫-棕榈酸(16-18F-fluro-4-thia-palmitate,18F-FTP)和18F-18-氟-4-硫-油酸(18-18F-fluro-4-thia-oleate,18F-FTO),其中18F-FTHA和18F-FTP为棕榈酸类似物,18F-FTO为油酸类似物。18F-FTHA的临床应用广泛,Ohira等[27]利用18F-FDG联合18F-FTHA显像评价肺动脉高压患者的心肌代谢情况,结果表明,肺动脉压升高与右心室18F-FDG/18F-FTHA的摄取比值增加有关;Labbé等[28]给予患者口服18F-FTHA进行显像评价糖尿病患者的脂肪酸代谢情况,研究结果表明,糖耐量异常患者心肌摄取脂肪酸增加与心功能障碍相关。Savisto等[29]开发了18F-FTHA自动化制备方法,但制备时比活度不宜过高,因为18F产生的γ射线可能导致18F-FTHA的碳链中硫原子键断裂,降低产品的放射化学纯度[30]。Shoup等[31]报道了18F-9-氟-3,4-亚甲基十七烷酸(9-18F-fluoro-3,4-methyleneheptadecanoic acid,18F-FCPHA)显像剂,该显像剂的C-3和C-4位上甲基支链形成环丙基阻碍β氧化,大鼠显像实验结果显示该显像剂的图像质量良好[32]。目前18F-FCPHA已进入临床试验阶段,其主要用于评价心肌缺血[33]。18F标记的脂肪酸显像剂普遍存在脱氟现象,Cai等[34]对18F-FTO进行结构修饰,在碳链末端引入三唑杂环,修饰后虽然降低了体内脱氟,但心脏摄取也随之降低。除18F外,Wu等[35]还应用11C标记甲基-16-硫代棕榈酸(11C-methyl-16-thiopalmitic acid,11C-MTPA),11C-MTPA是在碳链末端引入硫原子,动物实验结果表明,其在小鼠心肌具有相对较长的滞留时间。多种脂肪酸捕获型显像剂的结构式见图3。
-
综上所述,正电子核素标记的显像剂可以从氧代谢、糖代谢和脂肪酸代谢等方面评价心肌代谢情况,目前临床上应用最多的是18F-FDG,结合心肌灌注显像可以明确心肌是否存活,但患者接受检查时需要调节血糖,检查流程相对复杂,且一项小范围的研究结果表明,11C-acetate的阳性预测值和阴性预测值均优于18F-FDG(89%和73% vs. 65%和57%,P<0.025)[36],而11C-acetate受半衰期所限,难以在临床上广泛推广。因此,脂肪酸代谢显像剂是当前研究的主要方向,其中18F-FTHA等已在临床应用,多种新型的显像剂处于早期研发阶段,但要进入临床还需要大量的研究和实践[37]。脂肪酸的氧化代谢是心肌的最主要能量来源,全面、准确评价心肌脂肪酸代谢情况将有助于多种心脏疾病的诊断和治疗[38],尤其适合于糖尿病和肥胖患者。2种类型的脂肪酸代谢显像剂各具优势,代谢清除型显像剂可全面评价脂肪酸的摄取、氧化和储存,而捕获型显像剂的特点是图像质量更好,但不能区分氧化和储存途径。从目前的研究成果来看,18F标记的长链脂肪酸将是主要研究方向之一[39],但需要注意显像剂体内脱氟的问题,可以参照18F-F7的结构设计代谢清除型显像剂,在近羧基端引入硫原子,在远端的苯环上进行18F标记。此外,68Ga标记的脂肪酸用于心肌代谢显像有一定的可行性,这也为业界提供了新的研究思路。当前关于正电子核素心肌代谢显像剂的研究正在不断开展,未来还需继续深入研究[40]。
利益冲突 本研究由署名作者按以下贡献声明独立开展,不涉及任何利益冲突。
作者贡献声明 李帅负责观点的提出、文献的查阅、综述的撰写;李剑明负责综述的审阅与修订。
正电子核素心肌代谢显像剂的研究进展
Research progress of positron radionuclide myocardial metabolism imaging agents
-
摘要: 心肌细胞利用葡萄糖、脂肪酸、乳酸及酮体等多种底物产生能量,以维持自身的正常舒缩功能。心肌细胞能量代谢的异常改变与多种心脏疾病相关,如心肌缺血和心力衰竭等。放射性核素显像作为一种无创性功能检查方法,能够用于心肌细胞代谢状况的评价。放射性核素心肌代谢显像剂是由放射性核素标记的心肌代谢底物及其类似物,在临床上分为氧代谢显像剂、糖代谢显像剂和脂肪酸代谢显像剂。笔者就近年来有关正电子核素心肌代谢显像剂的研究进展进行综述。Abstract: Cardiomyocytes use various substrates such as glucose, fatty acids, lactic acid, and ketone bodies to produce energy to maintain their normal systolic and diastolic function. Abnormal changes in cardiomyocytes' energy metabolism are associated with various heart diseases, such as myocardial ischemia and heart failure. As a non-invasive functional examination method, radionuclide imaging can be used to evaluate the metabolism status of cardiomyocytes. Radionuclide myocardial metabolism imaging agents are myocardial metabolism substrates. Their analogues are labeled with radionuclides, divided into oxygen metabolism imaging agents, glucose metabolism imaging agents, and fatty acid metabolism imaging agents. This paper reviews the research progress of positron radionuclide myocardial metabolism imaging agents in recent years.
-
Key words:
- Radionuclide imaging /
- Positron imaging agent /
- Myocardial metabolism
-
[1] Zhou B, Tian R. Mitochondrial dysfunction in pathophysiology of heart failure[J]. J Clin Invest, 2018, 128(9): 3716−3726. DOI: 10.1172/JCI120849. [2] Angelidis G, Giamouzis G, Karagiannis G. SPECT and PET in ischemic heart failure[J]. Heart Fail Rev, 2017, 22(2): 243−261. DOI: 10.1007/s10741-017-9594-7. [3] Salata BM, Singh P. Role of cardiac PET in clinical practice[J]. Curr Treat Options Cardiovasc Med, 2017, 19(12): 93. DOI: 10.1007/s11936-017-0591-x. [4] Gropler RJ. Recent advances in metabolic imaging[J]. J Nucl Cardiol, 2013, 20(6): 1147−1172. DOI: 10.1007/s12350-013-9786-z. [5] Kudomi N, Kalliokoski KK, Oikonen VJ, et al. Myocardial blood flow and metabolic rate of oxygen measurement in the right andleftventricles at rest and during exercise using 15O-labeled compounds and PET[J/OL]. Front Physiol, 2019, 10: 741[2020-02-24]. https://www.frontiersin.org/articles/10.3389/fphys.2019.00741/full. DOI: 10.3389/FPHYS.2019.00741. [6] Cockburn N, Corsaut J, Kovacs MS, et al. Validation protocol for current good manufacturing practices production of [15O] water for hybrid PET/MR studies[J]. Nucl Med Commun, 2020, 41(10): 1100−1105. DOI: 10.1097/MNM.0000000000001249. [7] Nielsen R, Møller N, Gormsen LC, et al. Cardiovascular effects of treatment with the ketone body 3-hydroxybutyrate in chronic heart failure patients[J]. Circulation, 2019, 39(18): 2129−2141. DOI: 10.1161/CIRCULATIONAHA.118.036459. [8] Grassi I, Nanni C, Allegri V, et al. The clinical use of PET with 11C-acetate[J/OL]. Am J Nucl Med Mol Imaging, 2012, 2(1): 33−47 [2020-02-24]. https://pubmed.ncbi.nlm.nih.gov/23133801. [9] Wu KY, Dinculescu V, Renaud JM, et al. Repeatable and reproducible measurements of myocardial oxidative metabolism, blood flow and external efficiency using 11C-acetate PET[J]. J Nucl Cardiol, 2018, 25(6): 1912−1925. DOI: 10.1007/s12350-018-1206-y. [10] Liu S, Lin X, Shi X, et al. Myocardial tissue and metabolism characterization in men with alcohol consumption by cardiovascular magnetic resonance and 11C-acetate PET/CT[J]. Cardiovasc Magn Reson, 2020, 22(1): 23. DOI: 10.1186/s12968-020-00614-2. [11] Le Helleix S, Dollé F, Kuhnast B. Easy upgrade of the TRACERLab FX C Pro for [11C]carboxylation reactions: application to the routine production of [1-11C]acetate[J]. Appl Radiat Isot, 2013, 82: 7−11. DOI: 10.1016/j.apradiso.2013.06.020. [12] Bucerius J, Hyafil F, Verberne HJ, et al. Position paper of the Cardiovascular Committee of the European Association of Nuclear Medicine (EANM) on PET imaging of atherosclerosis[J]. Eur J Nucl Med Mol Imaging, 2016, 43(4): 780−792. DOI: 10.1007/s00259-015-3259-3. [13] 姜婧晨, 王雪梅, 张凯秀. 18F-FDG PET/CT心肌代谢显像图像质量影响因素的研究进展[J]. 国际放射医学核医学杂志, 2020, 44(2): 114−118. DOI: 10.3760/cma.j.issn.1673-4114.2020.02.008.
Jiang JC, Wang XM, Zhang KX. Current status of studies on factors affecting myocardial metabolism imaging quality of 18F-FDG PET/CT[J]. Int J Radiat Med Nucl Med, 2020, 44(2): 114−118. DOI: 10.3760/cma.j.issn.1673-4114.2020.02.008.[14] 朱紫薇, 常智, 史晓鹏, 等. 合并和不合并糖尿病的冠心病患者18F-FDG PET/CT心肌代谢图像质量及其影响因素[J]. 中华核医学与分子影像杂志, 2020, 40(5): 281−287. DOI: 10.3760/cma.j.cn321828-20191012-00231.
Zhu ZW, Chang Z, Shi XP, et al. 18F-FDG PET/CT images quality and its impact factors in diabetic and non-diabetic patients with coronary artery disease[J]. Chin J Nucl Med Mol Imaging, 2020, 40(5): 281−287. DOI: 10.3760/cma.j.cn321828-20191012-00231.[15] 孙茉茉, 李剑明, 刘志刚. 冠状动脉旁路移植术前13N-NH3/18F-FDG PET显像检测冬眠心肌的临床研究[J]. 中国医学影像技术, 2018, 34(7): 1003−1008. DOI: 10.13929/j.1003-3289.201709005.
Sun MM, Li JM, Liu ZG. Clinical study of 13N-NH3/18F-FDG in detecting hibernating myocardium before coronary artery bypass grafting[J]. Chin J Med Imaging Technol, 2018, 34(7): 1003−1008. DOI: 10.13929/j.1003-3289.201709005.[16] Dence CS, Powers WJ, Welch MJ. Improved synthesis of 1-[11C]D-glucose[J]. Appl Radiat Isot, 1993, 44(6): 971−980. DOI: 10.1016/0969-8043(93)90053-d. [17] Herrero P, Sharp TL, Dence C, et al. Comparison of 1-11C-glucose and 18F-FDG for quantifying myocardial glucose use with PET[J]. J Nucl Med, 2002, 43(11): 1530−1541. [18] van de Weijer T, Paiman EHM, Lamb HJ. Cardiac metabolic imaging: current imaging modalities and future perspectives[J]. J Appl Physiol, 2018, 124(1): 168−181. DOI: 10.1152/japplphysiol.01051.2016. [19] Knapp FF Jr, Kropp J. Iodine-123-labelled fatty acids for myocardial single-photon emission tomography: current status and future perspectives[J]. Eur J Nucl Med, 1995, 22(4): 361−381. DOI: 10.1007/bf00941855. [20] Christensen NL, Jakobsen S, Schacht AC, et al. Whole-body biodistribution, dosimetry, and metabolite correction of [11C]palmitate: a PET tracer for imaging of fatty acid metabolism[J]. Mol Imaging, 2017, 16: 1−9. DOI: 10.1177/1536012117734485. [21] Amor-Coarasa A, Kelly JM, Babich JW. Synthesis of [11C]palmitic acid for PET imaging using a single molecular sieve 13X cartridge for reagent trapping, radiolabeling and selective purification[J]. Nucl Med Biol, 2015, 42(8): 685−690. DOI: 10.1016/j.nucmedbio.2015.03.008. [22] Son NH, Basu D, Samovski D, et al. Endothelial cell CD36 optimizes tissue fatty acid uptake[J]. J Clin Invest, 2018, 128(10): 4329−4342. DOI: 10.1172/JCI99315. [23] Tu ZD, Li SH, Sharp TL, et al. Synthesis and evaluation of 15-(4-(2-[18F]fluoroethoxy) phenyl) pentadecanoic acid: a potential PET tracer for studying myocardial fatty acid metabolism[J]. Bioconjug Chem, 2010, 21(12): 2313−2319. DOI: 10.1021/bc100343h. [24] Jain A, Mathur A, Pandey U, et al. 68Ga labeled fatty acids for cardiac metabolic imaging: influence of different bifunctional chelators[J]. Bioorg Med Chem Lett, 2016, 26(23): 5785−5791. DOI: 10.1016/j.bmcl.2016.10.048. [25] DeGrado TR, Wang SY, Holden JE, et al. Synthesis and preliminary evaluation of 18F-labeled 4-thia palmitate as a PET tracer of myocardial fatty acid oxidation[J]. Nucl Med Biol, 2000, 27(3): 221−231. DOI: 10.1016/s0969-8051(99)00101-8. [26] DeGrado TR, Bhattacharyya F, Pandey MK, et al. Synthesis and preliminary evaluation of 18-18F-fluoro-4-thia-oleate as a PET probe of fatty acid oxidation[J]. J Nucl Med, 2010, 51(8): 1310−1317. DOI: 10.2967/jnumed.109.074245. [27] Ohira H, DeKemp R, Pena E, et al. Shifts in myocardial fatty acid and glucose metabolism in pulmonary arterial hypertension: a potential mechanism for a maladaptive right ventricular response[J]. Eur Heart J Cardiovasc Imaging, 2016, 17(12): 1424−1431. DOI: 10.1093/ehjci/jev136. [28] Labbé SM, Grenier-larouche T, Noll C, et al. Increased myocardial uptake of dietary fatty acids linked to cardiac dysfunction in glucose-intolerant humans[J]. Diabetes, 2012, 61(11): 2701−2710. DOI: 10.2337/DB11-1805. [29] Savisto N, Viljanen T, Kokkomäki E, et al. Automated production of [18F]FTHA according to GMP[J]. J Labelled Comp Radiopharm, 2018, 61(2): 84−93. DOI: 10.1002/jlcr.3589. [30] Pandey MK, Jacobson MS, Groth EK, et al. Radiation induced oxidation of [18F]fluorothia fatty acids under cGMP manufacturing conditions[J]. Nucl Med Biol, 2020, 80/81: 13−23. DOI: 10.1016/j.nucmedbio.2019.11.004. [31] Shoup TM, Elmaleh DR, Bonab AA, et al. Evaluation of trans-9-18F-fluoro-3,4-methyleneheptadecanoic acid as a PET tracer for myocardial fatty acid imaging[J]. J Nucl Med, 2005, 46(2): 297−304. [32] Gropler RJ. PET radiotracers of the cardiovascular system[J]. PET Clin, 2009, 4(1): 69−87. DOI: 10.1016/j.cpet.2009.06.001. [33] Demeure F, Cerqueira MD, Hesse M, et al. A new F-18 labeled PET tracer for fatty acid imaging[J]. J Nucl Cardiol, 2015, 22(2): 391−394. DOI: 10.1007/s12350-014-0012-4. [34] Cai ZX, Mason NS, Anderson CJ, et al. Synthesis and preliminary evaluation of an 18F-labeled oleic acid analog for PET imaging of fatty acid uptake and metabolism[J]. Nucl Med Biol, 2016, 43(1): 108−115. DOI: 10.1016/j.nucmedbio.2015.08.005. [35] Wu XX, Wang PZ, Liu RX, et al. Development of 11C-labeled ω-sulfhydryl fatty acid tracer for myocardial imaging with PET[J]. Eur J Med Chem, 2018, 143: 1657−1666. DOI: 10.1016/j.ejmech.2017.10.062. [36] Khalaf S, Chamsi-Pasha M, Al-Mallah MH. Assessment of myocardial viability by PET[J]. Curr Opin Cardiol, 2019, 34(5): 466−472. DOI: 10.1097/HCO.0000000000000652. [37] Taillefer R, Harel F. Radiopharmaceuticals for cardiac imaging: current status and future trends[J]. J Nucl Cardiol, 2018, 25(4): 1242−1246. DOI: 10.1007/s12350-018-1194-y. [38] Mather KJ, DeGrado TR. Imaging of myocardial fatty acid oxidation[J]. Biochim Biophys Acta, 2016, 1861(10): 1535−1543. DOI: 10.1016/j.bbalip.2016.02.019. [39] Werner RA, Chen XY, Rowe SP, et al. Recent paradigm shifts in molecular cardiac imaging-establishing precision cardiology through novel 18F-labeled PET radiotracers[J]. Trends Cardiovasc Med, 2020, 30(1): 11−19. DOI: 10.1016/j.tcm.2019.02.007. [40] Bois JP, Gropler RJ, Peterson LR. Contemporary advances in myocardial metabolic imaging and their impact on clinical care: a focus on positron emission tomography (PET)[J]. Curr Cardiovas Imaging Rep, 2018, 11(2): 5. DOI: 10.1007/s12410-018-9444-6. -






 下载:
下载: