-
颞骨的恶性肿瘤发病率极低,仅为1/10万~6/10万,其中以外耳道最常见,中耳及内耳更为少见[1]。内淋巴囊肿瘤(endolymphatic sac tumor,ELST)是起源于内耳的低度恶性肿瘤,较为罕见,起病隐匿,生长缓慢。ELST位于部位较深的侧颅底,周围紧邻面神经、颈内动静脉等重要神经及血管,其后方为后颅窝。因此,尽管其恶性程度较低,但肿瘤常累及桥小脑角区,较大肿瘤延伸至颈静脉球部,侵蚀静脉窦及其相关血管等结构,手术难度较大[2-3]。笔者报道了1例经病理结果证实的ELST病例,通过患者的临床表现、实验室诊断、MRI与CT检查结果,并结合相关文献,总结了其影像学表现在诊断中的应用价值。
-
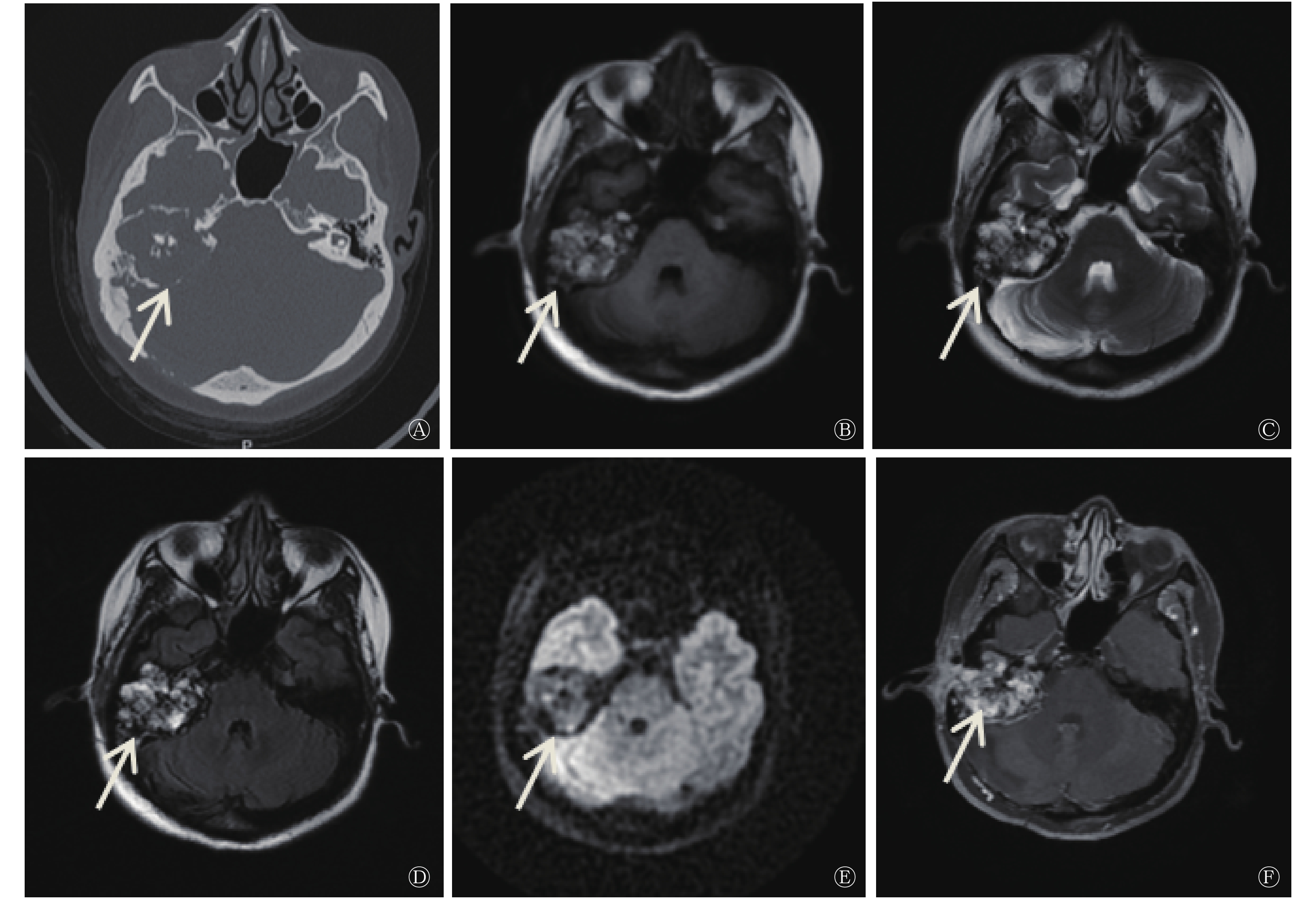
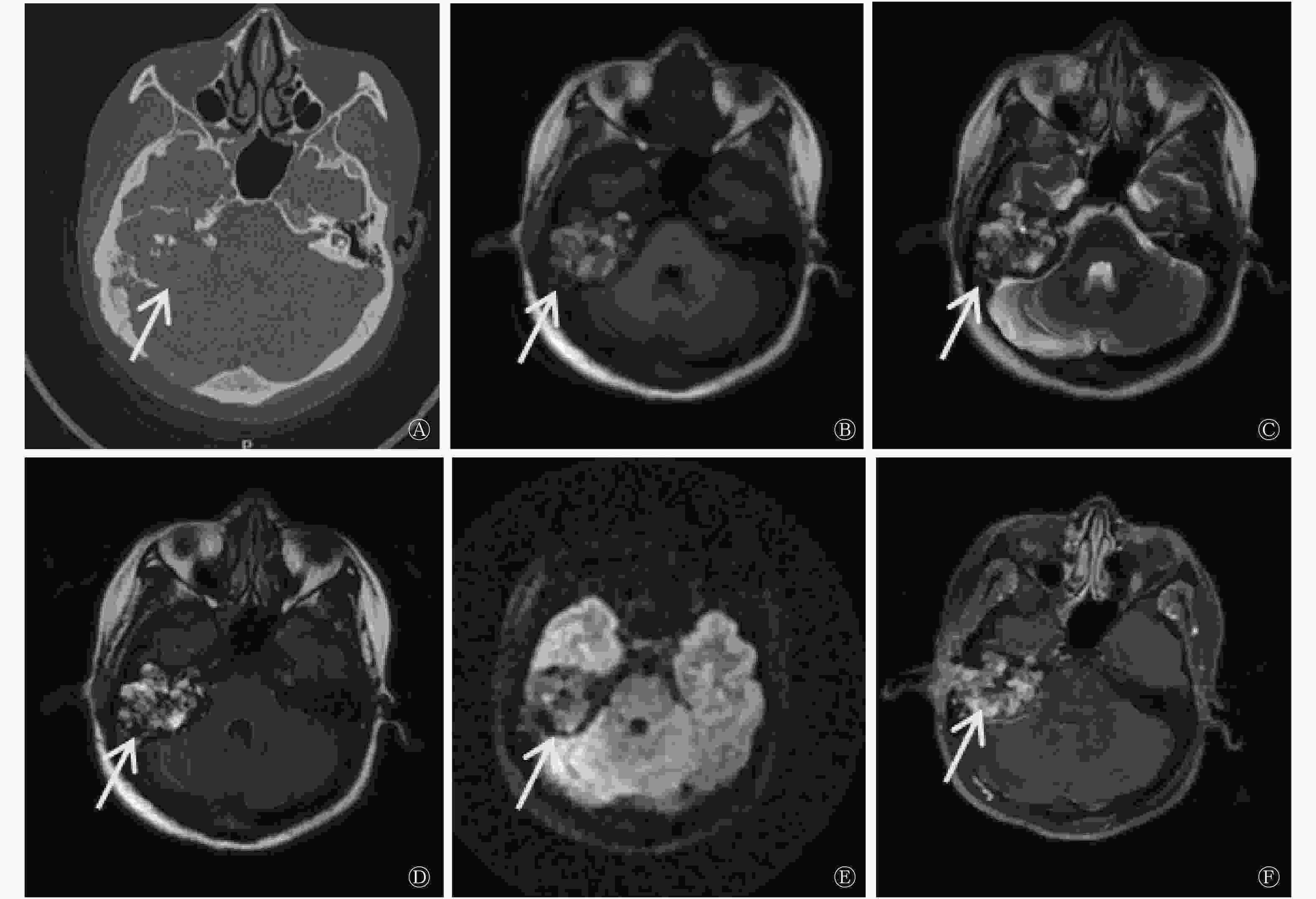
患者女性,46岁,因“右耳外耳道肿物30年、右侧面瘫28年加重”就诊。1996年患者就诊于我院耳鼻喉科,行幕下开颅囊肿探查术,病理结果提示(桥小脑角处硬膜外)孤立性骨囊肿。2018年9月12日患者右耳再次流脓流血,入院进行治疗。患者此次入院后行颞骨CT检查,CT表现为右侧内耳不规则软组织密度肿块,周围颞骨呈“蜂窝状”弥漫性溶骨性破坏,肿瘤向周围膨胀性生长,其内可见不规则钙化影,边缘见环形高密度影;累及中耳及外耳道,内耳听小骨破坏,仅见锤骨头、砧骨体部及残缺砧骨短脚;病灶累及面神经,致面神经膝部、鼓室段、乳突段骨管破坏;耳蜗外侧鼓室岬骨质局部缺如,半规管、前庭导水管及内听道骨质破坏。CT诊断提示为右侧颞骨乳突占位病变(图1)。并进行耳部MRI平扫及弥散加权成像检查,结果显示病灶T1、T2加权成像呈混杂高信号,弥散加权成像呈等低或低信号,增强扫描病灶呈明显不均匀强化,大小约为4.1cm×3.7cm,邻近脑膜受累呈线样强化。MRI诊断提示为右侧中耳、内耳区占位性病变,考虑ELST可能性大(图1)。根据患者主诉、体征及各项辅助检查结果,临床诊断为ELST,右侧周围性完全性面瘫,右耳极重度感音神经性耳聋。决定行右侧ELST切除术、右侧颞骨次全切除术治疗。术中取组织,诊断结果为(右侧颞骨)形态符合ELST。免疫组化结果:广谱细胞角蛋白(AE1/AE3)(+)、上皮膜抗原(+)、波形蛋白(+)、CK8/18(+)、甲状腺转录因子(−)、甲状腺球蛋白(−)、胶质纤维酸性蛋白(−)、细胞增殖指数Ki-67(阳性1%)、细胞特异激活蛋白(+)。术后患者达到临床治愈,可以出院。ELST易复发,嘱患者定期复查,长期观察病情变化。
-
ELST是由Hassard等[4]发现的起源于内耳内淋巴囊的肿瘤。1989年Heffner等[5]对20例ELST患者的综合分析发现,患者颞骨有一致性的组织学改变。内淋巴囊位于颞骨岩部后方的前庭导水管外口处,主要功能是监测内淋巴的体积和压力。内淋巴囊可分为近侧段及远侧段两部分,近侧段走行于岩骨中后缘的骨性凹陷切迹内,被认为是ELST的发生部位。ELST分为散发型和遗传型,遗传型ELST常合并希-林病(von Hippel-Lindau diesease,VHL),VHL是第3号染色体短臂上的肿瘤支持基因失活,是常染色体遗传性疾病。据文献报道,10%~15%的VHL患者会发生ELST,其中30%为双侧发病[6]。ELST好发于成人,平均年龄40岁,年龄跨度较大。
ELST生长缓慢,随着疾病的进展,肿瘤可向内侧延伸至桥小脑角,向外累及中耳甚至外耳,向上延伸至中颅窝,向下延伸至中颅底,向前外累及海绵窦、内听道及面神经管,向后侵犯颅后窝等,引起周围组织破坏,但肿瘤淋巴结转移可能性非常小,远处转移文献报道少见。ELST临床表现主要取决于肿瘤的大小和生长方向,以单侧听力损失最为常见,主要为进行性感音神经性耳聋、持续不断且高调耳鸣、眩晕、颅神经受累等,少数病例表现为突聋,此时病情多已发展为重度。由于肿瘤生长部位较深,周围毗邻面神经,因此面神经多受累,表现为面肌无力或面瘫。此外,第Ⅸ~Ⅻ对颅神经也可因受累表现出相应的症状[7]。
ELST影像学表现具有一定特点[8-9],CT表现为颞骨岩部软组织密度肿块,呈浸润性生长,内有点状、针状钙化,直径≤3 cm的肿瘤通常集中在颞骨岩部后方,靠近内淋巴囊部位;而最大径>3 cm的肿瘤扩散至邻近区域,引起相应的临床表现。MRI结果显示,绝大部分ELST T2加权成像呈高信号,T1加权成像呈等高或高信号,部分接近小脑白质。肿瘤边缘见环形高信号,增强扫描呈明显强化。ELST由颈内动脉、咽升动脉及小脑前后动脉等供血。在本病例中,ELST最大径>3 cm,其影像学表现与文献[8-9]报道结果相符。
ELST为低级别腺癌,肿瘤生长方式多样,可见乳头状、实性、滤泡状或囊性结构[10]。肿瘤细胞通常单层排列,呈乳头状、管状;囊性腺管样结构的腺腔内可见粉染胶样分泌物,与甲状腺肿瘤相似,浸润性生长并破坏周围骨质。乳头或腺腔被覆单层立方或柱状上皮细胞,细胞质丰富,核分裂像罕见;间质为富于血管的大量增生的纤维结缔组织,灶区淋巴细胞浸润及含铁血黄素沉积,部分区域可见少量死骨。韩冬艳等[11]研究结果显示,ELST免疫染色组织检测为波形蛋白、广谱细胞角蛋白和上皮膜抗原呈弥漫阳性,胶质纤维酸性蛋白、突触素表达不定,甲状腺球蛋白和甲状腺转录因子表达呈阴性,增殖细胞核抗原Ki-67值不高[12]。本病例与该文献报道一致。
ELST需要与颈静脉区生长的肿瘤相鉴别。(1)颈静脉球瘤。其位于颈静脉孔区富血供的实性肿块,起源于颈静脉球和鼓室体副神经节,起源部位低于ELST,肿瘤常膨胀性生长,侵入颈静脉孔区;颈静脉球瘤MRI典型的影像学表现为盐-胡椒征。(2)颈静脉孔神经鞘瘤。部分学者将神经鞘瘤分为4型,即A型位于颅内,较少扩展入颈静脉孔;B型位于颈静脉孔,并扩展入颅内;C型位于颅外,扩展入颈静脉孔区;D型同时侵犯颅内外,呈哑铃状,即哑铃型或称颅内外沟通型[13]。ELST主要与B型神经鞘瘤相鉴别,神经鞘瘤多见于40岁以上女性,肿瘤以颈静脉孔神经部为中心,颈静脉窝扩大,肿块呈长T1长T2信号,增强扫描呈明显均匀或不均匀强化。(3)颈静脉孔区脑膜瘤。肿块以宽基底与脑膜相连,并沿脑膜生长,常引起相邻骨组织增生硬化或轻度吸收破坏,增强扫描呈明显强化,并见“脑膜尾征”,颈静脉孔扩大不明显。
尽管ELST发病率极低,但对于发生在颞骨内淋巴囊区域的肿块,CT检查发现骨质明显破坏,肿块内出现钙化,MRI T2加权成像呈明显不均性高信号,增强扫描呈明显强化时,高度提示ELST。CT和MRI对其诊断、鉴别诊断及确定疾病范围具有很高价值。
利益冲突 本研究由署名作者按以下贡献声明独立开展,不涉及任何利益冲突。
作者贡献声明 韩冰负责论文的撰写与修订;张瑜、岳光红负责病例与文献的收集;周及红负责论文的审核与校对;刘东负责方案的提出与设计、论文的审阅。
内淋巴囊肿瘤术后20年复发影像学诊断一例
A case of imaging diagnosis of 20-year recurrence of endolymphatic sac tumor
-
摘要: 笔者报道了1例行次全切术后复发的内淋巴囊肿瘤病例,且初次诊断为乳头状汗腺瘤,分析其CT及MRI特点、临床表现和病理形态,并复习相关文献,重点总结其影像学表现,旨在提高影像医师及临床医师对该病的认识。Abstract: This paper reports a case of recurrent endolymphatic sac tumor after subtotal resection, which was initially diagnosed as papillary sweat adenoma. The CT and MRI characteristics, clinical manifestations and pathological morphology of the tumor were analyzed, and the relevant literature was reviewed. The imaging manifestations were mainly summarized in order to improve the understanding of the tumor by radiologists and clinicians.
-
Key words:
-
[1] 史珣贝, 戴春富. 颞骨恶性肿瘤临床诊疗的现状[J]. 中华耳科学杂志, 2019, 17(3): 311−316. DOI: 10.3969/j.issn.1672-2922.2019.03.007.
Shi JB, Dai CF. Current opinions on clinical diagnosis and treatment of temporal bone malignancy[J]. Chin J Otology, 2019, 17(3): 311−316. DOI: 10.3969/j.issn.1672-2922.2019.03.007.[2] 程乐, 戴艳红, 徐新运. 内淋巴囊肿瘤临床、影像、病理和免疫组化分析[J]. 医学影像学杂志, 2012, 22(6): 1043−1045. DOI: 10.3969/j.issn.1006-9011.2012.06.058.
Cheng L, Dai YH, Xu XY. The clinical, radiological, pathological and immunohistochemical features of endolymphatic sac tumors[J]. J Med Imaging, 2012, 22(6): 1043−1045. DOI: 10.3969/j.issn.1006-9011.2012.06.058.[3] Alkhotani A, Butt B, Khalid M, et al. Endolymphatic sac tumor at the cerebellopontine angle: a case report and review of literature[J]. Int J Surgery Case Reports, 2019, 58: 162−166. DOI: 10.1016/j.ijscr.2019.04.032. [4] Hassard AD, Boudreau SF, Cron CC. Adenoma of the endolymphatic sac[J]. J Otolaryngol, 1984, 13(4): 213−216. [5] Heffner DK. Low-Grade adenocarcinoma of probable endolymphatic sac origin. A clinicopathologic study of 20 cases[J]. Cancer, 1989, 64(11): 2292−2302. DOI: 10.1002/1097-0142(19891201)64:11<2292::aid-cncr2820641119>3.0.co;2-#. [6] 郝瑾, 许丽萍, 鲜军舫, 等. 内淋巴囊瘤的临床和VHL基因突变分析研究[J]. 中华耳科学杂志, 2018, 16(5): 651−658. DOI: 10.3969/j.issn.1672-2922.2018.05.012.
Hao J, Xu LP, Xian JF, et al. Clinical and VHL gene mutation analysis of endolymphatic sac tumor[J]. Chin J Otology, 2018, 16(5): 651−658. DOI: 10.3969/j.issn.1672-2922.2018.05.012.[7] 岳云龙, 陈孝柏, 金延方. 内淋巴囊肿瘤的影像学表现(附两例报告并文献复习)[J]. 临床放射学杂志, 2007, 26(9): 869−871. DOI: 10.3969/j.issn.1001-9324.2007.09.007.
Yue YL, Chen XB, Jin YF. Imaging manifestations of endolymphatic sac tumor (with two reports and literature review)[J]. J Clin Radiology, 2007, 26(9): 869−871. DOI: 10.3969/j.issn.1001-9324.2007.09.007.[8] Jackler RK, Driscoll CLW. Tumors of the ear and temporal bone[M]. Philadelphia: Lippincott Williams and Wilkins, 2000: 156–171. [9] Lo WW, Applegate LJ, Carberry JN, et al. Endolymphatic sac tumors: radiologic appearance[J]. Radiology, 1993, 189(1): 199−204. DOI: 10.1148/radiology.189.1.8372194. [10] Mendenhall WM, Suárez C, Skálová A, et al. Current treatment of endolymphatic sac tumor of the temporal bone[J]. Adv Ther, 2018, 35(7): 887−898. DOI: 10.1007/s12325-018-0730-0. [11] 韩冬艳, 付慧君, 何燕燕, 等. 内淋巴囊肿瘤临床病理分析及文献复习[J]. 诊断学理论与实践, 2018, 17(6): 711−714. DOI: 10.16150/j.1671-2870.2018.06.016.
Han DY, Fu HJ, He YY, et al. Clinicopathological analysis and literature review of endolymphatic sac tumor[J]. J Diagn Concept Pract, 2018, 17(6): 711−714. DOI: 10.16150/j.1671-2870.2018.06.016.[12] 傅海燕, 王家耀. 内淋巴囊肿瘤四例临床病理观察及鉴别诊断[J]. 中华肿瘤防治杂志, 2014, 21(19): 1553−1556. DOI: 10.16073/j.cnki.cjcpt.2014.19.017.
Fu HY, Wang JY. Clinicopathological observation and differential diagnosis of four cases of endolymphatic sac tumor[J]. Chin J Cancer Prevent Treat, 2014, 21(19): 1553−1556. DOI: 10.16073/j.cnki.cjcpt.2014.19.017.[13] Andrade NN, Mathai PC, Kamil R, et al. Inflammatory myofibroblastic tumour: a case report and a clinical update[J]. J Oral Biol Craniofac Res, 2017, 7(3): 219−222. DOI: 10.1016/j.jobcr.2017.09.005. -





 下载:
下载: