-
前列腺癌(prostate cancer,PCa)是男性常见的恶性肿瘤,且90%以上的癌症病灶发生在外周带[1-3]。随着我国快速步入老龄化社会,PCa的发病率也呈上升趋势,但在临床诊断工作中,PCa的MRI诊断仍是一个难点。T2加权成像(T2-weighted imaging,T2WI)具有观察前列腺解剖结构的优势,通过前列腺外周带高信号衬托,病变在T2WI上呈相对稍低信号,提示病变存在的可能。基于水分子高斯分布的弥散加权成像(diffusion-weighted imaging,DWI)是一种反映水分子布朗运动的高灵敏成像技术,通过观察水分子运动受限情况,可以灵敏地间接提示病变的存在及其性质。目前的研究认为,DWI所用b值越高,越有可能获得真实的水分子弥散情况,从而提升对病变诊断的可靠性[1-3]。本研究旨在探讨超高b值的DWI联合T2WI技术无创性诊断外周带PCa的临床应用价值。
-
回顾性分析2018年12月1日至2019年10月1日于佛山市第一人民医院临床疑诊前列腺病变患者41例,年龄49~89岁,中位年龄69岁。所有入组患者均于检查前签署了知情同意书。
纳入标准:临床疑诊前列腺病变患者,完成超声引导下前列腺靶点穿刺、临床病理学确诊,并于穿刺前后1个月内完成前列腺常规MRI及超高b值DWI序列检查。排除标准:穿刺过程导致前列腺局部出血较多,明显影响病灶评估及MRI图像伪影明显影响评估的患者。
-
采用美国GE公司生产的Discovery MR 750w 3.0T MRI仪及16通道相控阵腹部表面线圈完成MRI扫描。所有患者均完成盆部T2WI和b值分别为2000、3000 s/mm2的DWI序列成像。
T2WI序列:采用快速自旋回波(FSE)序列。脉冲序列重复时间/回波时间为3180 ms/90 ms,激发次数为2,层厚4 mm,无间距,视野均为320 mm×320 mm。
DWI序列:采用单次激发平面回波成像(SS-EPI)序列。b值分别取2000、3000 s/mm2;脉冲序列重复时间/回波时间为3000 ms/98 ms,激发次数为12、15,层厚4 mm,无间距,视野均为400 mm×400 mm。
-
参考2016版前列腺穿刺中国专家共识[4],采用直肠内超声引导经会阴前列腺10+X穿刺法完成穿刺。
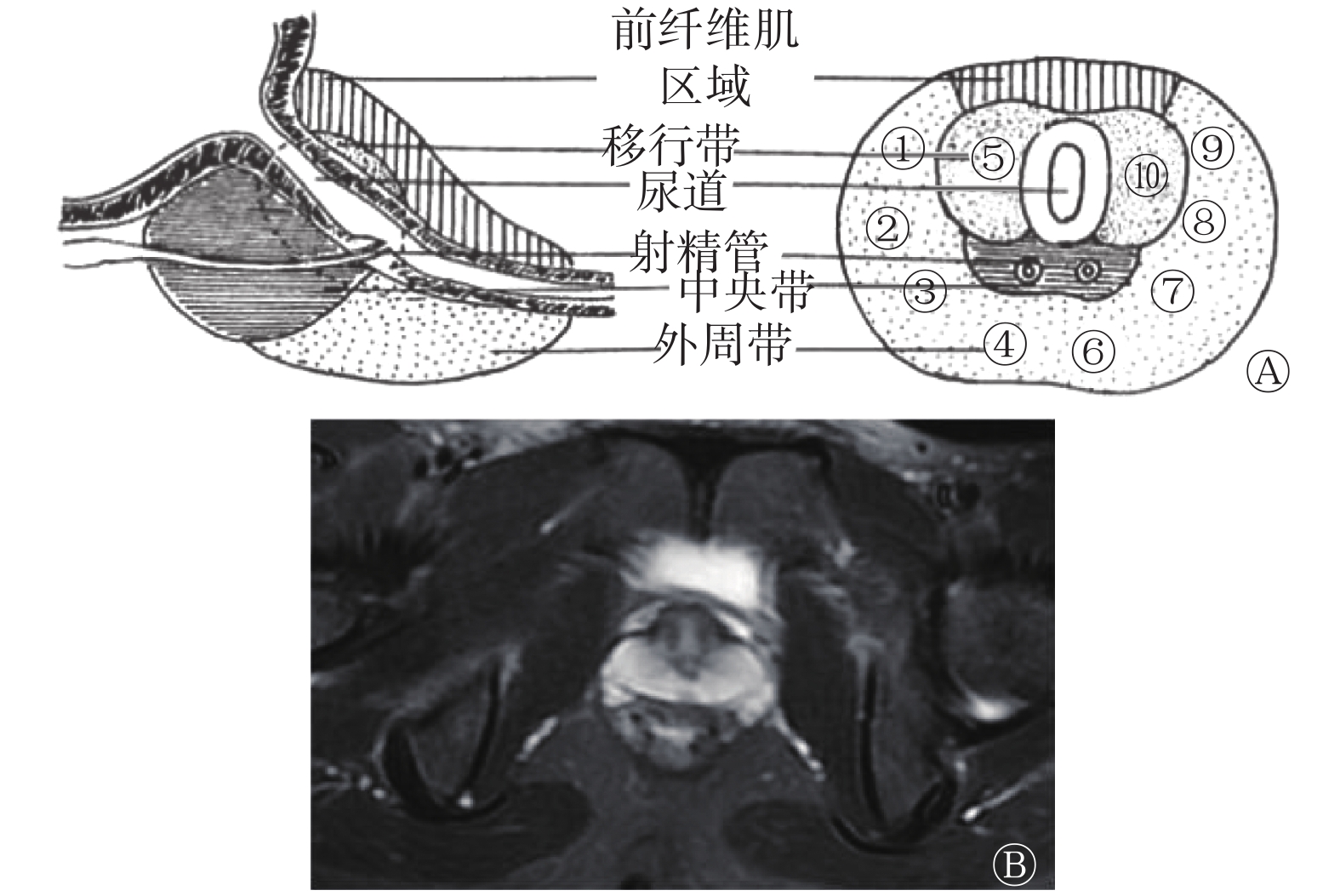
患者取截石位,自行向上牵拉阴囊,充分暴露会阴部。常规消毒后行局部麻醉。采用10+X穿刺法进行穿刺,即分别于前列腺两侧外周带前部(右①左⑨)、外侧部(右②左⑧)、中部(右③左⑦)、后部(右④左⑥)及两侧移行区(右⑤左⑩)各穿1针,共穿刺10针(图1)。对超声或MRI报告可疑区域增加1针(X针)。取出组织按顺序编号,标本用10%甲醛溶液固定,行病理学检查。
-
在MRI图像上,把前列腺外周带分为右侧和左侧的前部、外侧部、中部、后部及两侧移行区,分别与穿刺针位置对应(图1)。考虑到穿刺的局限性,仅把中央腺体区域肿瘤的尿道周围病变纳入研究。
-
参考PCa MRI检查和诊断共识(第二版)[1]中的相关序列图像的判断方法和标准。由两位有5年以上诊断经验的副主任医师采用双盲法在仪器自带的ADW 4.6工作站上对图像进行分析评价。若诊断意见不一致,协商后采用统一意见。
轴位T2WI图像上外周带低信号提示可能为癌症病灶。当T2WI图像外周带未发现低信号时,评为0分;有低信号时,评为1分。
轴位DWI图像上外周带弥散受限高信号提示可能为癌症病灶。当DWI图像外周带未发现高信号时,评为0分;有高信号时,评为1分。
以靶点穿刺病理学结果为“金标准”,评估T2WI、DWI(b=2000 s/mm2)、DWI(b=3000 s/mm2)、T2WI+DWI(b=2000 s/mm2)、T2WI+DWI(b=3000 s/mm2)对PCa诊断的灵敏度、特异度和准确率。
-
应用SPSS20.0软件进行统计学分析。采用ROC曲线分析计算各方法诊断PCa的AUC。P<0.05为差异有统计学意义。
-
41例患者中,PCa患者26例(通过临床结合穿刺点位置确诊为外周带PCa),良性前列腺增生患者15例。前列腺超高b值DWI序列及T2WI序列图例见图2。前列腺外周带T2WI序列出现低信号、DWI(b=2000 s/mm2)、DWI(b=3000 s/mm2)序列出现高信号的例数分别为34、30、27,阳性率分别为82.92%(34/41)、73.17%(30/41)和65.85%(27/41)。
-
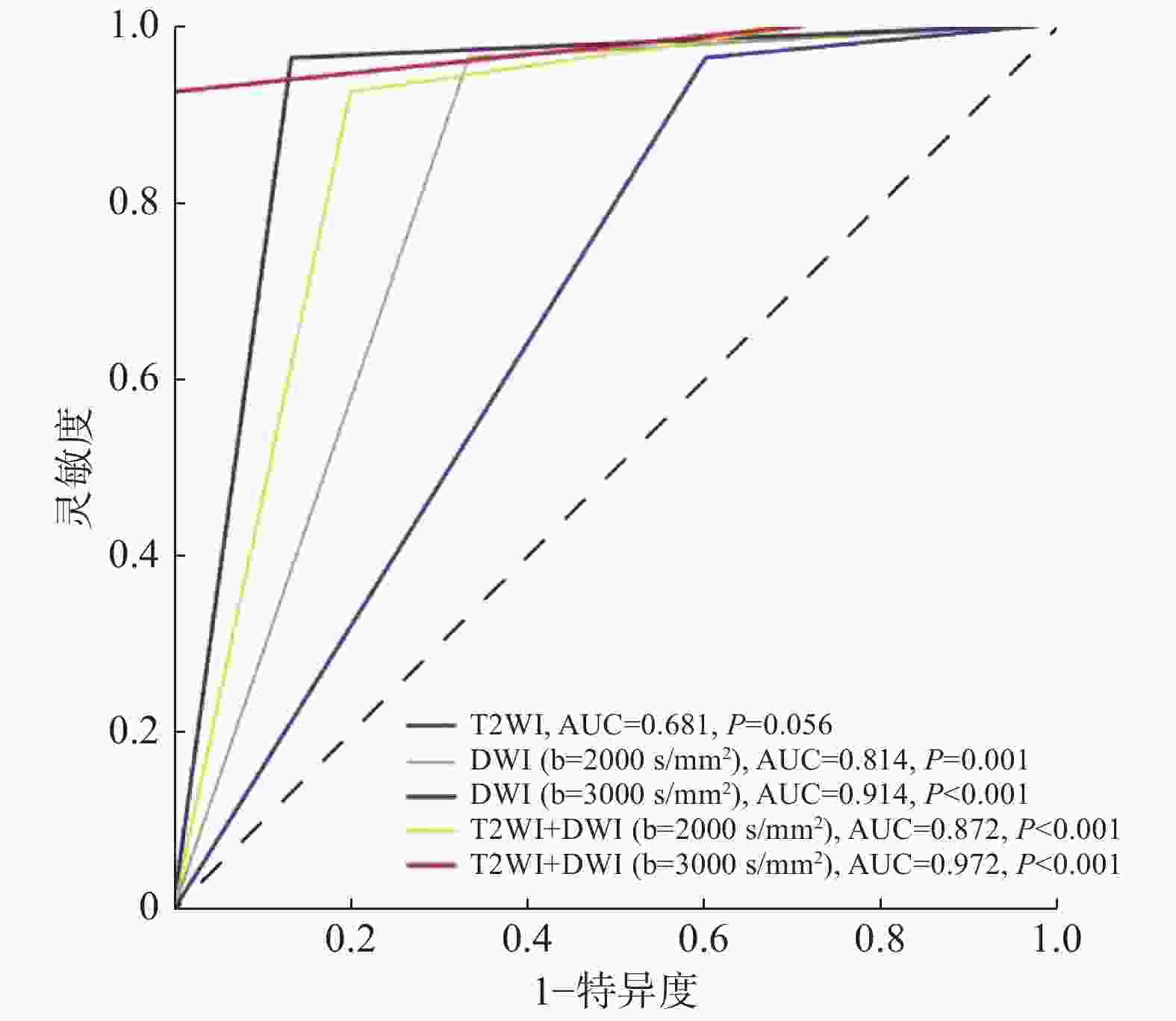
各序列或其组合对PCa的诊断效能详见表1。T2WI、DWI(b=2000 s/mm2)、DWI(b=3000 s/mm2)序列对PCa诊断的灵敏度一致,均为0.962;但T2WI序列对PCa诊断的特异度较低(0.400);DWI(b=3000 s/mm2)序列对PCa诊断的特异度和准确率均高于DWI(b=2000 s/mm2);T2WI+DWI(b=3000 s/mm2)序列对PCa诊断的特异度和准确率最高,分别为1.000和0.975,该序列ROC的AUC为0.972(图3)。
序列 灵敏度 特异度 准确率 T2WI 0.962(25/26) 0.400(6/15) 0.756(31/41) DWI
(b=2000 s/mm2)0.962(25/26)
0.667(10/15)
0.854(35/41)
DWI
(b=3000 s/mm2)0.962(25/26)
0.867(13/15)
0.926(38/41)
T2WI+DWI
(b=2000 s/mm2)0.923(24/26)
0.800(12/15)
0.878(36/41)
T2WI+DWI
(b=3000 s/mm2)0.923(24/26)
1.000(15/15)
0.951(39/41)
注:表中,T2WI:T2加权成像;DWI:弥散加权成像 表 1 T2WI、DWI各序列和两者组合对前列腺癌的诊断效 能(n=41)
Table 1. Diagnostic efficiency of T2-weighted imaging and DWI sequences and their combination in prostate cancer (n=41)
-
目前,MRI被认为是检查前列腺疾病的最佳方法[1],对发现早期恶性病变、观察病变侵犯范围、临床分期和随访等具有重要价值[5-7]。临床工作中,T2WI是观察前列腺解剖结构的最佳序列[1],且在评价PCa患者的精囊和包膜受侵、淋巴结情况等方面有明显优势。在T2WI图像上,外周带PCa通常在外周带正常组织高信号的衬托下表现为稍低信号,而T2WI脂肪抑制序列图像有利于进一步简化判断扫描区域的图像信号构成。本研究结果显示,T2WI对PCa的检出具有灵敏度高(0.962)、特异度低(0.400)的特点,这主要是因为多种其他前列腺病变(如增生结节、前列腺炎等)也可表现为T2WI或T2WI脂肪抑制序列图像稍低信号。因此,T2WI对部分PCa的准确判断仍然存在困难,必须联合其他成像序列,以提高MRI对PCa诊断的特异度。
DWI可以灵敏地反映组织内部水分子扩散运动的差异,从而反映组织结构的改变。随着b值的增大,水分子扩散信号的衰减逐渐偏离线性,DWI的弥散权重越大,T2穿透效应和对血流灌注效应的影响越小。超高b值的DWI主要反映组织的整体扩散不均匀性,且组织结构越复杂,非正态分布水分子扩散受限越显著。可见,b值是影响DWI的重要参数。临床经验表明,b值越大,图像信噪比越低,并可能影响对解剖结构的识别[8-9]。我们认为,对于前列腺疾病,DWI序列中b值的选择应至少满足以下3个条件:①能清晰显示和分辨被检组织及其内部结构;②有效避免T2穿透和微循环灌注效应;③尽可能选择高b值,且扫描时间能被绝大多数受检者接受,从而避免出现移动伪影。
过去,国内外大多数前列腺病变DWI的b值为500~1000 s/mm2[10-15],对PCa的诊断准确率为62%~76%[10, 14-15],仍有较大提升空间。在临床实践中,b≤1000 s/mm2及以下者,受T2穿透效应影响明显,PCa、炎症及增生等病变在低b值DWI上均表现为高信号,导致癌症病灶的假阳性率高。因此,2018年PCa MRI检查和诊断共识[1]建议DWI的b值应≥1400 s/mm2。故本研究未对b<2000 s/mm2的DWI图像进行比较研究。但前列腺疾病DWI研究中最佳b值的选择至今尚无统一意见[1]。部分学者尝试采用超高b值(b=3000 s/mm2)行前列腺DWI,但所得结果不一。张扬贵等[15]认为,b=2000 s/mm2较b=3000 s/mm2的DWI对PCa的诊断具有更高的灵敏度和特异度(93.0%对82.6%、76.9%对73.4%)。Rosenkrantz等[16]也认为,前列腺DWI的b值选择不建议>2500 s/mm2。而张琨等[14]、Zhang等[17]和我们均认为,与b=2000 s/mm2比较,b=3000 s/mm2为前列腺疾病DWI的最优选择。
我们研究发现,b=2000 s/mm2与b=3000 s/mm2的DWI对PCa诊断的灵敏度一致(均为0.962),但b=3000 s/mm2的特异度及准确率均高于b=2000 s/mm2者(0.867对0.667、0.926对0.854)。因此我们推测,DWI(b=3000 s/mm2)可能比DWI(b=2000 s/mm2)进一步减少了T2穿透效应及微循环血流灌注效应的干扰,增加了局部病理状态下扩散受限的水分子与周围组织的对比,在保证图像具有足够信噪比(空间分辨率)的条件下,更容易突显病灶,从而获得更好的诊断效能。可见,对前列腺增生结节等良性病变与癌症病灶的鉴别,b=3000 s/mm2的DWI可能更具优势。
此外,本研究对b=2000 s/mm2与b=3000 s/mm2的DWI分别采用12次和15次激励次数,均获得了良好的图像质量,未出现因图像扭曲变形等质量问题而影响解读的情况。将二者分别联合T2WI图像,其在PCa诊断中的ROC的AUC分别为0.872、0.972,与既往低b值DWI研究结果[10, 14-15]对比,明显提高了对PCa诊断的特异度和准确率,在鉴别PCa与前列腺增生等病变上有一定的优势。而b=3000 s/mm2的DWI联合T2WI序列更具优势,与张琨等[18]的研究结果类似。
本研究不足之处:①超声引导下靶点穿刺活检有假阴性的可能,导致入组患者有假阴性PCa存在的可能;②本研究按时间顺序选取一年内行超声引导下前列腺穿刺确诊的患者,入组患者和流行病学分布情况基本一致,部分患者确诊时已是外周带PCa晚期患者,早期、细小PCa病灶患者相对较少,缺乏中央带PCa患者,有待增加这部分患者行进一步研究;③本研究未对超高b值图像质量对诊断效能的影响进行评估,有待进一步优化扫描参数后,结合不同b值和其他机型深入研究;④表观弥散系数(apparent diffusion coefficient,ADC)去除了T2穿透效应的干扰,能更客观地反映组织中水分子的扩散特性,而我们没有做ADC的定量分析比较,主要是由于ADC的量化影响因素较多,例如:取超高b值的DWI,水分子扩散运动偏离了假设条件下的正态分布,是否需要优化ADC的算法?我们正在就此设计进一步研究。
综上所述,3.0T超高b值的DWI可用于PCa的诊断和鉴别诊断,且b=3000 s/mm2的DWI联合T2WI序列对PCa的诊断具有很高的准确率,有望为需要行进一步诊断的前列腺疾病患者提供一种可靠性高的无创性检查方法。
利益冲突 本研究由署名作者按以下贡献声明独立开展,不涉及任何利益冲突。
作者贡献声明 刘健萍负责研究方法的建立、论文的撰写;贺小红、高明勇负责研究方法的指导、论文的审阅;金亚彬负责数据的统计学处理;林胜强负责数据的测量;李斌负责患者的收集。
超高b值弥散加权联合T2加权序列诊断外周带前列腺癌的价值
Value of ultra-high b-value diffusion-weighted imaging combined with T2-weighted imaging in the diagnosis of peripheral prostate cancer
-
摘要:
目的 探讨超高b值弥散加权成像(DWI)联合T2加权成像(T2WI)诊断外周带前列腺癌(PCa)的临床应用价值。 方法 选取2018年12月1日至2019年10月1日在佛山市第一人民医院行超声引导下前列腺靶点穿刺、临床病理学确诊并于穿刺前后1个月内行前列腺MRI检查的PCa患者41例,年龄49~89岁,中位年龄69岁。所有患者均行3.0T超高b值(分别为2000、3000 s/mm2)的DWI及T2WI脂肪抑制序列MRI成像。以前列腺靶点穿刺病理学结果为“金标准”,分别计算T2WI、DWI(b=2000 s/mm2)、DWI(b=3000 s/mm2)、T2WI+DWI(b=2000 s/mm2)、T2WI+DWI(b=3000 s/mm2)对PCa的诊断灵敏度、特异度和准确率。采用受试者工作特征(ROC)曲线分析计算各方法诊断PCa的曲线下面积。 结果 41例患者中,PCa患者26例(通过临床结合穿刺点位置确诊为外周带PCa),良性前列腺增生患者15例。T2WI、DWI(b=2000 s/mm2)、DWI(b=3000 s/mm2)、T2WI+DWI(b=2000 s/mm2)、T2WI+DWI(b=3000 s/mm2)诊断PCa的灵敏度分别为0.962(25/26)、0.962(25/26)、0.962(25/26)、0.923(24/26)、0.923(24/26),特异度分别为0.400(6/15)、0.667(10/15)、0.876(13/15)、0.800(12/15)、1.000(15/15),准确率分别为0.756(31/41)、0.854(35/41)、0.926(38/41)、0.878(36/41)、0.951(39/41),ROC曲线下面积分别为0.681、0.814、0.914、0.872、0.972(P=0.056、0.001、<0.001、<0.001、<0.001)。 结论 T2WI+DWI(b=3000 s/mm2)序列图像诊断PCa具有较高的准确率,有望成为一种可靠的诊断前列腺疾病的无创性检查方法。 Abstract:Objective To investigate the clinical value of ultra-high b-value diffusion-weighted imaging (DWI) combined with T2-weighted imaging (T2WI) in the diagnosis of peripheral prostate cancer (PCa). Methods Forty-one patients who underwent ultrasound-guided prostate target puncture, clinicopathological diagnosis, and prostate MRI within one month before and after the puncture were selected from December 1, 2018 to October 1, 2019 in the First People's Hospital of Foshan. The patients' ages ranged from 49 to 89 years, with a median age of 69 years. All of the patients completed 3.0T ultra-high b-value DWI and T2WI fat suppression (2000 and 3000 s/mm2, respectively). With prostate target puncture pathology as the gold standard, the sensitivity, specificity, accuracy, and area under the receiver operating characteristic (ROC) curve were calculated for the different imaging methods in PCa diagnosis. Results Among all the 41 patients, 26 had PCa (the 26 cases were peripheral zone PCa confirmed by clinical diagnosis and puncture site location) and 15 had benign hyperplasia. The sensitivity of T2WI, DWI (b=2000 s/mm2), DWI (b=3000 s/mm2), T2WI+DWI (b=2000 s/mm2), and T2WI+DWI (b=3000 s/mm2) in PCa diagnosis was 0.962 (25/26), 0.962 (25/26), 0.962 (25/26), 0.923 (24/26), and 0.923 (24/26) respectively; the specificity was 0.400 (6/15), 0.667 (10/15), 0.876 (13/15), 0.800 (12/15), and 1.000 (15/15), respectively; the accuracy was 0.756 (31/41), 0.854 (35/41), 0.926 (38/41), 0.878 (36/41), and 0.951 (39/41), respectively; and the area under the ROC curve was 0.681, 0.814, 0.914, 0.872, and 0.972(P=0.056, 0.001, <0.001, <0.001, <0.001), respectively. Conclusions DWI (b=3000 s/mm2) combined with the T2WI image exhibited high accuracy in PCa diagnosis. It is expected to become a highly reliable noninvasive examination procedure for the diagnosis of PCa. -
表 1 T2WI、DWI各序列和两者组合对前列腺癌的诊断效 能(n=41)
Table 1. Diagnostic efficiency of T2-weighted imaging and DWI sequences and their combination in prostate cancer (n=41)
序列 灵敏度 特异度 准确率 T2WI 0.962(25/26) 0.400(6/15) 0.756(31/41) DWI
(b=2000 s/mm2)0.962(25/26)
0.667(10/15)
0.854(35/41)
DWI
(b=3000 s/mm2)0.962(25/26)
0.867(13/15)
0.926(38/41)
T2WI+DWI
(b=2000 s/mm2)0.923(24/26)
0.800(12/15)
0.878(36/41)
T2WI+DWI
(b=3000 s/mm2)0.923(24/26)
1.000(15/15)
0.951(39/41)
注:表中,T2WI:T2加权成像;DWI:弥散加权成像 -
[1] 中华放射学杂志前列腺疾病诊疗工作组, 中华放射学杂志编辑委员会. 前列腺癌MRI检查和诊断共识(第二版)[J]. 中华放射学杂志, 2018, 52(10): 743−750. DOI: 10.3760/cma.j.issn.1005−1201.2018.10.005.
Chinese Journal of Radiology Working Group on Diagnosis and Treatment of Prostate Diseases, Editorial Committee of Chinese Journal of Radiology. Consensus on MRI and diagnosis of prostate cancer (Second Edition)[J]. Chin J Radiol, 2018, 52(10): 743−750. DOI: 10.3760/cma.j.issn.1005−1201.2018.10.005.[2] Feng ZY, Min XD, Margolis DJA, et al. Evaluation of different mathematical models and different b-value ranges of diffusion-weighted imaging in peripheral zone prostate cancer detection using b-value up to 4500 s/mm2[J/OL]. PLoS One, 2017, 12(2): e0172127[2019-10-20]. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0172127. DOI: 10.1371/journal.pone.0172127. [3] 季立标, 陆志华, 姚鸿欢, 等. 超高b值扩散加权成像在前列腺癌定性诊断中的临床价值[J]. 中华医学杂志, 2017, 97(27): 2107−2110. DOI: 10.3760/cma.j.issn.0376−2491.2017.27.006.
Ji LB, Lu ZH, Yao HH, et al. Application study of qualitatively diagnosing prostate cancer using ultrahigh b-value DWI[J]. Natl Med J China, 2017, 97(27): 2107−2110. DOI: 10.3760/cma.j.issn.0376−2491.2017.27.006.[4] 中华医学会泌尿外科学分会, 中国前列腺癌联盟. 前列腺穿刺中国专家共识[J]. 中华泌尿外科杂志, 2016, 37(4): 241−244. DOI: 10.3760/cma.j.issn.1000−6702.2016.04.001.
Chinese Medical Association Urology Surgery Branch, China Prostate Cancer Alliance. Chinese expert consensus on prostate puncture[J]. Chin J Urol, 2016, 37(4): 241−244. DOI: 10.3760/cma.j.issn.1000−6702.2016.04.001.[5] Barrett T, Turkbey B, Choyke PL. PI-RADS version 2: what you need to know[J]. Clin Radiol, 2015, 70(11): 1165−1176. DOI: 10.1016/j.crad.2015.06.093. [6] Fang D, Zhao CL, Ren D, et al. Could Magnetic Resonance Imaging Help to Identify the Presence of Prostate Cancer Before Initial Biopsy? The Development of Nomogram Predicting the Outcomes of Prostate Biopsy in the Chinese Population[J]. Ann Surg Oncol, 2016, 23(13): 4284−4292. DOI: 10.1245/s10434-016-5438-2. [7] Shi CZ, Zhang D, Xiao ZY, et al. Ultrahigh b-values MRI in normal human prostate: Initial research on reproducibility and age-related differences[J]. J Magn Reson Imaging, 2017, 46(3): 801−812. DOI: 10.1002/jmri.25629. [8] Feuerlein S, Davenport MS, Krishnaraj A, et al. Computed high b-value diffusion-weighted imaging improves lesion contrast and conspicuity in prostate cancer[J]. Prostate Cancer Prostatic Dis, 2015, 18(2): 155−160. DOI: 10.1038/pcan.2015.5. [9] Vural M, Ertaş G, Onay A, et al. Conspicuity of Peripheral Zone Prostate Cancer on Computed Diffusion-Weighted Imaging: Comparison of cDWI1500, cDWI2000, and cDWI3000[J]. Biomed Res Int, 2014, 2014: 768291. DOI: 10.1155/2014/768291. [10] 王俊, 卢环, 刘少强, 等. 3.0T MR多高b值DWI对前列腺癌诊断及与Gleason分级相关性分析[J]. 实用放射学杂志, 2018, 34(5): 730−732, 739. DOI: 10.3969/j.issn.1002−1671.2018.05.021.
Wang J, Lu H, Liu SQ, et al. Diagnostic value of 3.0T MR multi high-b-value DWI in prostate cancer and its correlation with Gleason classification[J]. J Pract Radiol, 2018, 34(5): 730−732, 739. DOI: 10.3969/j.issn.1002−1671.2018.05.021.[11] 席建平, 马新. 磁共振弥散加权成像诊断联合多b值检查对前列腺癌的诊断价值[J]. 实用癌症杂志, 2018, 33(11): 1900−1903. DOI: 10.3969/j.issn.1001−5930.2018.11.047.
Xi JP, Ma X. Diagnostic Value of Magnetic Resonance Diffusion Weighted Imaging Diagnosis Combined with Multi-b Value Examination for Prostate Cancer[J]. Pract J Cancer, 2018, 33(11): 1900−1903. DOI: 10.3969/j.issn.1001−5930.2018.11.047.[12] 邱英良, 郑晓林, 邹玉坚, 等. 前列腺中央带前列腺癌与前列腺增生MRI弥散加权成像的多b值分析[J]. 中国CT和MRI杂志, 2018, 16(6): 85−88, 92. DOI: 10.3969/j.issn.1672−5131.2018.06.027.
Qiu YL, Zheng XL, Zou YJ, et al. Signal Intensity Analyzing of Multi b Values MRI in Prostatic Central Zone: Applying to Difference between Prostatic Cancer and Hyperplasia[J]. Chin J CT MRI, 2018, 16(6): 85−88, 92. DOI: 10.3969/j.issn.1672−5131.2018.06.027.[13] Ueno Y, Takahashi S, Ohno Y, et al. Computed diffusion-weighted MRI for prostate cancer detection: the influence of the combinations of b-values[J]. Br J Radiol, 2015, 88(1048): 20140738. DOI: 10.1259/bjr.20140738. [14] 张琨, 张轶伟, 郭勇, 等. 扩散加权成像诊断前列腺癌b值优化的初步探讨[J]. 实用医技杂志, 2018, 25(4): 352−355. DOI: 10.19522/j.cnki.1671−5098.2018.04.002.
Zhang K, Zhang YW, Guo Y, et al. Preliminary discussion of b value optimization of ultra-high b-value diffusion-weighted imaging in prostate cancer[J]. J Pract Med Tech, 2018, 25(4): 352−355. DOI: 10.19522/j.cnki.1671−5098.2018.04.002.[15] 张杨贵, 陈珊红, 廖文华, 等. 1.5T磁共振多高b值弥散加权成像信号强度在前列腺癌中的诊断价值[J]. 实用医学影像杂志, 2017, 18(3): 194−197. DOI: 10.16106/j.cnki.cn14−1281/r.2017.03.004.
Zhang YG, Chen SH, Liao WH, et al. The diagnostic value of 1.5T magnetic resonance multi b DWI signal intensity for prostate cancer[J]. J Pract Med Imaging, 2017, 18(3): 194−197. DOI: 10.16106/j.cnki.cn14−1281/r.2017.03.004.[16] Rosenkrantz AB, Parikh N, Kierans AS, et al. Prostate Cancer Detection Using Computed Very High b-value Diffusion-weighted Imaging: How High Should We Go?[J]. Acad Radiol, 2016, 23(6): 704−711. DOI: 10.1016/j.acra.2016.02.003. [17] Zhang K, Shen YG, Zhang X, et al. Predicting Prostate Biopsy Outcomes: A Preliminary Investigation on Screening with Ultrahigh B-Value Diffusion-Weighted Imaging as an Innovative Diagnostic Biomarker[J/OL]. PLoS One, 2016, 11(3): e0151176[2019-10-20]. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0151176. DOI: 10.1371/journal.pone.0151176. [18] 张琨, 张晓晶, 钟燕, 等. 超高b值扩散加权成像诊断前列腺中央腺体癌的价值[J]. 中华放射学杂志, 2016, 50(5): 357−361. DOI: 10.3760/cma.j.issn.1005−1201.2016.05.009.
Zhang K, Zhang XJ, Zhong Y, et al. Preliminary investigation of diagnostic value of ultra-high b-value based diffusion-weighted imaging in prostate central gland diagnosis[J]. Chin J Radiol, 2016, 50(5): 357−361. DOI: 10.3760/cma.j.issn.1005−1201.2016.05.009. -





 下载:
下载: